Long-Term Follow-Up Study of Young Adults Treated for Unilateral Complete Cleft Lip, Alveolus, and Palate by a Treatment Protocol Including Two-Stage Palatoplasty: Speech Outcomes
Article information
Abstract
Background
No consensus exists on the optimal treatment protocol for orofacial clefts or the optimal timing of cleft palate closure. This study investigated factors influencing speech outcomes after two-stage palate repair in adults with a non-syndromal complete unilateral cleft lip and palate (UCLP).
Methods
This was a retrospective analysis of adult patients with a UCLP who underwent two-stage palate closure and were treated at our tertiary cleft centre. Patients ≥17 years of age were invited for a final speech assessment. Their medical history was obtained from their medical files, and speech outcomes were assessed by a speech pathologist during the follow-up consultation.
Results
Forty-eight patients were included in the analysis, with a mean age of 21 years (standard deviation, 3.4 years). Their mean age at the time of hard and soft palate closure was 3 years and 8.0 months, respectively. In 40% of the patients, a pharyngoplasty was performed. On a 5-point intelligibility scale, 84.4% received a score of 1 or 2; meaning that their speech was intelligible. We observed a significant correlation between intelligibility scores and the incidence of articulation errors (P<0.001). In total, 36% showed mild to moderate hypernasality during the speech assessment, and 11%–17% of the patients exhibited increased nasalance scores, assessed through nasometry.
Conclusions
The present study describes long-term speech outcomes after two-stage palatoplasty with hard palate closure at a mean age of 3 years old. We observed moderate long-term intelligibility scores, a relatively high incidence of persistent hypernasality, and a high pharyngoplasty incidence.
INTRODUCTION
Although cleft lip and/or palate is the most commonly encountered craniofacial malformation, its surgical treatment and clinical management still differs vastly among treatment centres worldwide [1]. In general, the success of surgical treatment is determined by several criteria, such as fistula incidence, hearing problems, maxillary growth, and speech development. To date, the optimal timing of palate closure remains a topic of discussion. Early palatal closure likely promotes better speech development. In contrast, early closure of the hard palate is likely detrimental for mid-facial growth, as the iatrogenic scar tissue interferes with maxillary outgrowth.
Schweckendiek [2] was one of the first clinicians to perform two-stage palatoplasty in the 1950s (Marburg project). In this two-stage repair, the soft palate cleft is closed at an early age, leaving the hard palate unrepaired. The hard palate is subsequently closed at a second stage later in life, and in the Marburg project, even after the age of 12 years [3]. It was hypothesised that primary soft palate closure would benefit speech development, and that late hard palate closure would allow for normal maxillary outgrowth. Twenty-five years later, subjects treated according to Schweckendieck's protocol showed excellent maxillary and facial growth, often within the normal growth ranges [4]. However, their long-term speech results were poor [4].
In the following years, both unfavourable and satisfactory speech outcomes have been reported after delayed hard palate closure [4567]. One-stage and two-stage protocols are still used in daily practice, as hard evidence favouring one technique over the other is lacking. Comparing clinical outcomes after one-stage or two-stage closure is difficult due to the paucity of studies reporting long-term outcomes, small patient groups, the lack of prospective studies, and heterogeneity in study design leading to contradictory outcomes. So far, most studies have solely focused on the timing of hard palate repair when evaluating speech outcomes or facial growth. Other factors should, however, also be considered, including the incidence of fistulas, dental occlusion, surgical skill, and the technique used in soft palate closure. Furthermore, few studies have evaluated speech outcomes after two-stage palatoplasty in adults with complete unilateral cleft lip and palate (UCLP).
The present centre used a two-stage palatoplasty protocol for over 30 years. The aim of this study was to investigate factors affecting long-term speech outcomes after two-stage palate repair in patients with a non-syndromal complete UCLP treated at our hospital.
