DISCUSSION
Various surgical techniques have been established as a means for performing mastectomy in transgender males within the framework of gender reassignment surgery. Depending on the patients’ breast features, different techniques may be utilized to reach an optimized result. As well as a peri-areolar approach, in which the mastectomy is performed through a key-hole procedure and circular peri-areolar mastopexy is simultaneously possible, a technique involving a large incision in the sub-mammary fold is often an option for patients with larger breast volume, skin excess, or impaired skin elasticity [
3,
4,
6]. The latter may be performed by
en bloc resection of lipoepidermal and glandular tissue and combined with a completely new positioning of the NAC through free grafting. Alternatively, excess skin may be deepithelialized leaving a lipodermal pedicle of the NAC, which then may be repositioned accordingly, as has also been described for mastectomy in male patients with gynecomastia by Kornstein and Cinelli [
7] as an option that “maintain(s) neovascular integrity and form.” Both large incision techniques result in a horizontal scar within the sub-mammary fold.
Hence, the surgical procedure needs to be adapted to the individual patient and breast anatomy. Different surgical techniques have been utilized to perform mastectomies [
8-
10], but all techniques have been derived from breast surgery for mammaplasty in female patients or gynecomastia treatment in male patients [
11-
13].
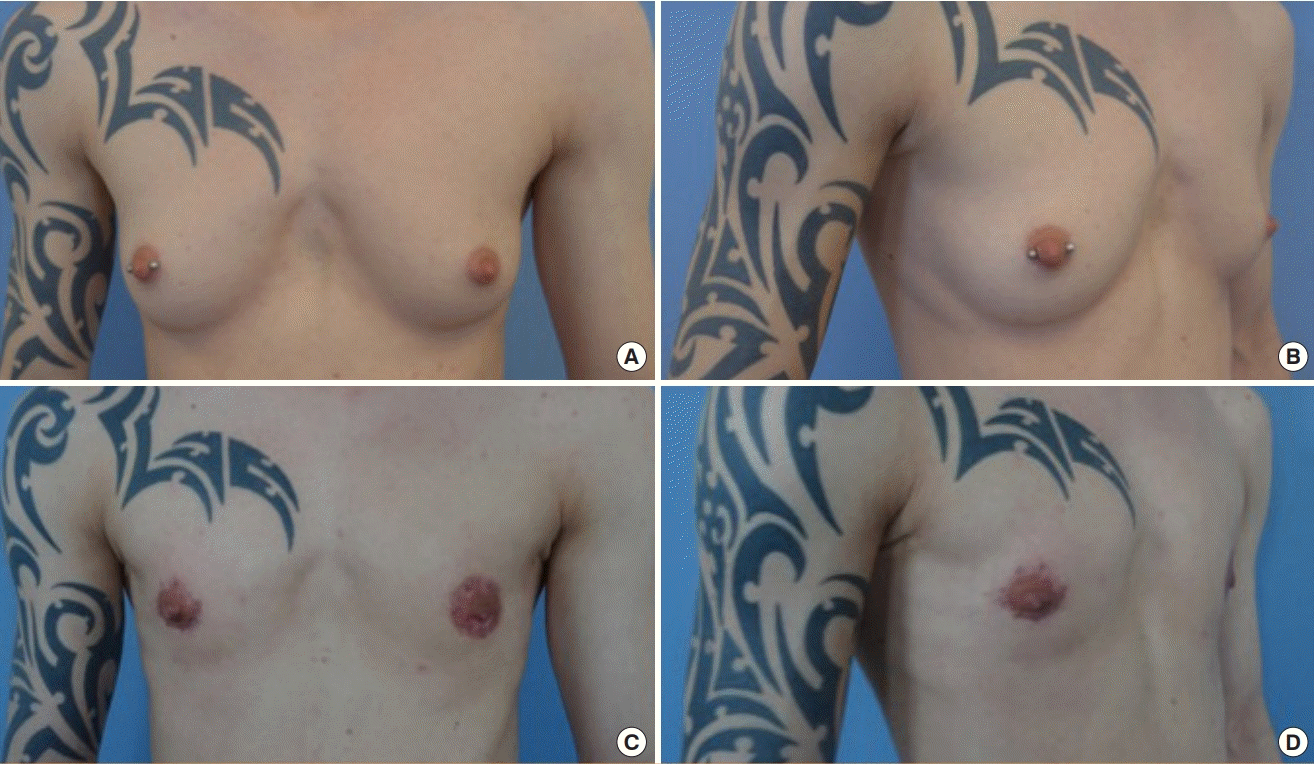
Glandular removal may be performed through a variety of incisions. In small breasts, glandular tissue can be removed through a semi-circular incision at the areolar rim (
Fig. 1). Here the glandular tissue is carefully dissected from the surrounding tissue and may be removed on bloc through the semi-circular peri-areolar incision, resulting in minimal scarring. Peri-areolar skin removal may be combined to perform simultaneous lifting of the breast. This minimal incision procedure is challenging due to minimal visual access for gland removal and difficulties involving hemostasis [
3].
