INTRODUCTION
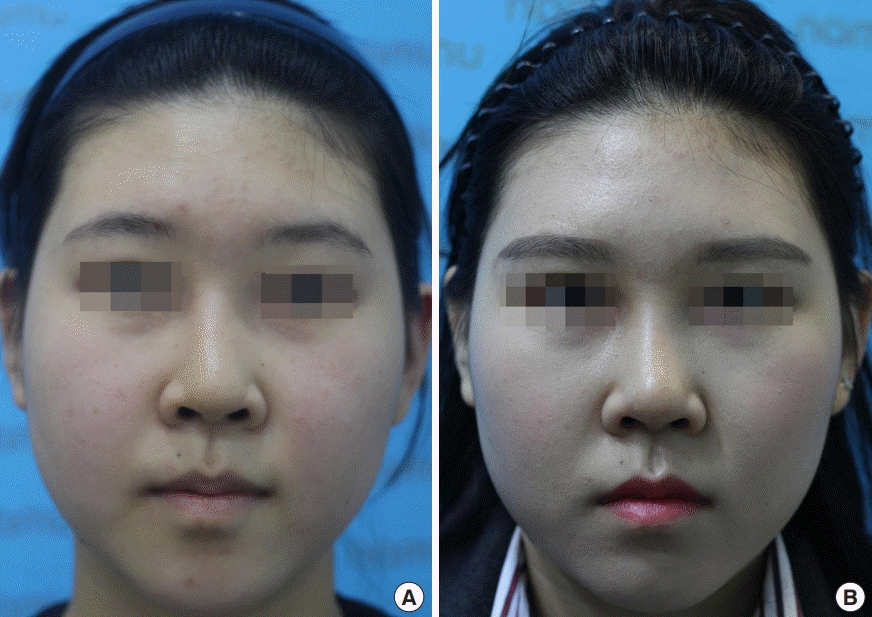
In Asians, the skin and soft tissue envelope of the nose are strong and tight, but the cartilage is scant and weak. Therefore, a bulbous tip, small nose, and short nose are frequently seen, requiring framework support [
1,
2]. Autologous, homologous, and synthetic materials are used for framework support. Among these materials, autologous tissue is preferred, but its harvest faces limitations, such as the amount and quality of cartilage, as well as structural faults at the donor site. Synthetic materials have therefore been used to overcome these limitations.
Adjuvant materials recently used in rhinoplasty include porous high-density polyethylene sheets (Medpor), polycaprolactone (PCL), polylactic-co-glycolic acid (PLGA), poly-L-lactic acid (PLLA), and polydioxanone (PDS) plates. In this study, a PDS plate was used as an adjuvant material for the cartilage framework during rhinoplasty. The PDS plate was made of the same material as PDS threads and was approved by regulatory authorities in Europe in 2009, the United States in 2010, and Korea in 2016 [
3,
4].
A PDS plate remains structurally intact until 10 weeks after implantation and serves as a temporary scaffold. After 25 weeks, the plate is completely degraded without significant effects on the surrounding structures [
5,
6]. A PDS plate also guides cartilage regeneration, so that new chondrocytes are arranged regularly at the defect area, which prevents cartilage deviation [
4]. Using a PDS plate together with cartilage results in increased strength of the cartilage and PDS plate complex. For example, using a 0.15-mm PDS plate with cartilage was found to yield a 3- to 4-fold increase in strength compared to the cartilage alone [
3,
7].
DISCUSSION
Because of the tight skin and weak cartilage structure of Asians, framework changes and support are important components of most rhinoplasty procedures in Asian patients. Various materials can be used for correction, of which autologous tissues are preferred in rhinoplasty because they are highly biocompatible and have a low risk of infection or extrusion compared to homologous or alloplastic materials [
8].
The most common material used to support the framework is the nasal septum. The nasal septum is composed of hyaline cartilage with similar properties to the native cartilaginous framework of the nose itself [
8]. Because the nasal septum is located in the same operative field, an additional incision is unnecessary, which reduces the operating time. In addition, the nasal septum is straight and strong, so it can endure the tensile force of the skin and soft tissue envelope. However, if the septum is small and thin, the harvesting procedure itself is difficult and the amount harvested might be insufficient. This might lead to subsequent collapse or weakening of the L-strut. For the same reason, harvesting is not possible if the nasal septum has already been harvested in a previous operation. Another autologous material used for framework support is the ear cartilage. The ear cartilage is an elastic cartilage that is used mainly as an onlay graft, rather than as framework support, due to its innate curved shape. Nevertheless, an incision is required on the auricle because the donor site is not in the same operative field. This could cause hypertrophic scarring or a deformity at the donor site. Rib cartilage can provide both a sufficient amount of cartilage and strong support [
9,
10]. However, harvesting rib cartilage leaves a scar on the chest wall and extends the operating time. In addition, the pleura could be perforated during harvest.
