The management of nasal defects following surgery is influenced by several factors, including histology, location, staging, and previous treatment regimens employed [
2-
5]. These characteristics define the degree of tumor control and therefore the reconstruction [
4]. The size and location of the defect as well as the availability of adjacent skin are further factors to be considered. The patients' age, co-morbidities, and aesthetic goals must also be included in the decision making process [
8,
9]. The ideal reconstruction closes the defect following tumor resection with a good tissue match and no stenosis or distortion. Immediate closure decreases morbidity, prevents hemorrhage and minimizes wound infection [
10]. The forehead represents a maximum tissue reservoir for reconstructing large, full-thickness defects of the nose. The forehead flap is the method of choice for closure of nasal defects that are not amenable to more simple reconstructive options [
11,
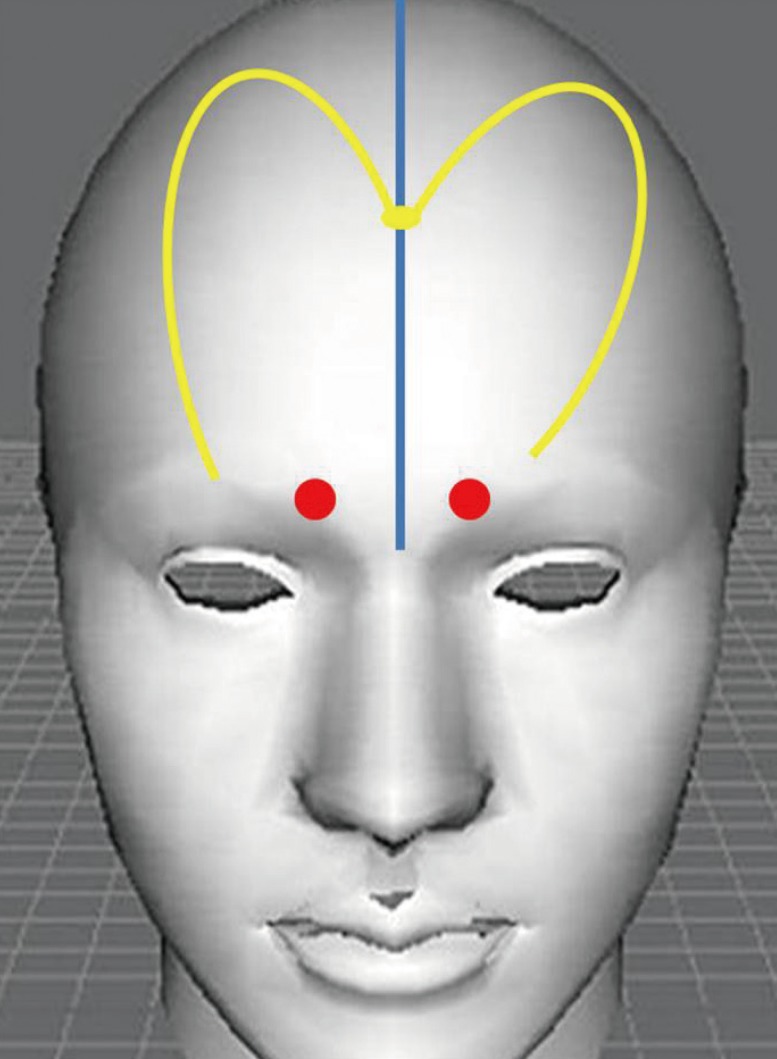
12]. This flap is based upon the supratrochlear artery, which crosses the supero-medial orbit approximately 1.7 to 2.2 cm lateral to the midline, and courses vertically in a paramedian position approximately 2 cm lateral to the midline [
3-
9]. The Doppler location of the supratrochlear artery localizing its exact position allows flap harvesting with a relatively narrow pedicle of less than 1.5 cm. This facilitates pivot rotation providing a more effective flap length and preventing donor site deformity in the glabellar region [
5]. Vascular delay is performed at three weeks with appropriate debulking and contouring at the recipient site [
