Type, distribution, and location
The type, distribution, and location of the lesions were evaluated through physical examination and imaging tests in patients in whom a VM was suspected. With the exclusion of the eight patients who underwent only D-USG, the multifocal type was found in five patients (6.8%) and the unifocal type in 69 patients (93.2%) on MRI or CT scans. The lesion size was less than 5 cm in 45 patients (60.8%) and more than 5 cm in 29 patients (39.2%). The margin was well-defined in 41 patients (55.4%) and ill-defined in 33 patients (44.6%).
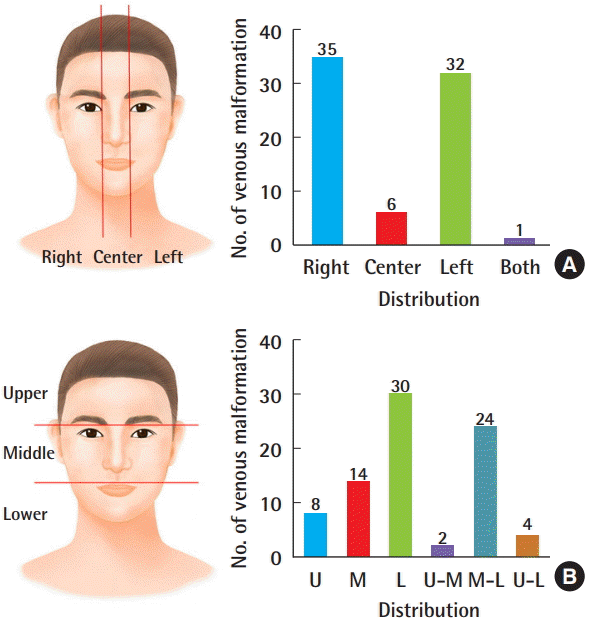
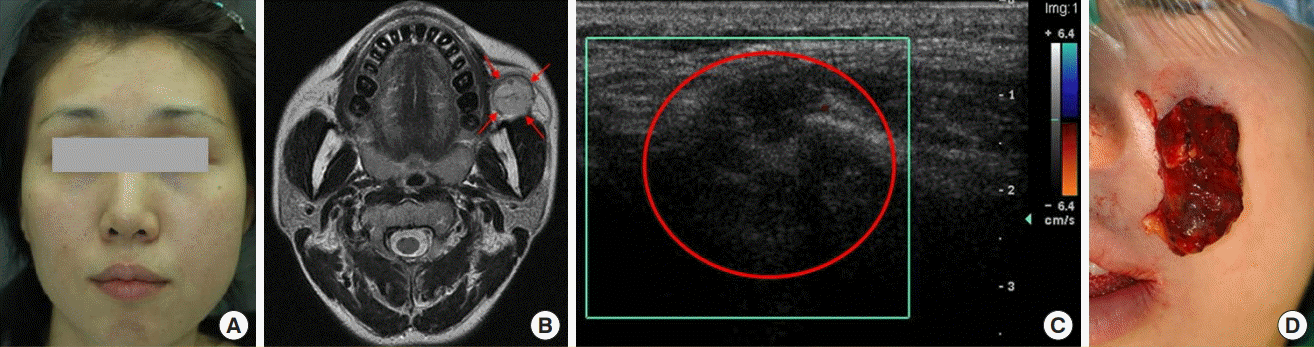
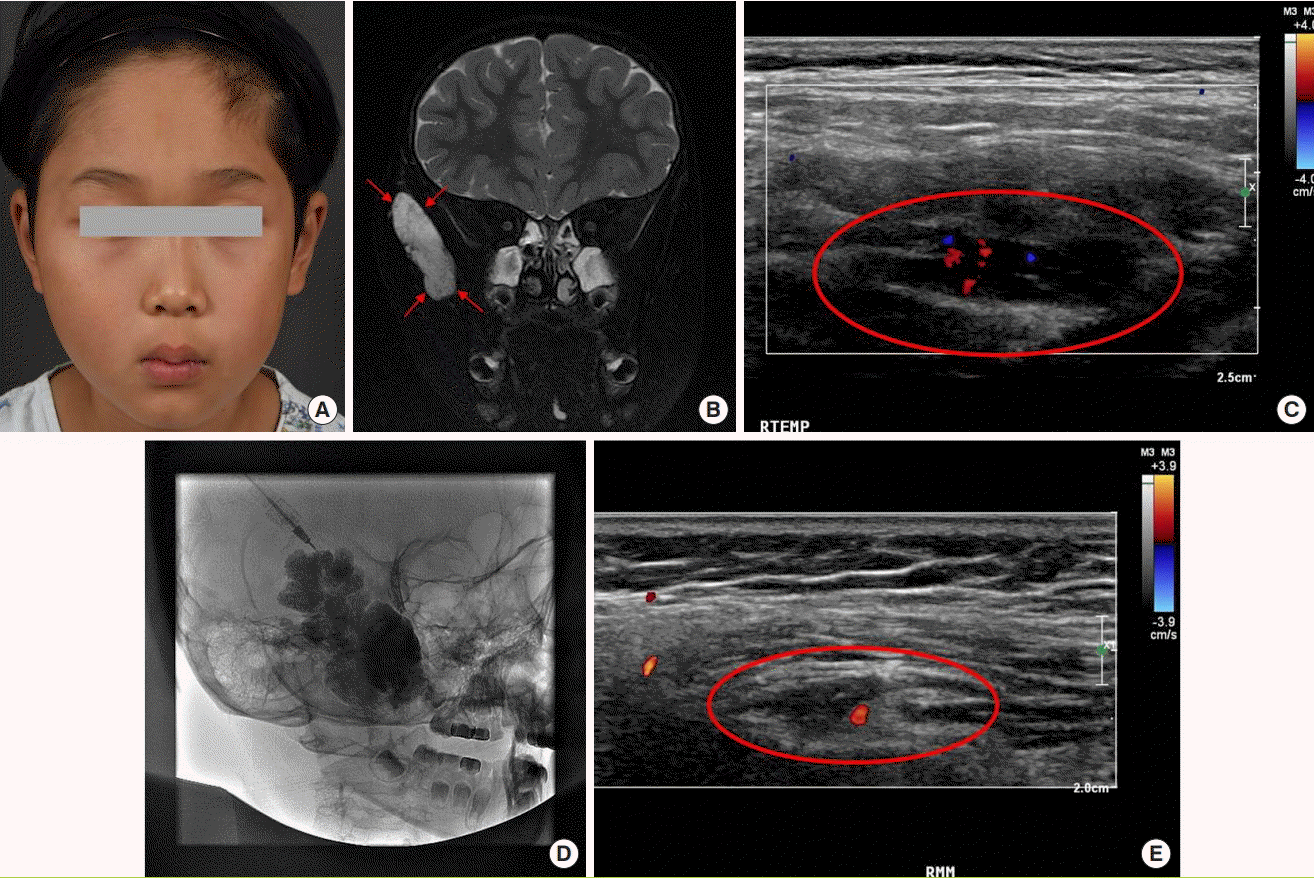