METHODS
Patients
As part of our standard treatment protocol, all cleft patients 17 years of age and older were invited for a final follow-up at the end of their treatment. During this follow-up, every patient was evaluated by each member of our multidisciplinary team, including a plastic surgeon, an audiologist, a speech therapist, and an ear-nose-throat (ENT) surgeon. For the present study, we selected all patients born between 1977 and 1996 with a complete UCLP (n=148). Cleft repair consisted of a two-stage palatoplasty performed by one of the two surgeons at our tertiary centre. Each patient's medical file was scanned for surgical data, medical history, and the type of cleft. Only patients with a complete UCLP, including a complete cleft of the alveolus, were considered for analysis. Patients with additional anomalies (n= 4), Simonart bands (n=1), non-Caucasian ethnicity (n=6), partial treatment elsewhere (n=34), or incomplete information regarding the timing of surgery or treatment according to a different protocol (n=25) were excluded.
Of the 78 patients who met our inclusion criteria, 52 patients eventually attended the follow-up (67%). Of the 26 patients who did not attend, 9 indicated that they were not interested in follow-up or were unable to attend. The remaining patients were lost to follow-up either due to non-response or incorrect contact details (n=17, 22%).
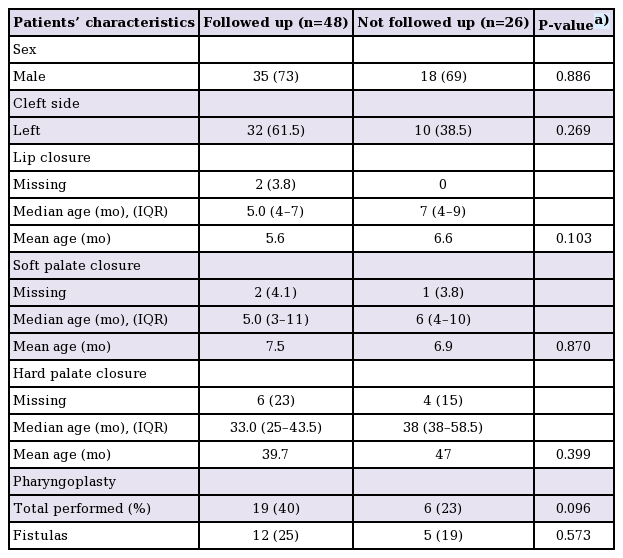
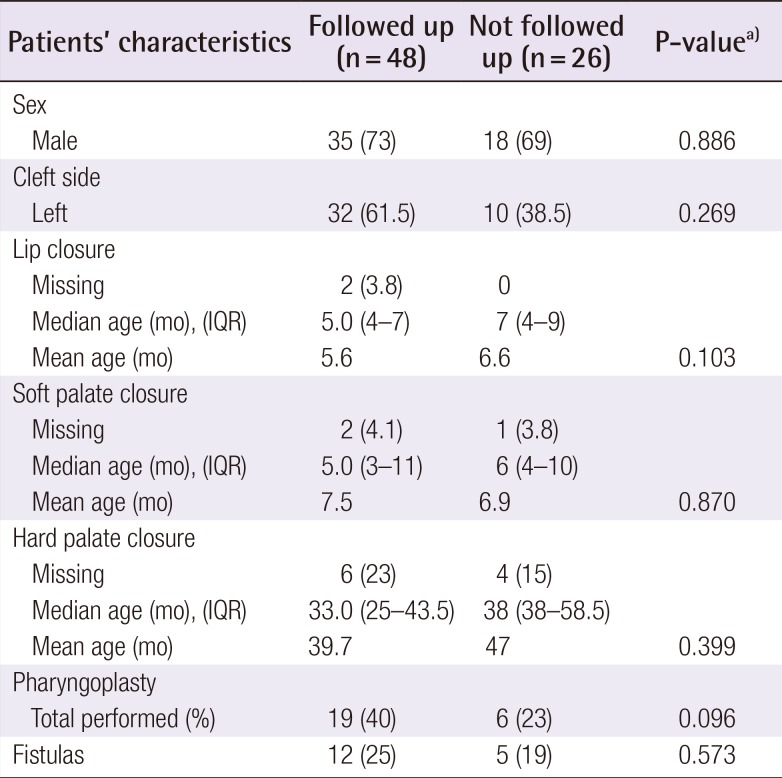
Follow-up dates were scheduled between 2008 and 2014. The patient demographics are summarized in Table 1. The mean age of the present group was 21 years (standard deviation [SD], 3.4 years). In order to assess the degree to which the patients who attended the follow-up visit were representative of the whole population, we compared clinical and treatment-related variables between patients who did or did not attend the follow-up visit. No significant differences were found regarding sex, the side of the cleft, the timing of surgery, or the percentage of patients who underwent speech-enhancing surgery (Table 1).
