Usurpation of the role of the plastic surgeon as a public health problem in Mexico: Reflections on a case
Article information
Introduction
Unlike other professions in Mexico, the training of professionals in health is supervised by the Interinstitutional Commission for the Training of Human Resources in Health (CIFRHS), which is jointly administered by the Secretary of Public Education, the Ministry of Health, and the various universities that endorse the curricula. The fundamentals of medical residency are established in the official Mexican standard 001-SSA3-2012. In Mexico, plastic and reconstructive surgery is a surgical subspecialty. Despite having a regulatory system, in recent years, some institutions have offered postgraduate courses in health sciences (master’s degree, diplomas, or training) without complying with the stipulations of the CIFRHS, as exemplified by graduates of masters or cosmetic surgery programs.
These courses have an average duration of 2 years and comply neither with any regulations nor with any university curricula. When the program ends, they grant a master’s degree in aesthetic surgery that makes students believe that they are fully prepared to perform aesthetic or reconstructive surgical procedures, without actually being plastic surgeons [1].
In 2011, a ranking of the countries with the most plastic surgical procedures was released. Among the 20 countries listed in the ranking, Mexico was the sixth in terms of the most plastic surgical procedures performed. According to the ranking, the most common procedure was abdominoplasty [2]. In expert hands, the complication rate is less than 1% [3]. Since the number of non-certified plastic surgeons has increased, the complication rate has also increased considerably.
Necrosis of the skin flaps accounts for between 2% to 3% cases and is caused by incorrect surgical technique or tobacco consumption. This complication is an aesthetic catastrophe that produces a deformity, prolongs the patient’s hospital stay, increases costs, and predisposes the patient to a higher rate of systemic complications [4].
Clinical case
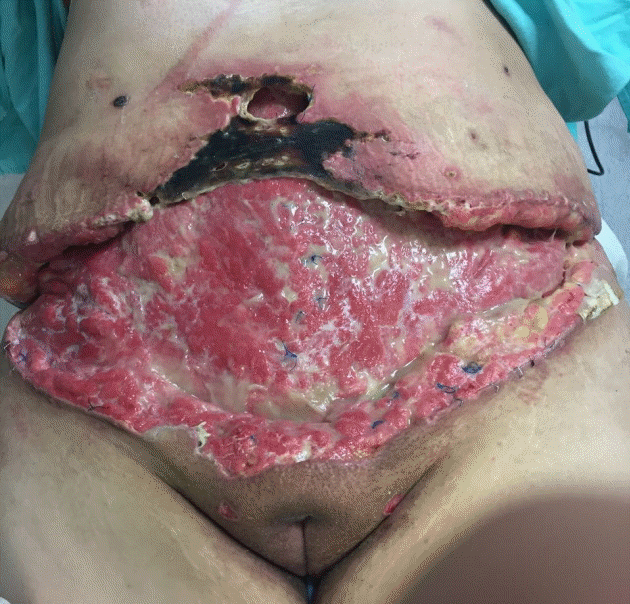
A 27-year-old woman had the following important antecedents: rheumatoid arthritis with unspecified treatment, a 10-year history of smoking with a smoking index of 13, obesity grade II (body mass index [BMI], 37 kg/m2), minor depression without treatment, and bichectomy and liposuction of the jowls 3 months previously. She was referred to our unit because 2 weeks before admission to the hospital, she underwent an abdominoplasty performed by a doctor who was not an expert in plastic surgery (the doctor in question had a master’s degree in cosmetic surgery). She was discharged the day after surgery. Three days after the surgical intervention, the patient presented with hyperemia, hyperthermia, leakage of purulent material, and pain on the surgical margins. Two days later she presented with necrosis of the surgical margins, increased output of purulent material, fever, and poor general condition. Once necrosis was found to be present along the surgical edges and cutaneous flaps, with signs of sepsis, she was referred to our hospital. In our evaluation, necrosis of the pubic flaps was found at the bilateral costal margin, with a cutaneous defect measuring 40 cm×20 cm, with purulent material output (Fig. 1). The purulent secretion was cultured, and Escherichia coli and Candida albicans were found, for which broad-spectrum antibiotic management was initiated. Surgical washing and debridement was performed on two occasions, and a vacuum-assisted closure system was placed in the last procedure, followed by the harvesting and application of a partial-thickness skin graft covering a bloody area measuring approximately 15 cm in diameter.