Among the 74 patients with information from MRI or CT scans, VMs occurred more often on the right side (35 patients, 47.3%) than on the left side (32 patients, 43.2%), and were most common in the lower region (30 patients, 36.6%), followed by the middle-lower region (24 patients, 29.3%), and the middle region (14 patients, 17.1%). Altogether, the right lower region was the most common incidence region (
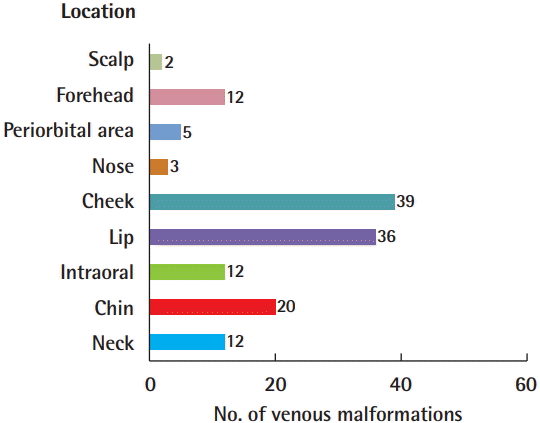
Fig. 1). When the location of the head and neck VMs was divided into nine regions, the most common region was the cheeks (39 patients), followed by the lips (36 patients) and the chin (20 patients), and 38 patients had two or more affected regions (
Fig. 2).