Treatment protocol
Surgical protocol
In the present group, surgical closure of the lip was performed at a mean age of 5.7 months (SD, 2.2 months) (Table 1). Lip closure was performed using the Millard technique and was often combined with a McComb nose correction. Soft palate closure was performed at a mean age of 7.8 months (SD, 5.8 months) using the intravelar veloplasty technique developed by Perko (described elsewhere) [6]. In this technique, 2 supraperiostal mucosal flaps are dissected towards the posterior third of the hard palate. Subsequently, the nasal mucosa is gently released from the nasal side of the maxilla and medially, without damaging the hamulus. The levator muscle is detached anteriorly, mobilized, and reconstructed into a transverse muscle sling. The nasal mucosa at the vomer is elongated using a Z-plasty, the residual musculature is closed, and the oral mucosa is elongated by V-Y plasty.
Finally, the hard palate was closed at a mean age of 40 months (3 years and 3 months; SD, 2.4 years) using the Von Langenbeck technique [8].
Orthodontic treatment
Pre-surgical orthodontic treatment was not standardly implemented. After soft palate closure, orthodontic plates were only applied if the residual cleft impeded feeding, in order to close off the residual cleft. Alveolar bone grafting was performed at the age of 11 years. Standard orthodontic treatment was started 6 months before alveolar bone grafting and was resumed at least 6 months after the surgical intervention.
Pharyngoplasty and velopharyngeal incompetence
During the course of our treatment protocol, each patient's speech was repeatedly assessed. At these assessments, velopharyngeal competence was assessed by a speech therapist using our Dutch speech assessment protocol and by a plastic surgeon and ENT specialist. Velopharyngeal competence was confirmed by nasendoscopy. In case of mild velopharyngeal incompetence (VPI), speech training focusing on improving the elevation and closure of the velum was initiated for a minimum of 3 months. In case of severe VPI or insufficient improvement after 12 months of velum training, patients were eligible for a pharyngoplasty. Pharyngoplasties were performed according to the modified Honig technique [9]. In this technique, mucoperiosteal flaps are raised and remain attached to the soft palate in a plane superficial to the greater palatine neurovascular bundle, keeping the blood supply to the maxilla intact. The soft palate is completely released from the hard palate, resulting in a push-back effect, and both flaps are sutured in a V-Y fashion along the midline. Thereafter, a superior-based pharyngeal flap is used to close the gap on the nasal side. This flap is stitched to the posterior edge of the hard palate.
Speech analysis
On the day of follow-up, speech was evaluated by one of the 3 speech and language therapists working at our centre. Speech was assessed according to the Dutch diagnostic speech assessment protocol designed for children with orofacial clefts [10]. This assessment tool is used in all Dutch cleft centres. Each speech pathologist of the cleft team in Utrecht had completed specialized training and was certified by the speech pathology working group of the Dutch Association for Cleft Palate and Craniofacial Anomalies to use this assessment tool. In order to stay certified, each speech therapist is obliged to attend annual meetings where the speech assessment is practiced.
Data collection was carried out using standard assessment forms (Supplementary Table 1). Before the start of each speech test, patients were asked about their previous speech therapy and current hearing. As impaired hearing might influence speech negatively, hearing was regularly assessed before each consultation. Audiograms were obtained by an audiologist in a sound-proof room. Out of the 52 eligible patients, only 1 patient had bilateral severe hearing loss (>40 dB) (2%, n=49) and 3 patients had a combination of mild (<40 dB) and severe (>40 dB) hearing loss (6.4%). These 4 patients were excluded from the analysis (4 of 52, 7.7%). It was not possible to retrieve the audiograms of 3 patients; however, none of them had a history of regular ENT follow-up or ENT surgery. These patients were therefore included.