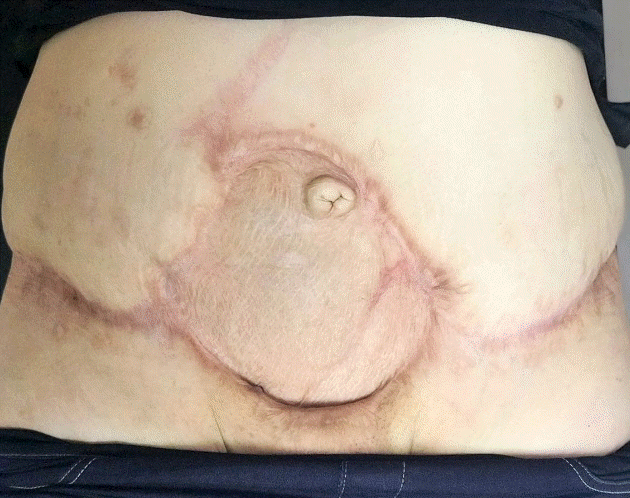
At a check-up after 6 months, proper integration of the cutaneous grafts was observed (Fig. 2) and a left breast nodule was detected. The patient reported that the same non-specialist doctor had injected a substance into both breasts. The nodule was classified as Breast Imaging Reporting and Data System IV; however, the patient did not attend subsequent appointments.
Discussion
The legal gaps that exist in the secretariats of public education of the states of Mexico have allowed the issuance of professional certificates as masters in aesthetic surgery, which allow the bearer of such a certificate to perform aesthetic surgery without possessing the necessary knowledge and skills. These practitioners abuse the psychological pain caused by the patient's bodily discomfort, offering surgery at very low costs and performed in unhygienic places [5]. However, above all, these doctors do not have professionalism, integrity, or honesty. They do not hesitate to place their patients at imminent risk [6,7]. In this case, the patient had a medical history (obesity, smoking, and rheumatic disease with treatment) that contraindicated this procedure. Tobacco has been associated with damage to the microcirculation that favors the appearance of cutaneous necrosis [8]; however, presumably due to a lack of knowledge, the doctor who carried out this procedure omitted the requirement for this patient to follow a supervised diet, to inform her that she should give up smoking, and to thoroughly investigate the drugs she used to control her rheumatoid arthritis, as such drugs alter the healing process. Moreover, the patient stated that she had not reached her desired parity. Currently, contraindications for abdominoplasty include scars in the right, left, or bilateral upper quadrants (relative); severe comorbid conditions (heart disease, diabetes, or smoking); future plans for pregnancy (relative); a history of thromboembolic disease (relative); morbid obesity (BMI >40 kg/m2); and unrealistic expectations on the part of the patient [9,10]. Although these guidelines have been clearly stated in the literature, the programs in aesthetic surgery do not provide the necessary training to practice plastic surgery. In this case, the patient experienced poor aesthetic outcomes and her health was put at risk.
Conclusion
The lack of regulation has allowed untrained practitioners to perform aesthetic procedures, putting the health of patients at risk, increasing the costs of hospital care, exacerbating morbidity and mortality, and worsening aesthetic outcomes. Therefore, strict regulation of the practice of plastic surgery is required to prevent this from becoming a further risk to public health.
Notes
No potential conflict of interest relevant to this article was reported.
Ethical approval
The study was approved by the Institutional Review Board is the Departament of Teaching and Research (IRB No. HRAEO-CIC-CEI007-17) and performed in accordance with the principles of the Declaration of Helsinki. The informed consent was waived.
Patient consent
The patient provided written informed consent for the publication and the use of her images.