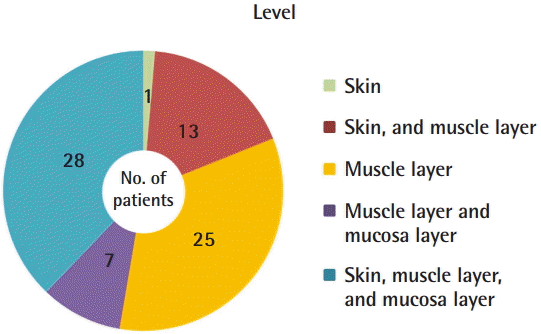
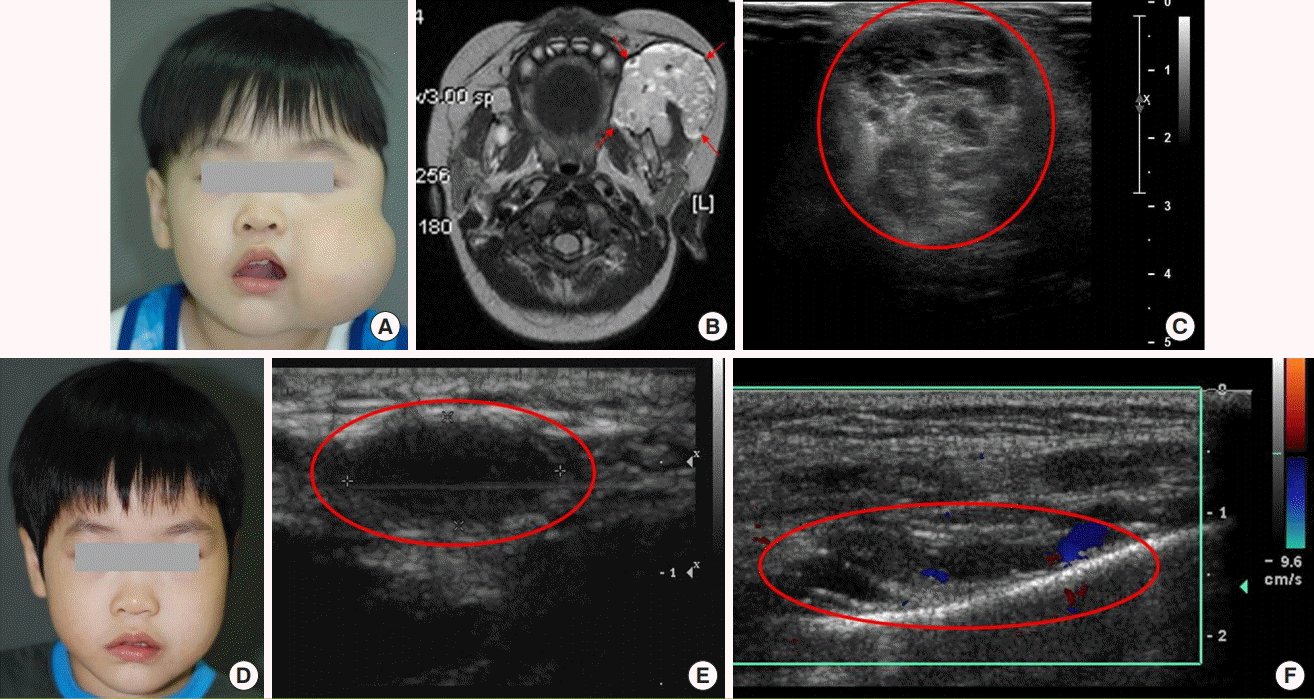
With the exclusion of the eight patients in whom this information could not be identified, the VMs in the 74 remaining patients were classified based on the depth and level of invasion, as follows: the skin (including subcutaneous tissue), the muscle layer, and the mucosa layer. The muscle layer was invaded in 98.7% of patients, but in one patient (1.3%), the VM was confined to the skin, including the subcutaneous tissue. The most common region of invasion was the skin (including subcutaneous tissue) along with the muscle and mucosa in 28 patients (37.8%), followed by the muscle layer only in 25 patients (33.8%), the skin (including subcutaneous tissue) and the muscle layer in 13 patients (17.6%), and the muscle and mucosa layers only in seven patients (9.5%) (
Fig. 3).