Various synthetic materials have been developed and used to overcome the limitations of autologous tissues. The ideal synthetic materials should be non-inflammatory, non-carcinogenic, non-allergenic, resistant to mechanical strain, able to be integrated into the host tissue, readily available, easy to shape, and fully sterilizable. No synthetic material satisfies all of these properties. Representative examples of synthetic materials include Medpor, PCL, PLGA, PLLA, and PDS plates. Medpor has many advantages, such as being thin, strong and easy to manipulate [
11]. However, it might damage and adhere to the surrounding tissues; thus, it is difficult to remove during a subsequent operation. Medpor is also non-absorbable [
12]. Polymers, such as PCL, PLGA, and PLLA, are biodegradable, but the absorption period can be as long as 1 to 2 years. Resected cartilage appears to regenerate after 10 weeks. Implants are necessary only as long as the supporting tissue heals; afterward, they need to be removed to avoid long-term complications. In addition, they are thicker than Medpor, potentially damaging the surrounding tissues or causing inflammation during the long absorption period [
4,
6,
7].
PDS is a colorless, crystalline, and biodegradable polymer that is used mainly as a suture material and can be made in the form of a sheet [
13]. PDS plates are available in three types defined in terms of thickness and perforation: 0.15 mm (perforated), 0.25 mm (perforated), and 0.5 mm (unperforated). These plates remain structurally intact for up to 10 weeks after implantation and serve as a scaffold. After 25 weeks, they are degraded completely by hydrolysis and metabolized with no damage to the surrounding tissues. Moreover, they do not cause any inflammatory or foreign body reactions [
4,
5]. Another important feature of PDS plates is their ability to guide cartilage regeneration [
7]. This plate is flexible and light, and has the mechanical properties of retaining memory and stiffness when an external force is applied. Therefore, it has been used to stabilize the nasal cartilage framework structures [
3,
5,
14].
A 0.15-mm perforated PDS plate was applied as an adjunct to reinforce the columellar struts or L-struts and alar cartilage push-down grafts, as well as for septal extension graft fixation and alar contour correction. The 0.15-mm perforated PDS plate retains its stiffness for 10 weeks after implantation, which is a sufficient interval for the grafted cartilage to be remodeled and enveloped by connective tissue [
3,
4]. In addition, blood and nutrients can be supplied to the cartilage through the perforations, providing a favorable environment for the survival of the grafted cartilage [
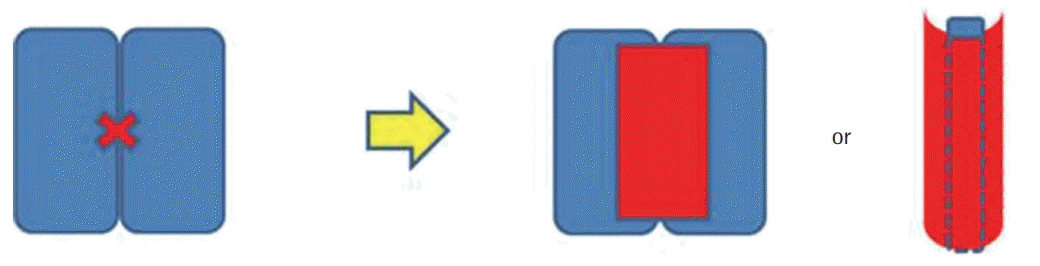
15]. If a columellar strut made of ear cartilage or the nasal septum is weak or bent, a PDS plate can be wrapped around the strut in the form of a U-shape. Definite improvements in strength and shape could be confirmed under direct vision and palpation (
Fig. 7).
The septal cartilage of the nose is the most common material used in dorsal lengthening procedures to correct a short nose. However, the cartilaginous framework of Asians is often weak and thin; thus, the amount of harvestable septum is insufficient in most patients with a short nose. Therefore, excessive harvesting can occasionally induce a saddle nose. In addition, although the L-strut is sufficient, correction should be performed using a scoring procedure when deviation occurs. For these reasons, the stability of an L-strut cannot be guaranteed. To prevent L-strut weakness, the PDS plate is attached to the remaining L-strut to enhance the strength of the remnant L-strut and to reduce the possibility of collapse. Moreover, the corrected nasal septum can be maintained in a straight form after reduction because the PDS plate acts as a splint (
Fig. 8).