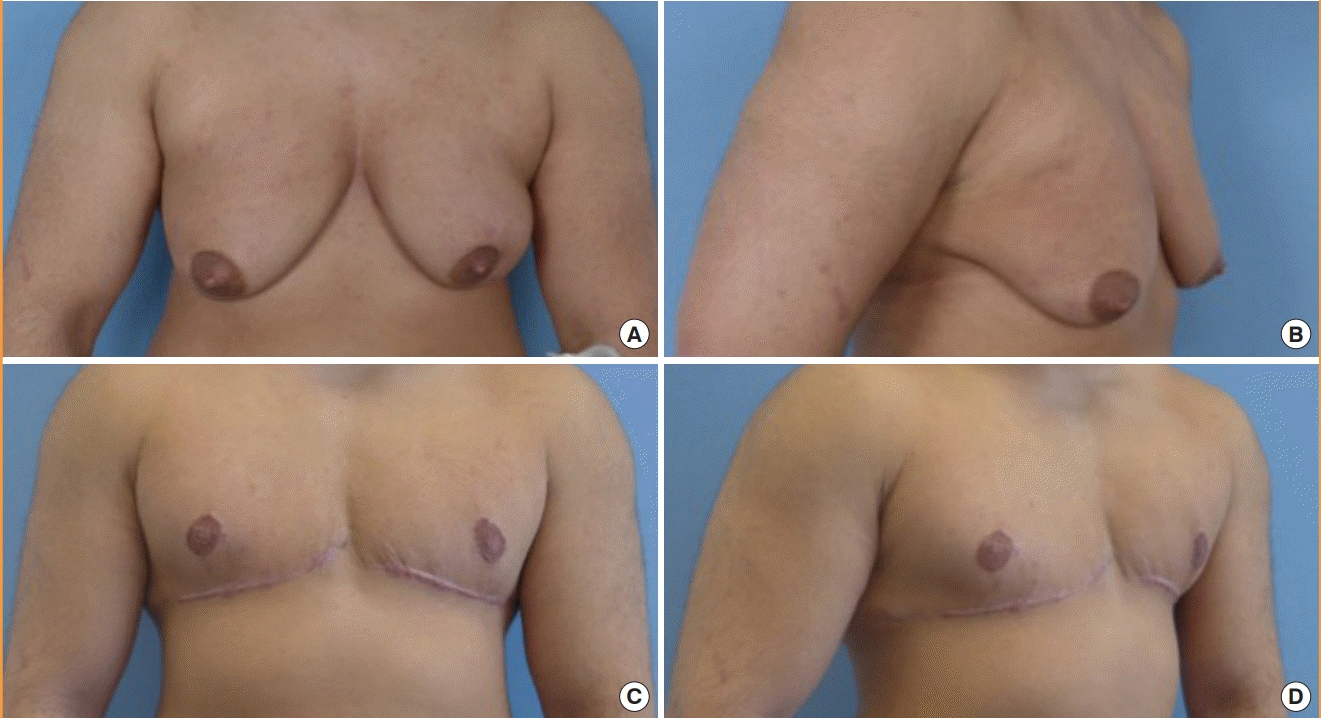
Larger breasts and those with ptosis require larger incisions, which may be achieved by performing a large inframammary incision along the complete width of the caudal breast fold, dissecting the glandular tissue to its cranial, lateral, and medial margins and performing a complete mastectomy including the glandular tissue with overlying skin. The NAC is then repositioned through free grafting [
14-
16]. This allows a thorough removal of glandular tissue with maximal visual access and safety, but it results in a long inframammary scar, as well as a peri-areolar scar, with a consequent lack of neural innervation of the NAC (
Fig. 2).