Diagnosis
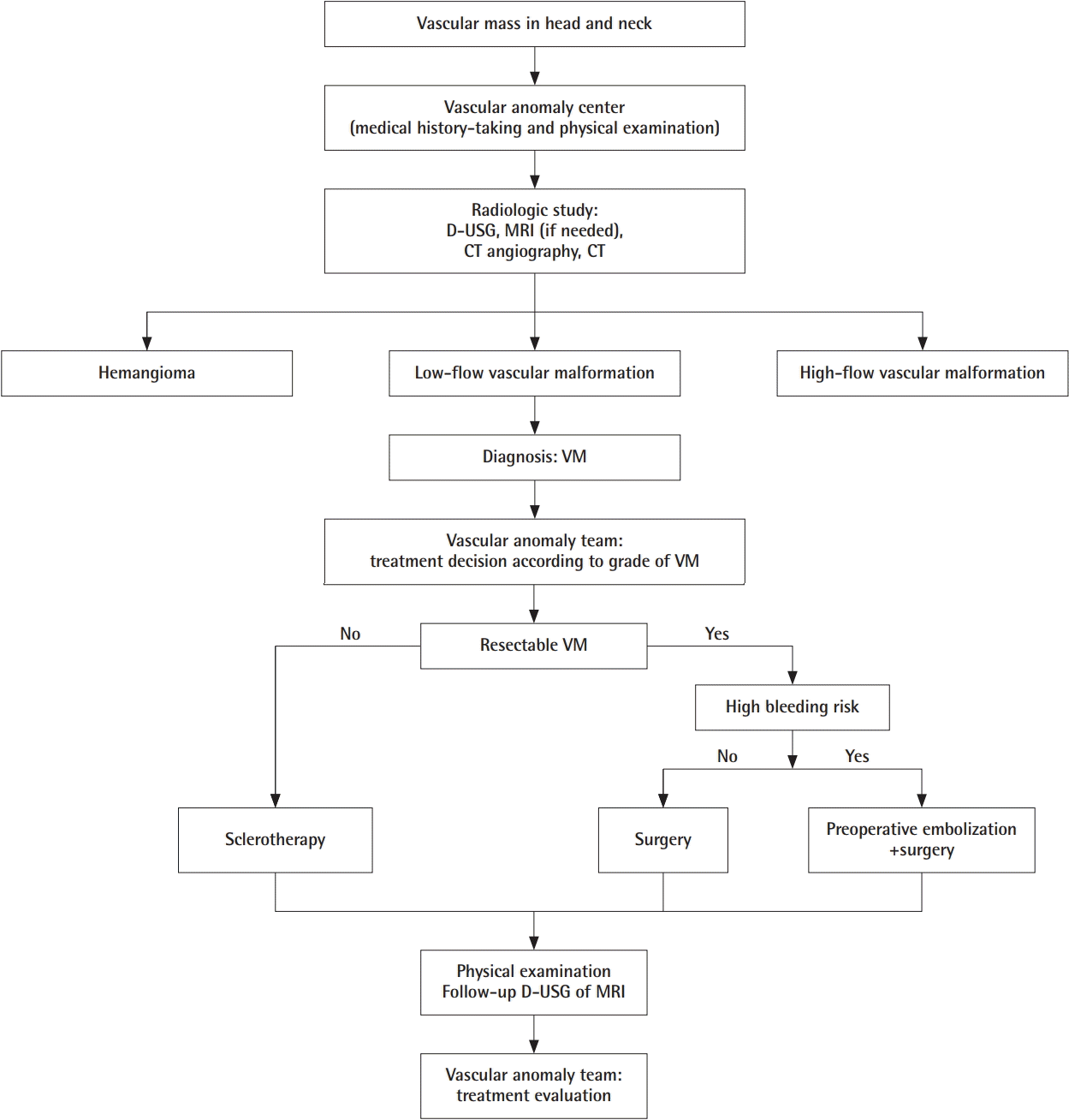
Fig. 4 shows the algorithm used for the diagnosis and treatment of patients suspected to have a vascular mass in the head and neck. Each patient’s diagnosis was finalized in collaboration with the various departments within the VAC and was confirmed through imaging tests or biopsy, mostly after a physical examination and history-taking in patients suspected to have a vascular malformation.
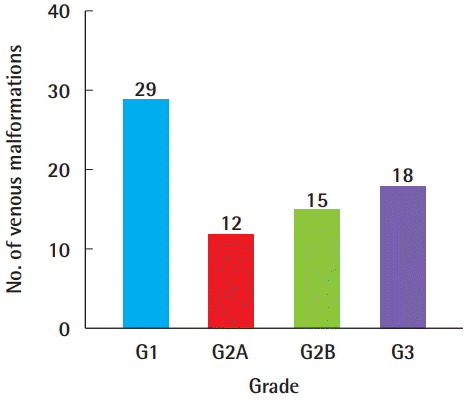
Imaging tests were performed with CT, MRI, and D-USG. Of the 82 subjects, 68 (82.9%), 12 (16.2%), and 60 (81.1%) underwent MRI, CT, and D-USG examinations, respectively; two patients (2.7%) underwent imaging after a punch biopsy at another local medical center, while two patients (2.7%) underwent surgical resection without imaging for simultaneous diagnosis and treatment. In 58 patients (78.4%), two or more tests were performed, including an imaging test and biopsy, 14 patients (18.9%) were treated after a single test, and seven patients each underwent MRI and D-USG. In the first diagnostic workup, D-USG was performed in 36 patients (48.6%) and MRI in 34 patients (45.9%), and both MRI and D-USG were performed in 31 patients (41.9%) around the same time within a week. Due to the burden of radiation, CT was performed only when the size of the lesion and its relationships with adjacent structures needed to be clarified. When dividing the grade by the size and margin after an MRI or CT scan, a grade 1 VM was found in 29 patients (39.2%), a grade 2A VM in 12 patients (16.2%), a grade 2B VM in 15 patients (20.3%), and a grade 3 VM in 18 patients (24.3%) (
Fig. 5).