Speech characteristics were evaluated by the speech therapist in the following order: resonance (subjectively and by nasometry), nasal emissions, grimaces, intelligibility, articulation, and consonant production.
First, resonance was subjectively evaluated while the patient read aloud 6 nasal, 5 oronasal, and 6 oral sentences. Resonance was scored for each sentence on a 3-point scale, as presented in detail in the supplementary material. A score of 1 was given for normal resonance, and a score of 3 for severe hypernasality or hyponasality. Resonance was also scored by nasometry. Until 2012, a NasalView System (Tiger Electronics, Seattle, WA, USA) was used for recording. Thereafter, the Nasometer II model 6450 (Kaypentax, Montvale, NJ, USA) was used. During the nasometry tests, patients were asked to read aloud validated nasal and oronasal sentences in Dutch (Supplementary Table 1) [11]. Patients' scores were compared to previously determined normal values.
Mirror tests were performed to detect nasal emissions (Supplementary Table 1). Patients were asked to read several sounds and sentences. For each air escape, speech therapists indicated which nostril the air escaped from (right, left, or bilateral) and whether the emissions were audible. While reading these sounds, the presence of turbulence was also scored.
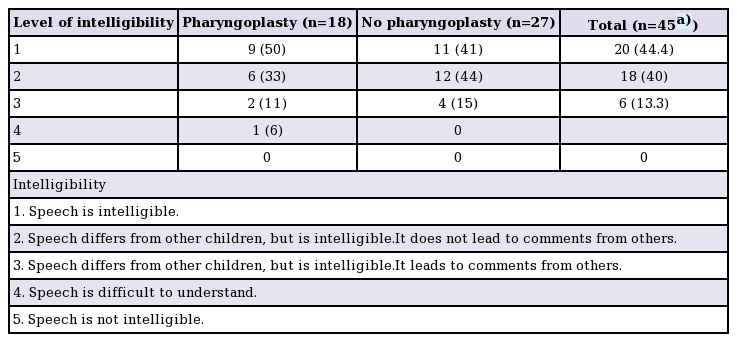
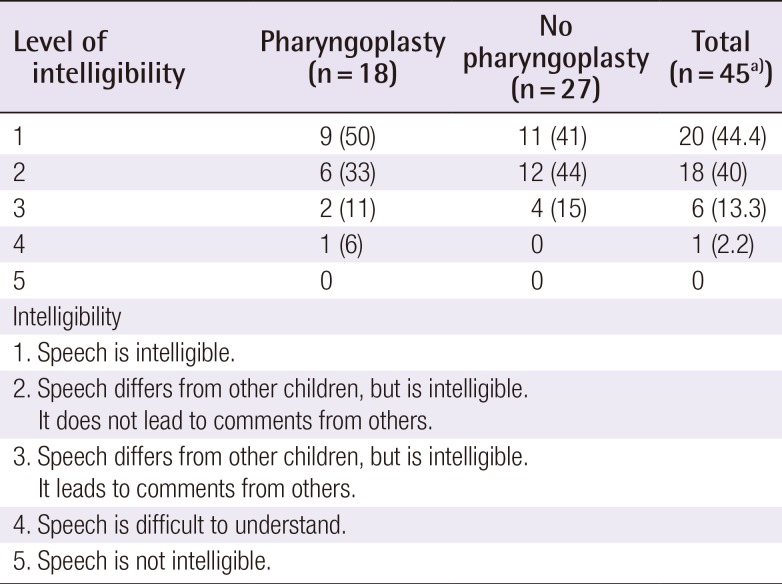
Subsequently, grimacing and intelligibility were scored during spontaneous speech (a minimum of 5 minutes). Intelligibility was scored on a 5-point scale, presented in Table 2. The intelligibility score was regarded as the main outcome parameter for the present study, as overall intelligibility is of the greatest importance in the day-to-day life of the patient.
Finally, articulation was evaluated. Patients were asked to read aloud words and sentences in which 26 target consonants or vulnerable consonant clusters were present (Supplementary Table 1). If a misarticulation occurred, the type of error was indicated on the form.