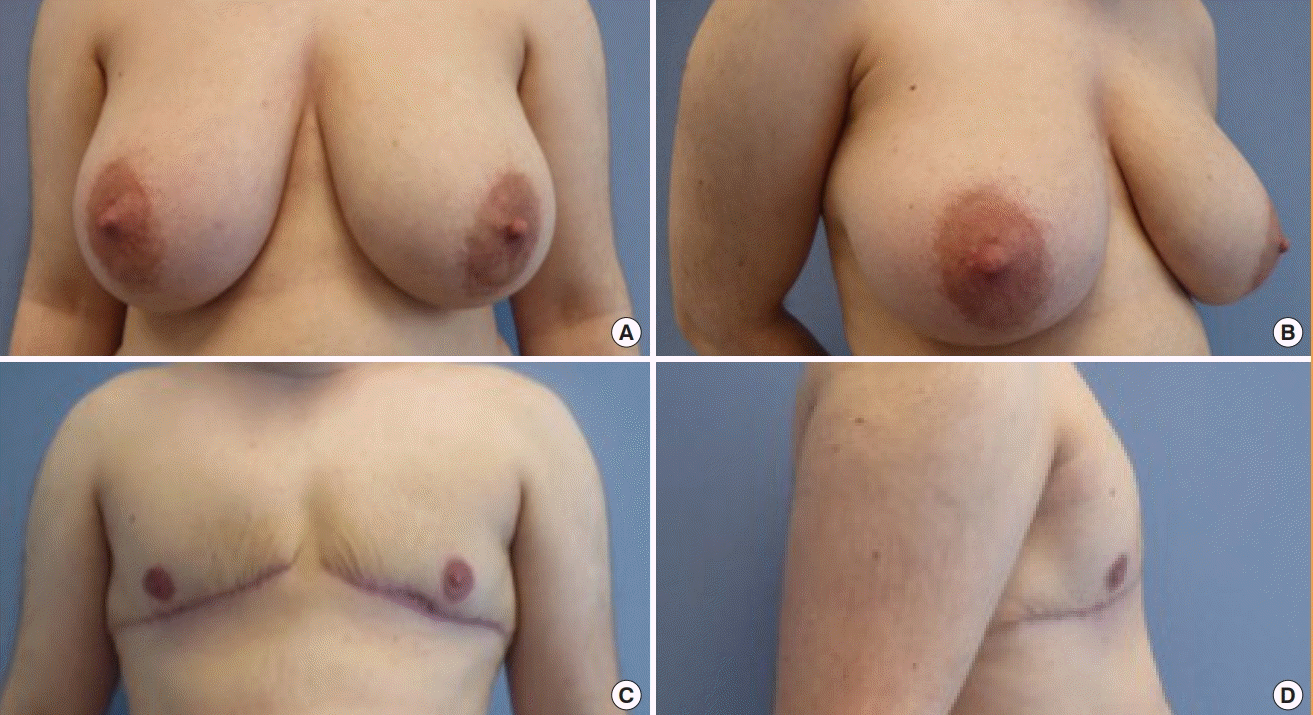
Another method, which also results in the latter scarring pattern, is to leave an inferior pedicled NAC, thereby preserving innervation of the NAC (
Fig. 3) [
6]. This technique has widely been utilized for female breast reduction [
17-
20].
The literature contains several algorithms that allow patient-based decision-making with regards to the surgical technique [
2,
5,
13]. Although slight differences are found between these algorithms, high congruence can be observed overall (
Table 4). Thus, small breasts with no or marginal ptosis and overall good skin elasticity are appropriate for areolar access without simultaneous breast skin lifting. Areolar access combined with skin reduction should be considered for medium-sized breasts and those with minimal or moderate ptosis and limited skin elasticity. Combined lipodermal and glandular breast resection or mastectomy with a lipodermal NAC pedicle should be considered for large breasts and those with severe ptosis and/or poor skin elasticity [
2,
5]. We have found our decision-making process regarding the choice of surgical technique to be consistent with these algorithms, although during the period of data-gathering of the present study a strict algorithm had yet to be established. Furthermore, it should be taken into account that the algorithms presented allow decision-making for optimized results in general, but surgeons will encounter transgender males with breast features not in exact accordance with the established algorithms. These cases benefit from an open and thorough dialogue with the patient regarding the different techniques and the corresponding possible expected outcomes, in order to encourage realistic expectations and to avoid dissatisfaction and disappointment to the extent possible. Furthermore, in our experience, awareness and self-education regarding different mastectomy techniques amongst transgender male patients are widespread. Patients are often well informed about different surgical mastectomy techniques and insist on a specific technique; for instance, they may knowingly opt for a peri-areolar approach despite a high potential risk of requiring revision surgery. In addition, body types are not always easily classified, which makes it difficult to strictly define a single suitable mastectomy technique in terms of a peri-areolar or sub-mammary approach to a certain individual habitus. A blurred transitional zone between different habitus types is not infrequent.
Table 3 outlines the differences in outcomes with respect to operative revision frequency in the current literature, as well as an overview of the frequency of the surgical methods used in our study compared to those used by other surgical departments. The differences in outcomes compared to those found in the current literature are small considering the wide range of published data on complication frequency. The occurrence of revisions in our study lies within the range found in the current literature (
Table 3).
