In the past decade, snakebites have been verified as a common occupational hazard for farmers and field workers and have been officially recognized by the WHO as a neglected tropical disease [
3,
4]. In addition to being an occupational hazard for workers in developing countries, snakebites are becoming more common in developed countries with improvements in quality of life, as spending more leisure time in outdoor activity equates to an increased chance of snake encounters and, in turn, snakebites. Worldwide, the estimate of snakebite victims is 421,000 persons per year, of whom 20,000 people die as a complication of the envenomation event [
5]. In South Korea, the annual incidence of snakebites ranges from 192 to 621 cases, with an average of five deaths per year. There are four species of venomous snakes that reside in Korea:
Gloydius blomhoffii, Gloydius saxatilis, Gloydius ussuriensis, and
Rhabdophis tigrinus [
6]. The venom from these snakes is usually not toxic, and systemic derangement from the response to the injected toxin is rare. Only a few clinical cases of mortality have been documented on the Korean peninsula. Consistent with other reports, our study found the same epidemiologic patterns, in which most bites happened in the afternoon and evening and the peak incidence of bites occurred in the rainy season [
7,
8]. In contrast to reports from Southeast Asian countries, where 70% of injuries are to the lower extremity, the percentage of upper extremity injuries is 69.6% in Korea. Although systemic complications, such as rhabdomyolysis, acute renal failure, coagulopathy, and hemolytic anemia were observed, they did not lead to mortality [
9]. In most cases, the symptoms as well as the lab processes were improved by the use of antivenom and conservative treatment. However, in addition to systemic complications, local complications, such as soft tissue necrosis and compartment syndrome, remain problematic. Hematotoxic/cytotoxic venom can initiate a significant amount of inflammation and edema in the injected tissue. If this process occurs deep within a compartment surrounded by non-compliant tissue (i.e., bone, ligament, and intermuscular fascia), the increasing edema leads to rising compartmental pressure and the potential for obstruction of distal perfusion, as well as local tissue ischemia. Although compartment syndrome has the same underlying physiologic basis regardless of the initial cause, the clinical presentation and diagnosis differ significantly between cases of snake envenomation and high-energy injury. In high-energy trauma (i.e., crush injuries), the clinical presentation alone is often sufficient to distinguish the physiologic changes from the injury itself from these of compartment syndrome (e.g., pulselessness and pain out of proportion to the injury). However, these distinguishing features of compartment syndrome are not reliable indicators in cases of snakebite because snake venom itself can cause hemodynamic instability (pulselessness) and significant pain that is out of proportion to two mere fang marks. The potential for the missed diagnosis of compartment syndrome in cases of snakebite was initially responsible for liberal use of fasciotomy in the 1960s for the management of snakebites, when a low threshold was set for snakebite-related compartment syndrome. The ischemic signs of compartment syndrome, excluding severe pain, are late signs and should not be relied on for the early diagnosis of compartment syndrome [
10]. For the past decades, the clinical consensus has been that such a low threshold was a cause of unnecessary surgical interventions, and various authors have advocated the use of antivenom in snakebite injuries, with fasciotomy performed under strict, absolute indications [
11]. Currently, the established guidelines suggest that fasciotomy is indicated in snake-bitten limbs that meet the following criteria [
1,
12,
13]: (1) hemostatic abnormalities have been corrected (antivenom with or without clotting factors); (2) clinical evidence of intracompartmental syndrome; or (3) intracompartmental pressure >40 mmHg (in adults).