Every speech sample was digitally recorded with the Record-Pad sound recorder within the consultation room of the speech therapist (NCH Software Inc., Greenwood Village, CO, USA). After each consultation, the speech therapists re-evaluated the forms and recorded samples to produce a written report and summary of the consultation.
In order to calculate interobserver variability, speech recordings were scored twice by 2 therapists. In case of disagreement between the scores of each therapist, the score given during the live consultation was used in this study.
Statistical analysis
All data was analysed using SPSS ver. 20 (IBM Corp., Armonk, NY, USA). Mean and median values were calculated where relevant. The independent-sample t-test, chi-square test, or Mann-Whitney test was used to compare groups. The gamma correlation test was used to calculate correlations. To determine interobserver agreement, the linear weighted kappa was calculated using vassarstats.net [12]. A P-value of <0.05 was regarded as statistically significant. In order to correct for multiple comparisons and to prevent the occurrence of a type 1 error, the modified Bonferroni correction according to Holm was applied when calculating the correlations presented in Table 3. The methods were approved by the Medical Ethical Research Committee in accordance with the principles expressed in the Declaration of Helsinki.
RESULTS
Surgical outcomes
A pharyngoplasty was performed in 19 of the 48 patients (40%) (Table 1). Twelve patients (25%) had a history of clinically significant fistulas of the soft and/or hard palate. A trend for a higher fistula incidence in patients who had undergone a pharyngoplasty was observed (42% vs. 14%, P=0.027).
Speech outcomes
Intelligibility of speech
The interobserver reliability (H.W., S.H.) was κ=0.589, indicating moderate agreement. Intelligibility scores are presented in Table 2. Overall, 38 patients (84.4%, total n=45) patients scored either a 1 or 2, indicating that their speech was clear and intelligible, with minimal distortion of sounds, vowels, and consonants (Table 2). Intelligibility was not significantly different between patients who had or had not undergone a pharyngoplasty (P=0.939). Thirty-six of the 48 patients (75%) reported a history of speech therapy, of whom 28 (77.8%) received speech therapy on a frequent basis.
Resonance
Hypernasality was scored both perceptually and by nasometry. Twenty-seven patients (61.4%) had normal perceptual resonance (n=44). One patient (2.3%) had severe hypernasality, and 16 patients (36.4%) had light to moderate hypernasality.
Nasometric scores were obtained for 46 of the subjects. In an analysis of the oronasal sentences, 5 patients (10.9%) showed increased nasalance scores (>2 SD) compared to the normative values. Eight patients (17.4%) had increased nasalance scores (>2 SD) while reading out the oral sentences. The incidence of increased nasalance scores was not significantly different in patients without a history of a pharyngoplasty (P=0.089 and P=0.966, respectively).
DISCUSSION
Previously published studies have reported contradictory speech results after two-stage palate closure [571314]. In addition, only a few studies have investigated speech outcomes in adults [714]. In the present study, 48 non-syndromal UCLP patients were included in a long-term speech assessment approximately 20 years after delayed hard palate closure was performed at a median age of 33 months. Intelligibility was regarded as our main outcome measure. Forty-one patients (84.4%) had normal intelligibility, with possible minimal speech aberrations, as indicated by an intelligibility score of 1 or 2. As expected, the intelligibility scores were significantly correlated with the amount of articulation errors (P<0.001). To achieve this result, 42% of the patients needed speech-enhancing surgery.
