INTRODUCTION
Breast reconstruction with flap surgery has fewer complications compared with breast reconstruction with artificial implants, such as implant displacement, infection, and capsular contracture [
1]. This procedure results in a more natural breast than does breast reconstruction with artificial implants [
2]. However, changes in breast volume occur over time following breast reconstruction with flap surgery [
3]. Quantitative measurements of breast volume in follow-up periods after breast reconstruction using a flap have not yet been reported.
Therefore, in the current study, postoperative breast volume changes were measured after breast reconstruction using transverse rectus abdominis myocutaneous (TRAM) flap. The results of these measurements should be helpful for deciding the flap size based on the defect after mastectomy and more objectively evaluating the postoperative results.
METHODS
Subjects
A total of 27 patients underwent immediate breast reconstructions using TRAM flaps after mastectomy from September 2007 to July 2010. The patients that were examined using positron emission tomography/computed tomography (PET/CT) or magnetic resonance imaging (MRI) were excluded, and the patients followed up using CT were included in the study. The patients who had received radiation therapy after mastectomy were also excluded.
CT scans were routinely performed for surveillance in the general surgery department to detect metastasis and recurrence of cancer. Therefore, CT scans did not need to be performed for our breast measurement study.
The method of breast volume measurement
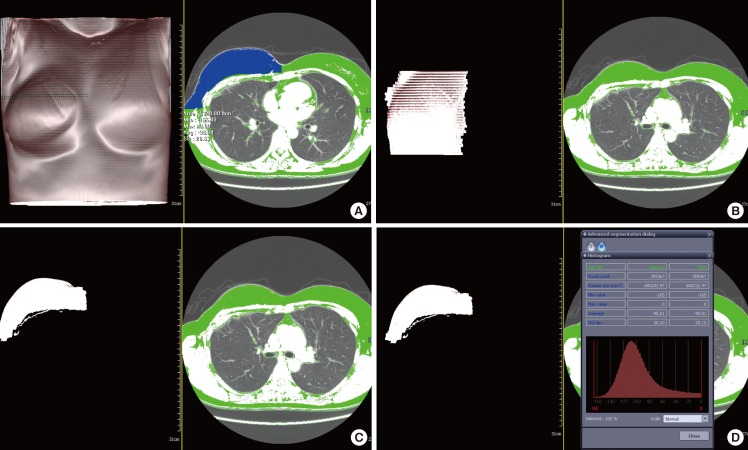
Consecutive CT scans were performed at 1 mm intervals, 1 mm thickness at 120 kV, and 170 mAs with a v64 channel multidetector computed tomography (MDCT) device (LightSpeed, GE Healthcare, Milwaukee, WI, USA) while the patients were lying supine, holding their breaths, and raising both hands over their heads. The breast volumes were examined using the Infinitt program (Infinitt Health Care, Seoul, Korea). We checked each section of the breast such as the section visible in a CT axial view, and changed each section into a three-dimensional image and measured the volume. The same surgeon checked the volume 3 times for each patient, and the median value was set as the breast volume.
When we measured the breast volume, we set the range of the breast from the posterior margin, anterior of the pectoralis major to the anterior margin, skin, and nipple-areola complex. On the axial view, we set the range of the breast from the starting part of the breast crest to the ending part of the breast crest. The medial side of the breast was the lateral border of the sternum, and the lateral side of the breast was the mid-axillary line (
Fig. 1).
The method of evaluation
We compared the changes in breast volume over time. In all 10 patients, the first CT scan was performed at about 9 months after breast reconstruction (average, 9.2 months), and the interval period between CT scans was about 1 year (average, 11.7 months).
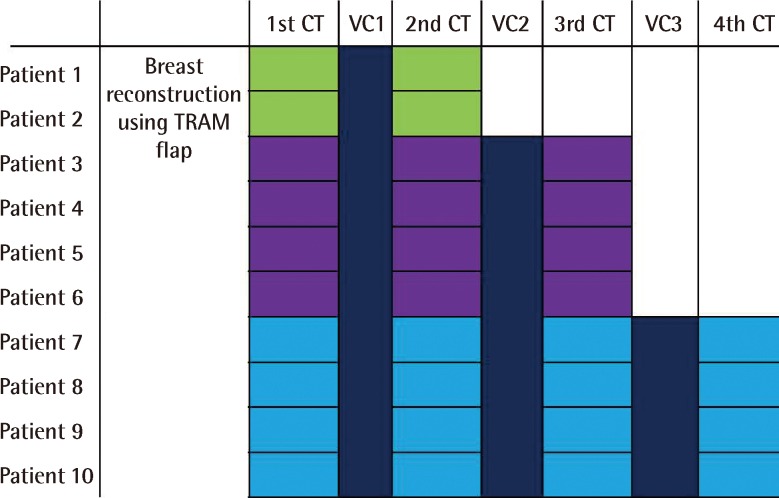
We evaluated the breast volume change between each CT scan. We defined the interval volume change (VC) between the first CT and second CT scan as "VC1" (n=10), the volume change between the second CT and third CT as "VC2" (n=7), and the volume change between third CT and fourth CT as "VC3" (n=4) (
Fig. 2).