The incorporation of intracompartmental pressure measurements as a diagnostic criteria for snakebite-related compartment syndrome is relatively new. So far, the authors are not aware of any other study on the use of objective pressure data to evaluate the need for fasciotomy in the context of snakebites. Between 2010 and 2013, fasciotomies were performed in just two cases at our institution, consistent with other studies reporting single cases of fasciotomy among hundreds of snakebite patients [
14-
16]. In 2014, intracompartmental pressure measurements were adopted as an official policy at our institution for patients suspected of having compartment syndrome from snakebites (n=59). This change led to pressure readings in 33 patients, of whom 17 ultimately required fasciotomy (17/158, 10.8%) for persistently elevated pressure readings despite antivenom administration. In comparison to the reported rates, the frequency of fasciotomy at our institution appears to be extremely high. One explanation for this may be the mean time interval of 9.8 hours (range, 1–28 hours) between snakebite and antivenom administration, which is significantly longer than the recommended 3-hour window. Another potential reason for the high rate of fasciotomy at our institution may be related to the higher rate of upper extremity involvement. In other reports, the lower extremity was more frequently involved than upper extremity (i.e., the hands). This can be a significant distinction, as the foot is usually protected by footwear, and snake fangs are generally not long enough to deliver the venom directly into the deeper compartments of the lower leg. Unless venom is injected deeper, directly into the muscular compartment, most swelling therefore occurs outside of the compartment and rarely impairs intracompartmental perfusion pressure. In the hand and forearm, compartment syndrome is more likely because snakebites can often lead to venom delivery into deep compartments [
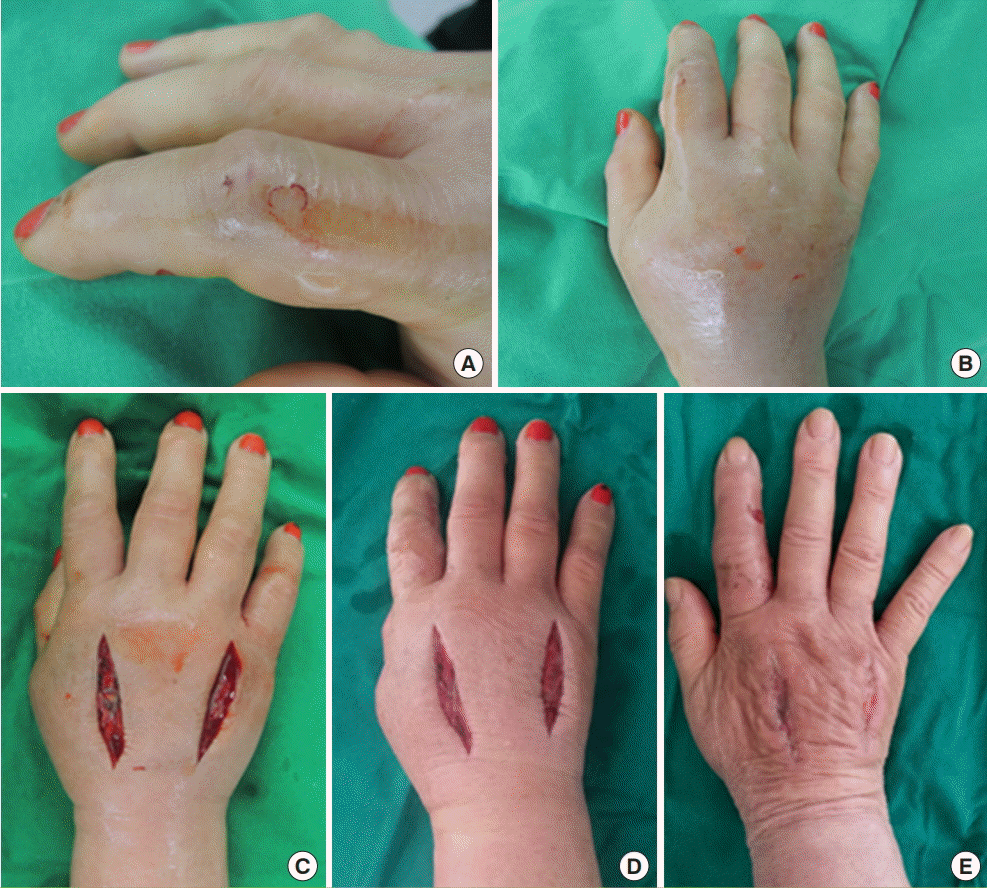
17]. In our study, 12 out of 17 fasciotomies were performed for snakebites on the hand, which suggests the anatomic site may be an important factor contributing to the development of compartment syndrome in snakebite (
Fig. 2). An alternative interpretation of our study is that, prior to 2013, we may have been too conservative in the management of potential compartment syndrome in snakebite wounds. Because both compartment syndrome and hematotoxic envenomation cause tissue necrosis, we may have missed the opportunity to perform fasciotomy in patients with actual compartment syndrome. In these patients, the tissue necrosis from increased tissue pressure and ischemia could easily have been considered as the consequence of hematotoxic venom.