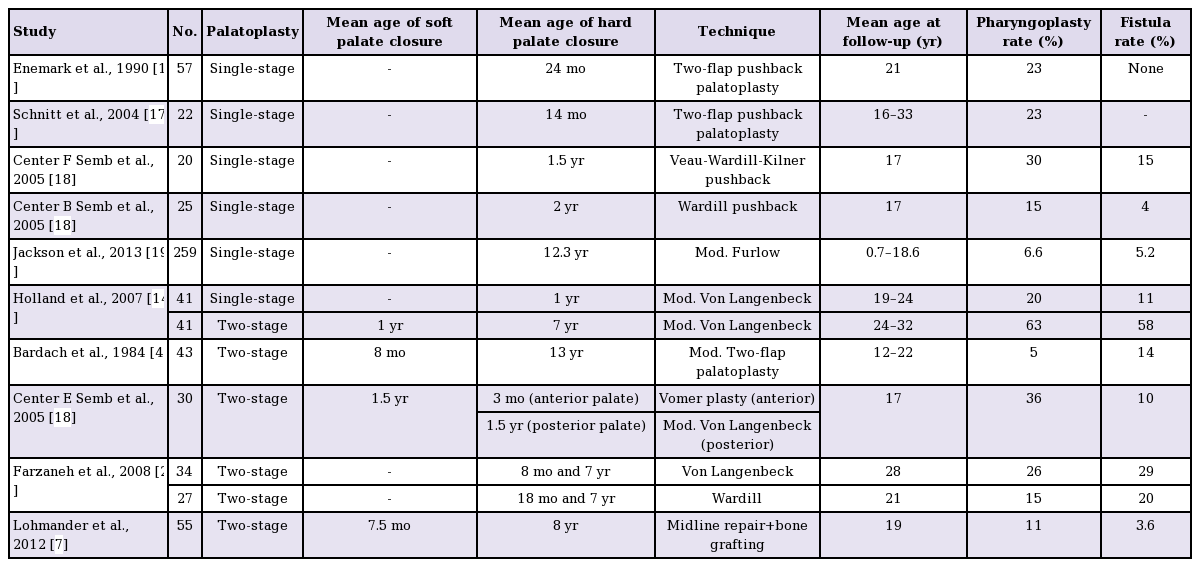
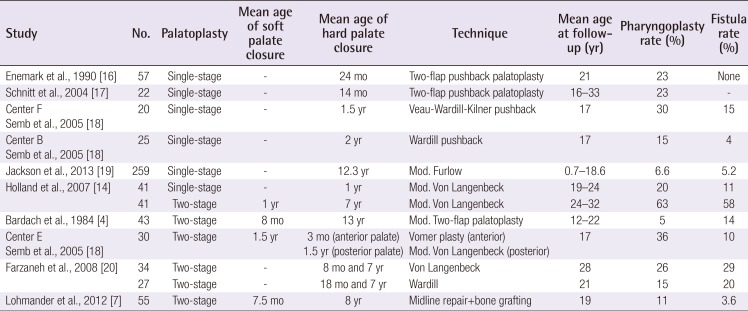
So far, few studies have reported good long-term speech results after delayed hard palate closure [37]. Lohmander et al. [7] found excellent long-term intelligibility results in UCLP subjects after delayed palate closure at the age of 8. In their cohort, 98%–100% of the patients were intelligible; no patients showed moderate or severely reduced intelligibility (3–4 on a 4-point scale). Furthermore, 94% of the UCLP patients treated according to the original Schweckendiek protocol (from the Marburg project) had ‘normal’ or ‘intelligible’ speech [3]. These results should, however, be interpreted with caution, as Bardach et al. [4] published less favourable results in adults treated by a similar protocol a few years later, showing high rates of velopharyngeal insufficiency (Table 5). Similarly, Holland et al. [14] reported more unfavourable speech results after two-stage closure than after one-stage closure. The currently available long-term studies, therefore, show contradictory outcomes regarding speech and intelligibility after delayed hard palate closure. Factors other than surgical timing are likely to influence speech outcomes and should be considered.