3]. If the lining is missing, its replacement should be the first consideration. Various alternatives can be considered to replace the internal nasal lining, including skin grafting, folding the distal aspect of the cutaneous flap on itself, intranasal pedicled mucosal flaps or epithelial turn-in flaps from around the defect. Skin grafts may contract and do not allow major cartilage replacement at the first stage. Small intranasal pedicled mucosal flaps (including septal and bipedicled septal/vestibular flaps) may be harvested ensuring an excellent blood supply. Nonetheless, a composite septal flap may not reach down to the nostril without compromising midline support and significant secondary donor site morbidity may lead to septal perforation formation [
5-
8]. On this basis, the revisited bilobed flap has an axial vascular pattern, which represents a valid alternative to reconstructing both the nasal lining and skin simultaneously with reduced complications. In particular, it is a double transposition flap, and its geometry enables a better distribution of the tensile forces along its rotation axis, avoiding the distortions and redundancy generated by other flaps. Our bi-pedicled flap has two main differences, as described in the plastic surgery literature. First, the traditional bilobed flap is a double transposition flap with a single pedicle in which the first flap is transposed into the defect and the second smaller flap is transposed to repair the secondary defect resulting from the larger flap transposition. Our flap differs from the classical description since it is equipped with two distinct vascular axes and two transposition flaps of equal dimensions fitting the receiving site (
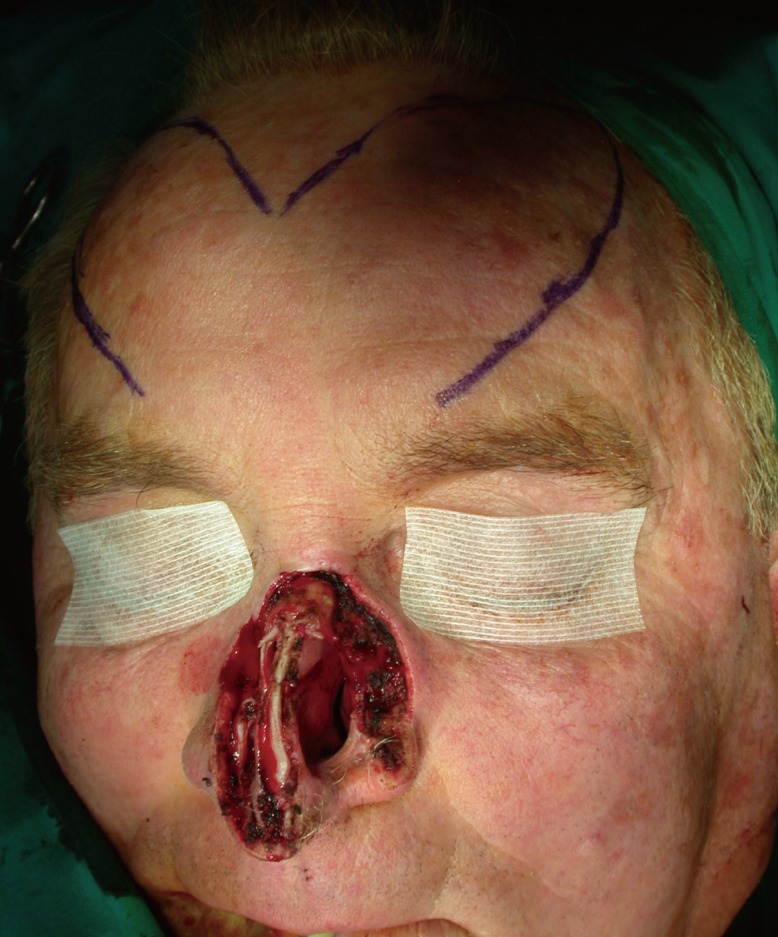
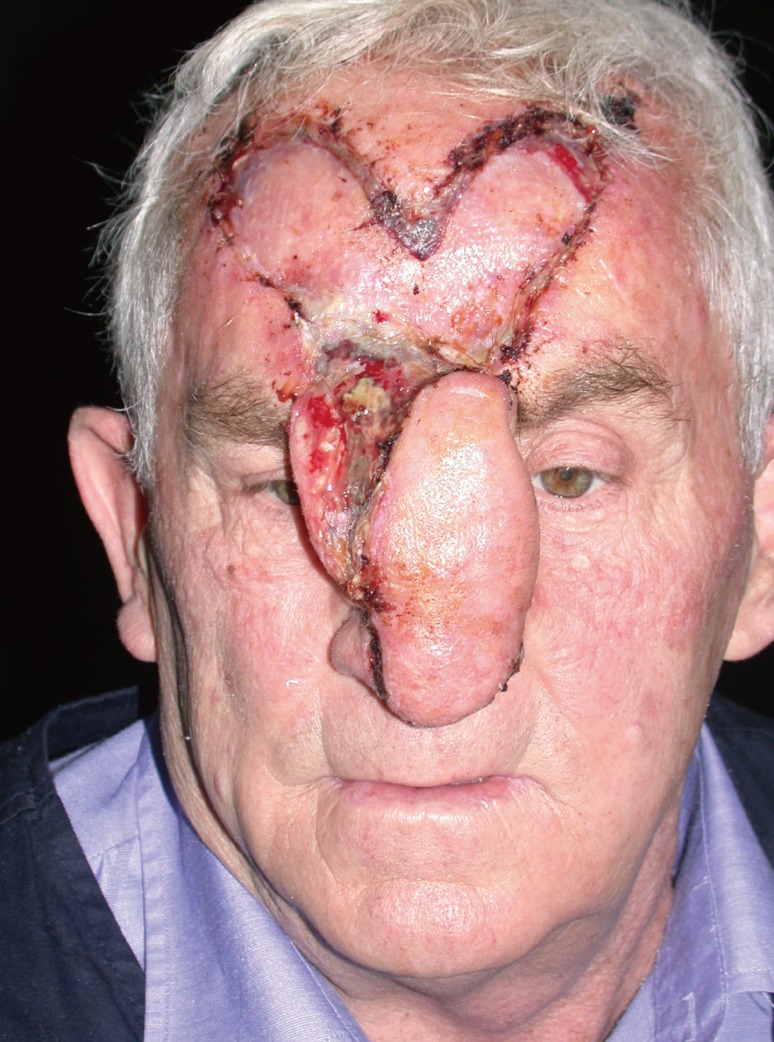
Fig. 3). Second, a bilobed forehead flap was described more than 30 years ago by McGregor for restoring a large nasal skin defect without lining involvement resulting from tumor excision [