We evaluated the mean change of VC and VC in proportion to the breast volume in the earlier CT. We used the Wilcoxon signed-rank test for statistical verification.
RESULTS
All 10 patients underwent modified radical mastectomy in the general surgery department of our hospital. All of the patients underwent pedicled TRAM flap using the contralateral superior epigastric artery. All 10 patients were diagnosed with invasive ductal carcinoma. The patients were categorized according to stage as follows: stage I, 2 patients; stage IIa, 7 patients; and stage IIIa, 1 patient. All 10 patients were treated with the same regimen of chemotherapy and hormone therapy (
Table 1). The mean age of the patients was 44.3 years, and the mean follow-up period was 3.8 years.
Volume changes of breasts with lesions treated with TRAM flap
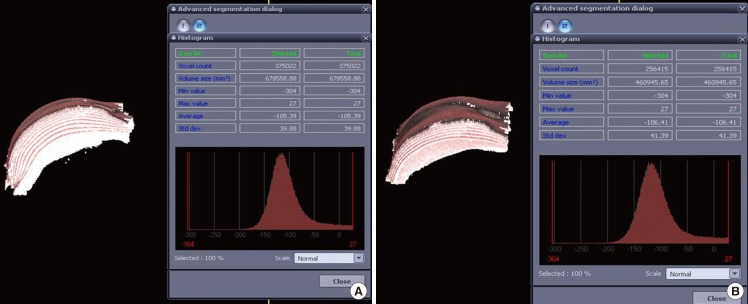
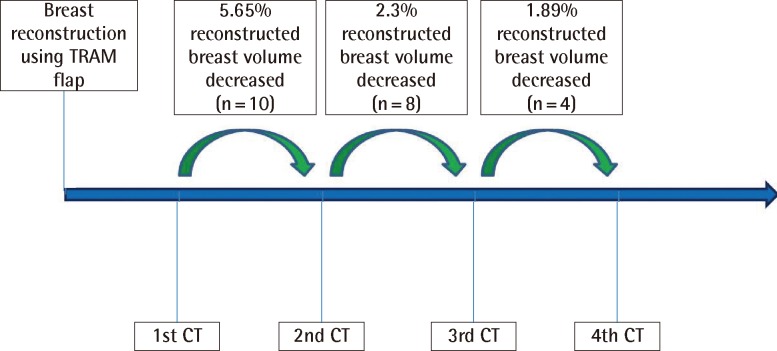
Of the 10 patients, the volume of the breast that had the lesion decreased on average over time (
Table 2): VC1 was 5.65%, VC2 was 2.3%, and VC3 was 1.89%, decreased in proportion to the earlier CT. The differences in VC1 (P-value, 0.005) and VC2 (P-value, 0.018) were statistically significant. However, the difference in VC3 was not statistically significant (P-value, 0.068) (
Figs. 3,
4)
DISCUSSION
The goal of breast reconstruction is for the breast that had the lesion to resemble the preoperative breast. For this, symmetry of both breasts needs to be satisfied. During the postoperative follow-up period, the evaluation criteria of the changes in the breast and symmetry of both breasts depends almost entirely on the surgeon's subjective criteria.
The measurement of breast volume is clearly necessary when performing breast reconstruction and mammoplasty. Using this measurement, we determined the size of the breast implant and the increase of the patient's postoperative satisfaction. Many methods are available to measure breast volume, but no standard method has yet been established; therefore, at our hospital, we depend on the surgeon's subjective decision when making preoperative plans or postoperative predictions.
In a prior study, Tegrmeier [
4] measured breast volume using overflowing water when the breast was dipped in a bowl filled with water. Grossman and Roudner [
5] measured the breast volume using a self-constructed device. Edsander-Nord et al. [
6] measured the volume using a thermoplastic casting. Methods that measure breast volume changes using three-dimensional body surface images from devices such as laser scanners [
7] and stereo photographs [
8] have also been introduced. Recently, with the development of radiologic technology, indirect breast volume measurements using MRI and its usefulness have been reported [
9,
10].
The method for measuring breast volume with an imaging device involves less discomfort for patients, and we can ignore the changes caused by the patient's position. CT is less expensive and more cost-effective than MRI. CT has been long used for follow-up evaluations on the recurrence of breast cancer after breast resection and metastasis of localized lymph node.
The measurement of volume using a CT scan was introduced previously in the diagnosis of a blow-out fracture. Lee et al. [
11] argued that the exact diagnosis and prediction of volume change in an injured orbit over time could be obtained through a CT scan. The prediction of orbital volume change through the follow-up period is important for determining whether surgery should be performed or not. Similarly, in this study, objective and quantitative data could be obtained through CT scans, and the exact preoperative plan and postoperative change of the breast were predicted.
To satisfy the symmetry of both breasts following breast reconstruction, Stevenson and Goldstein [
12] increased patient satisfaction by performing mastopexy and breast reduction on the contralateral breast, but this was performed on a Western women who had large breasts and on other patients who had ptosis of the breast. Thus, applying this to East Asian women who tend to have small to medium-sized breasts is not appropriate. Therefore, an accurate size of the flap inserted into the breast with the lesion has to be considered for breast reconstruction.