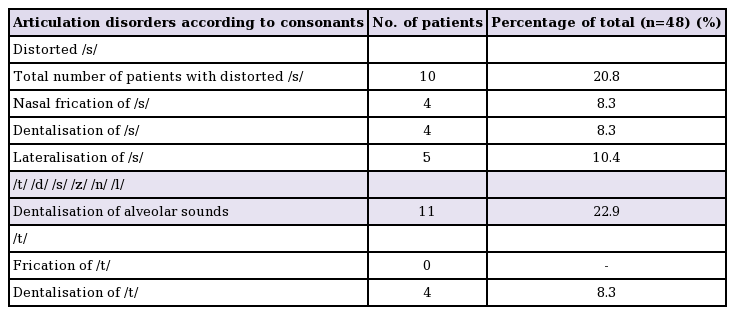
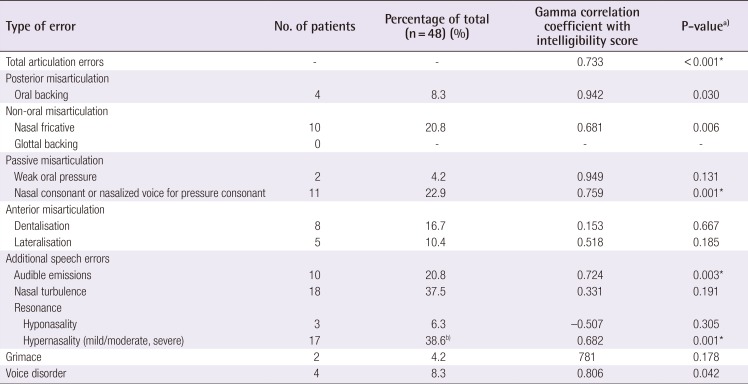
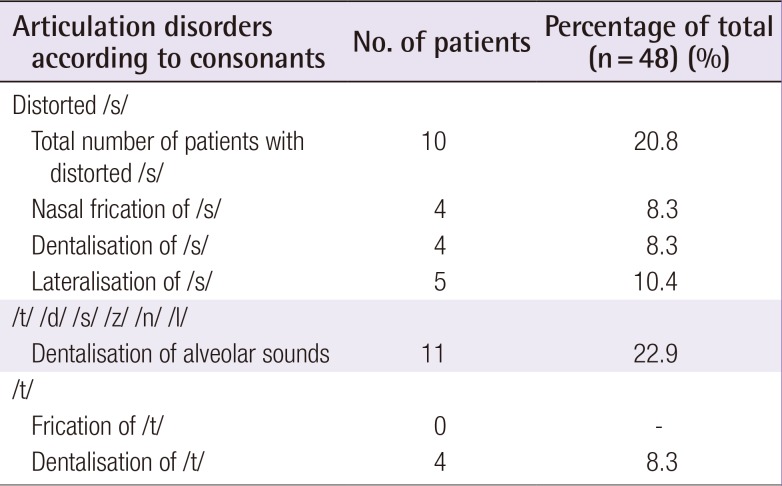
As resonance and articulation contribute to normal intelligibility, both parameters should be assessed when analysing intelligibility results [15]. We found a significant correlation between the amount of articulation errors and the level of intelligibility (P<0.001). The cohort described by Lohmander et al. [7] showed a lower incidence of articulation errors, which could be an explanation of their better outcomes. In our series, the presence of nasal fricatives, nasal emissions, and nasal consonants for pressure consonants seemed to be correlated with worse intelligibility outcomes (P=0.006, P=0.003, P=0.001, respectively). Remarkably, we also found a high incidence of dentalisation and lateralisation (27.6%) in the present series, mostly during the pronunciation of alveolar consonants. In cleft patients, the production of alveolar sounds is vulnerable due to the irregular alveolar structure and/or dental occlusion. In the present cohort, nearly 45% of patients had significant malocclusion with an initial Goslon Yardstick score of 4-5, which might therefore have negatively influenced articulation and intelligibility in our series. In addition, interdental articulation seems to be a common articulation error in the general Dutch and Flemish populations [21]. A similar phenomenon might be present for the /s/ sound in the Dutch language [21], and could explain our high incidence of /s/ distortions compared to previous reports (Table 4) [721].
The presence of nasalance and velopharyngeal insufficiency affects speech and intelligibility, in addition to articulation. We also found a correlation between the presence of nasal fricatives or nasal emissions and poorer intelligibility scores (Table 3). The incidence of perceptible nasal emissions was relatively high compared to previous long-term outcomes after early one-stage palate closure [19]. Our high incidence is in line with the hypothesis that delayed hard palate repair leads to speech difficulty at a young age, with a higher risk of subsequent speech problems [23]. In accordance, we observed a high pharyngoplasty rate (40%). High incidences of pharyngoplasty after two-staged palatoplasty have been described earlier (Table 5) [1418]. Interestingly, Lohmander et al. [7] and Holland et al. [14] both performed delayed hard palate closure around the age of 8 years, but found a great difference in the pharyngoplasty rate (11% vs. 63%). This again confirms that factors other than surgical timing are likely to have an influence on velum function, such as the degree of scarring, the skill of the individual surgeon, the technique used, and the cleft width.