12]. Our bi-pedicled forehead flap is used to reconstruct full-thickness defects by restoring the nasal lining with a transposition flap and the nasal skin by a contralateral specular flap. Consequently, this reconstructive technique is feasible for reconstructing full-thickness nasal defects of varying sizes of the whole nasal framework.
The bi-pedicled forehead flap is not suggested for the restoration of superficial defects but for total or subtotal nasal reconstruction [
1]. Indeed, the folded flap requires the use of bone or cartilage supports and includes simultaneous restoration of the nasal lining and skin. The forehead is usually well repaired following delay, with some exceptions, notably the superolateral areas, which remain covered by skin grafts. Nonetheless, the cosmetic outcome of the donor site is acceptable and well-tolerated [
8-
10,
13]. The forehead is not interrupted with a vertical scar commonly associated with the traditional forehead flap but instead exhibits gentle and curvilinear incisions, except laterally. Further refinements can be performed postoperatively. Limitations include discomfort due to the vascular delay (3 weeks) and a possible revision to thin the folded flap. Additionally, even if a simultaneous reconstruction of the nasal lining and facial skin can be achieved with a median or paramedian forehead flap grafted on the deeper layer, the flap often lacks bulk in many cases and grafting of cartilaginous or osseous support almost always proves problematic [
11,
13]. Furthermore, free tissue transfer significantly increases the difficulty, operating time, cost, and bulk of the tissue transferred [
11]. The bi-pedicled forehead flap, equipped with two thick and hairless lobes, can be considered a valuable resource and a valid alternative even for other complex facial defects in the orbital (exenteratio orbitae), zygomatic, and cheek regions.