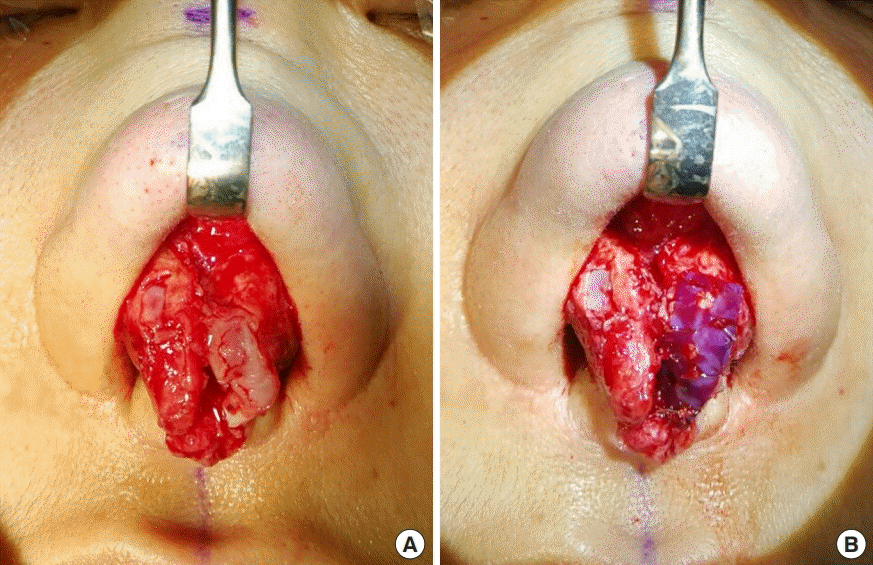
A tip extension suture is another useful tool for Asian patients [
16]. When a PDS plate is used in tip correction, the contact area is the surface, so that the retention force is superior to the suturing method alone. In addition, the PDS plate can act as a scaffold or splint for weak or deformed alar cartilage, enabling it to maintain a favorable shape and strength (
Fig. 9).
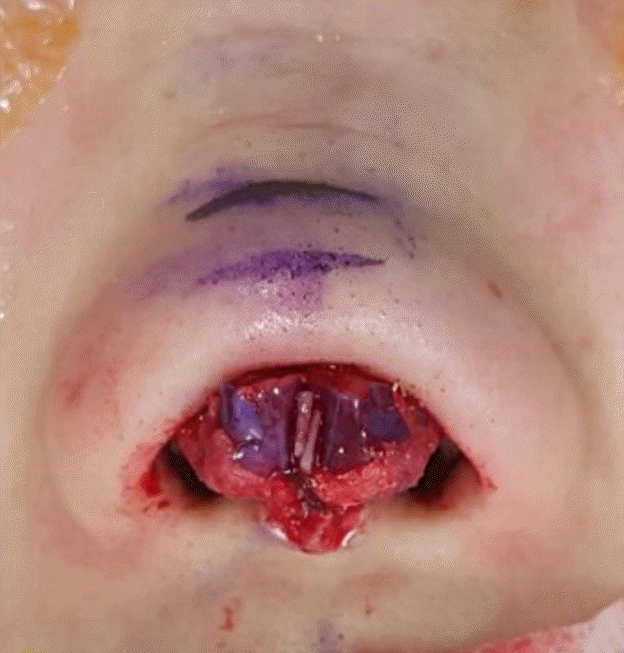
The septal extension graft can be fixed as a spreader or batten type. In this manner, a PDS plate is placed over the graft to facilitate fixation and to increase the strength of the graft. The PDS plate also allows end-to-end placement of a septal extension graft, which reduces the extent of septal bulging of a bilateral spreader or batten graft. The PDS plate retains similar memory and stiffness to the ear cartilage, so it can be used to correct the alar contour. In addition, it can be used for deformities of the upper lateral cartilage, such as inner valve collapse.
Compared to the line or point force exerted by a suture, the membrane-type PDS plate is advantageous because it has a larger contact surface (
Fig. 10).
As a recommendation based on our experiences, the PDS plate should be have a rounded-off edge to prevent palpation and exposure, particularly at the nasal tip and anterior columella, because the plate can be palpable or exposed if its cutting edge is sharp. Additionally, the authors recommend that an objective evaluation should be conducted over a relatively long follow-up period (more than 1 year) with accurate measurements of the tip projection and columello-labial angle.
The PDS plate has been used in Europe and the United States for more than a decade, and it is a safe material in plastic surgery. It provides a scaffold for autologous tissue not as a point, but as a surface, resulting in greater strength. In addition, as a frame support, it can also be used for a range of applications, such as contour correction. Therefore, it is a good alternative synthetic material, particularly for Asian patients with weak and deficient nasal cartilage.