One of those factors might also be the presence of fistulas needing additional surgical closure. In the present study, 25% of the patients had a history of clinically significant fistulas, which is higher than has been reported in previous studies (Table 5) [141819202122]. Similarly, Landheer et al. [23] demonstrated a 24% fistula rate after two-stage repair, compared to a 14% rate after one-stage repair. In our series, patients with a history of fistulas had a significantly higher pharyngoplasty incidence (P=0.023). The previous literature seems to confirm a positive correlation between fistulas and the need for a pharyngoplasty [4716171819202324]. This correlation might partially explain the difference in speech results and pharyngoplasty incidence (11% vs. 63%) between the results of Lohmander et al. [7] and Holland et al. [14], as fistula incidence differed greatly between the studies (3.6% vs. 58%, respectively) while the timing of palate closure was similar. Unintended fistula formation is caused by dehiscence of the surgical closure, which is inevitably followed by some healing of secondary intention, retraction, and scarring. As a result, the tissues remain under tension and the levator muscle is tethered more ventrally, even to the hard palate. Soft palate functioning is therefore negatively affected, which may in turn increase the need for speech-enhancing surgery. However, factors such as cleft width, extensive palatal dissection, and surgical technique increase both the risk of velopharyngeal insufficiency and of fistulas [142325]. Fistula formation may therefore not be a direct cause of velopharyngeal insufficiency, but in this study the incidence of both factors seemed related. It is however clear that impairment of speech and/or maxillary growth is multifactorial, and not solely determined by the timing of cleft closure. Furthermore, surgical skill is hard to measure, but no doubt has an important influence on outcomes. Future treatment protocols should therefore not be determined mainly by the timing of surgery, but should also try to minimize scar tissue formation, especially around the soft palate, when taking speech into account.
Our study has some limitations. The completeness of data for this retrospective study depended upon the detail and accuracy of past medical records. As the time range of this study includes more than 20 years, some data could not be retrieved, resulting in missing values for some of the parameters. In addition, patients were invited for long-term follow-up and therefore participated voluntarily. It is possible that patients with a more prolonged treatment or a less favourable outcome be might more inclined to accept an invitation for the long-term evaluation of their treatment. This may lead to selection bias and, possibly, an underestimation of the speech outcomes. Nevertheless, we found no significant differences in the treatment history of the patients that presented for follow-up and those who did not (Table 1).
In conclusion, this study describes long-term speech outcomes after two-stage palatoplasty, in which hard palate closure was performed at a mean age of approximately 3 years old. Intelligibility scores were moderate within this adult group. We observed a relatively high incidence of articulation errors and mild hypernasality within our population. In addition, 42% of the subjects needed speech-improving surgery and 25% had a history of clinically significant fistulas. Factors other than the timing of hard palate closure itself are likely to influence speech development. The high incidence of secondary surgical procedures, including fistula closures and surgery to address poor dental occlusion (as assessed by Goslon scores), might have contributed to the presently observed average speech outcomes.
Notes
The work was supported by the Department of Plastic Surgery at University Medical Centre Utrecht.
This study was presented at the 72nd Annual meeting of the American Cleft Palate-Craniofacial Association, held on April 24, 2015, Palm Springs, USA, and at the 10th European Craniofacial Congress, June 25, 2015, Gothenburg, Sweden.
This article contains Supplementary Table 1.
No potential conflict of interest relevant to this article was reported.
References
SUPPLEMENTARY MATERIAL
Supplemental data can be found at: http://e-aps.org/src/sm/aps-44-202-s001.pdf.
Supplementary Table 1
Test form for the evaluation of speech in patients with an orofacial cleft according to the Dutch national protocol (translated into English)