Amir et al. [
13] reported that proper flap size was obtained by measuring the resected breast tissue and the flap volume using Archimedes' rule for breast reconstruction with a free TRAM flap. Lazarus and Hudson [
14] also reported that the proper flap size was obtained by measuring the resected breast tissue and flaps using scales. However, after breast reconstruction, the volume of the breast that has been operated on began to change. Amir et al. [
13] determined the proper volume of the flap, which was calculated from the actual volume of the flap, plus an additional 10% of its volume. However, no reports have mentioned volume changes that occur over time. Therefore, this study aimed to determine the VC of flaps over time by measuring the VC in the operated breast using CT scanning. We found that after more than 3 years of follow-up, the change in breast volume could be ignored. Therefore, we should closely observe the breast volume for 2 years.
Based on these results, surgeons and patients were more satisfied with the results obtained by applying an over-correction of the flap size when the design of the flap was made.
In this study, inter-observer bias was minimized because only one examiner measured all of the breast volumes. Intra-observer bias was also minimized by using a mean value of three separate measurements.
Measuring breast volume using CT scans also depends on the examiner's subjective judgment, and the inaccuracy of measurements can cause apparent differences between breast volumes. This method considered only the volume of breasts in evaluating symmetry and did not consider the shapes of the breasts.
This study has some limitations. Because only a few cases were examined, the results cannot be broadly generalized. Moreover, the follow-up periods were short and the radiation effect on the flap was ignored; there was also the risk of unnecessary radiation exposure. Therefore, this study's findings are limited to generalization to the following types of patients: patients who want immediate breast reconstruction after mastectomy, patients who have a high risk potential for local or distant metastasis, which should be observed using CT scanning during the follow-up period, and patients who do not need adjuvant radiation therapy after breast reconstruction.
However, measuring the volume of the breast using a CT scan is cost-effective and does not cause patient discomfort. Therefore, this method is an objective and effective method for measuring breast volume and can be very helpful in designing the size of TRAM flaps on the defect after mastectomy.
It is well known that breast reconstruction after breast cancer extirpation plays an important role in offering benefits to restore symmetry, correct body image, and improve psychosocial wellbeing. Patients' desire for the restoration of body image after breast cancer extirpation is increasing markedly. There are a variety of reconstructive options available to patients. There has been a great deal of debate over the advantages of reconstructive surgical methods of the breast, but almost all plastic surgeons agree that breast reconstruction with autologous tissue is the most suitable surgical option for breast cancer patients. However, as the author observed, change in breast volume occurs over time, following breast reconstruction with autologous tissue.
Amir et al. [
1] determined the volume needed for an inserted flap, figured from the actual volume of the removed flap plus an additional 10 percent of its volume, given a predictable volume decrease. However, while this quantitative calculation of additional volume needed for an inserted flap is useful for flap shaping and volume measurement, it is not adequate for measurement of the reconstructed breast volume during follow-up.
Let it first be said that I agree with the author's decision to measure the postoperative breast volume change using computed tomography (CT) after breast reconstruction with the transverse abdominal myocutaneous island flap. It is a novel method for measurement of breast volume change over time during follow-up.
However, there are some limitations to this study. First, for the consecutive CT scanning, the patient was laid in the supine position while holding postoperative tissue edema, the position of the inserted flap, the status of the breast skin envelopes, and the ratio of the volume of the inserted flap versus the original breast skin her breath and raising both hands over her head. Normal breasts of women sag laterally in this position, but a reconstructed breast of a patient does not initially sag because of envelope. All of these factors could have introduced a measurement bias by repetition of CT scanning through uncorrectable flap motion although the author set the fixed bony point at the medial and lateral border. After the author checked each section of the axial CT scan, the sections were transformed into three-dimensional (3D) images. The process of this transformation would also introduce a bias in each axial scanBreast volume measurement using a 3D laser surface image change rather than in a CT scan is more accurate. Furthermore, a 3D surface image obtained using non-invasive recording in the standing position provides the ability to quantitatively evaluate symmetry, volume, shape, contour, and surface, and also measure distance [
2]. Second, this study included a very small number of patients. The author classified the patients into 4 groups, and each group was composed of 2 or 3 patients. This means that the volume change in one patient from the same group differs as much as the mean value of the group. To reduce statistical bias, each group should have had more than 7 patients. Finally, there were cost-benefit effects. The author affirmed that measuring the volume of the breast using a CT scan is cost-effective and does not cause discomfort to the patient. I disagree with the author's point of view on that matter. A 1-mm-thick slice in a follow-up CT scan for breast volume measurement is a much thinner section than routine breast CT scan, which is 5 mm in thickness in each section. This follow-up CT scan is not covered by insurance in Korea, and it is an additional economic burden to patients.
In conclusion, this article was the first trial for measurement of volume changes in breast reconstruction patients using CT scans. It would have been better if the volume measurement using a CT scan could represent the appearance and symmetry of the breast.