Treatment
Sclerotherapy was performed 2.54 times on average as the main treatment method, and it was the only treatment in 40 of the 82 patients (48.8%), except for two patients under observation. With the inclusion of patients who also underwent surgery during the treatment period, sclerotherapy was performed in a total of 66 patients (78.6%). Sclerotherapy was performed prior to debulking surgery for totally unresectable lesions, and was also performed in cases of significant functional impairment or cosmetically severe deformities, or for uncontrolled symptoms such as severe pain or swelling and bleeding. Sclerotherapy was also performed when there was concern about massive intraoperative bleeding, or when VMs involved major organs, with a risk of impaired vision, hearing, or eating.
For sclerotherapy, the VM was directly punctured under fluoroscopy, and contrast was used to identify the VM territory before injection; depending on the sclerosant, a maximum of 0.15 mL/kg of alcohol (range, 0.5–7.5 mL), from 0.5 mL of 0.5% sodium tetradecyl sulfate (STS) foam to 6.0 mL of 3.0% STS foam (range, 0.5%–3.0%; 0.5–6.0 mL), or 0.1–2.3 U/kg of bleomycin foam (1 mg/1 mL=1 U; range, 1–35 U) was used. Considering age, sex, body weight, the lesion’s location, the depth of invasion, and complications, STS, bleomycin, and alcohol were selected or used in parallel.
Surgery alone was performed in 14 patients (17.1%), while in 26 patients (31.7%), a combination of surgery and sclerotherapy was performed. Surgery was either complete resection or debulking. Complete resection was performed for small to moderate-sized well-defined VMs that did not invade vital structures. Debulking surgery was performed for unresectable lesions, to provide symptom relief before sclerotherapy, or when bulkiness remained after sclerotherapy. Surgery was performed with due consideration of postoperative complications such as scarring.
Prior to the surgical resection of large VMs, a decision was made whether to prevent intravascular coagulopathy by using low-molecular-weight heparin. Laser therapy was performed in 11 patients after sclerotherapy or surgery.
The treatment outcomes showed improvement in 27 of the 40 patients (67.5%) treated with sclerotherapy alone and in 16 of the 26 patients (61.5%) who underwent sclerotherapy with surgery. Of the total of 66 patients who underwent sclerotherapy with or without surgery, 43 (65.2%) showed improvement, whereas nine (64.3%) of the 14 patients who had surgery only showed improvement (
Table 1).
In terms of management by the grade of the VM, sclerotherapy alone was the most frequent treatment in grade 1, grade 2A, and grade 3 VMs, whereas in grade 2B VMs, sclerotherapy along with surgery was the most common. Grade 1 VMs were most frequently treated with sclerotherapy (15 patients, 50.0%), followed by surgery with sclerotherapy (9 patients, 30.0%). Grade 2A VMs were most frequently treated with sclerotherapy (6 patients, 54.5%), followed by surgery (3 patients, 27.3%). Grade 2B VMs were most frequently treated by surgery with sclerotherapy (6 patients, 40.0%), followed by sclerotherapy (4 patients, 26.7%) and surgery (4 patients, 26.7%). In grade 3 VMs, sclerotherapy was the most common treatment (9 patients, 50.0%), followed by surgery with sclerotherapy (7 patients, 38.9%).
Good results were observed most often in all grades (grade 1, 36.7%; grade 2A, 54.5%; grade 2B, 40.0%; grade 3, 50.0%). In grade 1 VMs, the next most common results were excellent in nine patients (30.0%) and poor in five patients (16.7%). In grade 2A VMs, excellent results were obtained in three patients (27.3%) and a poor result in one patient (9.1%), and in grade 2B VMs (15 patients), excellent results occurred in three patients (20.0%) and a poor result in one patient (6.7%). In grade 3 VMs (18 patients), the results were poor in seven patients (38.9%) and excellent in two patients (11.1%) (
Table 2).
Post-treatment complications occurred in three of the 82 patients (3.7%), and two discontinued treatment due to delirium or skin blanching during sclerotherapy. The other patient developed skin necrosis after sclerotherapy. All three patients with complications improved with conservative management.