Several surgical techniques were utilized to perform mastectomy, depending on individual factors, such as breast size and volume, as well as breast skin elasticity and breast ptosis, to obtain the best possible postoperative results. All techniques allow liposuction to be combined as a possible adjunct option for the refinement of chest wall contouring. Additionally, all mastectomy techniques used at our institution allow reshaping and size reduction of the areola in particular. For areolar incision methods, peri-areolar access may be selected and combined with circular peri-areolar reshaping and resizing of the areola, as well as breast lifting through the removal of excess breast skin circularly as described by Benelli [
13]. Similarly, trans-areolar access allows reshaping through removal of a central areola area. However, simultaneous breast skin reduction is not possible without creating additional scarring for trans-areolar incisions, and thus it should primarily be performed on patients who do not require simultaneous breast lifting in order to minimize postoperative scarring.
Surgical techniques solely using a peri-areolar incision allow glandular resection with or without skin resection, thereby enabling simultaneous breast lifting without creating additional scarring if performed as described by Benelli [
13]. Scarring is held at a minimum, which makes this technique attractive to both patients and surgeons. However, our results show that in procedures using these scar-sparing techniques, secondary corrections were found at a higher rate (48%) than in procedures performed using the sub-mammary incision technique (21%), despite resulting in more visible and greater scarring. By using minimal access techniques, such as an areolar incision, insufficient removal of the mammary gland resulting in a remaining female chest wall contour seems more likely compared to wide-scarring techniques, such as those using a sub-mammary incision to obtain access for glandular removal [
16]. Furthermore, skin resection is limited in areolar techniques, as a large amount of circular skin removal may lead to inadequate wound healing, because high circular traction may result in broad, visible, and disturbing scars. For patients with a great excess of skin, but poor skin elasticity, the removal of too little skin may lead to no or incomplete skin retraction, leaving the patient with an “empty”-looking breast that still resembles a female chest. This may explain the higher rate of secondary corrections being required for areolar incision techniques. Furthermore, regarding acute complications, Monstrey et al. [
4] found hematoma occurrence to be higher for areolar incisions.
Additionally, sub-mammary access with either combined resection of lipodermal and glandular components and subsequent NAC transplantation, as well as lipodermal NAC pedicle mastectomy, both allow reshaping and size reduction of the areola. In our findings, these two methods were used primarily for large-breasted patients, as reflected by the large average resection weight (
Table 2), as well as for patients with severe ptosis and poor skin quality, supporting the algorithms described previously (
Table 4). Large-access techniques allow an optimal view of the gland to be removed, which may allow more precise glandular resection and minimize the risk of remnants [
4]. However, these techniques result in larger scarring, which may be more noticeable. It has been discussed whether scarring plays an equally important role for FM patients as it does for female patients undergoing breast reduction or mastopexy [
4] and the literature as well as the findings of our study indicate that a male chest contour is prioritized above the use of scar-sparing techniques amongst FM patients. Another aspect to consider is NAC sensitivity, which commonly shows incomplete recovery after free NAC grafting, and to a lesser extent also after mastectomy with a NAC pedicle [
1]. This should be addressed and taken into consideration preoperatively.
Regarding the data and the timespan analyzed in the presented study, it is important to keep in mind that a strict algorithm had yet to be defined during the study period. At this time, our clinic has implemented the algorithms discussed above in order to obtain optimal results. Additionally, the presented data reflects the experience of a single-center, and hence several surgeons, over a period of 24 years. A strict consistency in the surgeons performing mastectomy cannot be met for this analysis.
As commonly described in the relevant literature, our findings also suggest that hematoma was the main cause for acute surgical revision measures [
5]. The literature suggests that hematoma is more frequently found in trans-areolar and semi-circular techniques than in large-access techniques that allow greater exposure [
4].
In conclusion, Besides the parameter of breast size, which predominantly determines the operative technique to be selected, surgeons should evaluate and consider skin elasticity as an important factor determining postoperative results and patient satisfaction [
4]. The overall frequency of secondary correction measures was high, especially regarding remaining skin excess as well as inadequate scar results, which were found to be the main reasons for secondary revision involving secondary chest wall contouring and scar revision, respectively (
Table 3). Remaining skin, and the resultant continued resemblance to a female breast contour or shape, seem to outweigh the length of the scars remaining after large-access surgical methods for FM patients. Hence, the results desired or expected by each individual FM patient and the individual emphasis of male chest wall contouring or low scarring should be addressed explicitly prior to surgery according to the chosen mastectomy method. As stated by Monstrey et al. [
4], “…with this group of patients, increasing the length of the scar on a masculine-appearing chest is far preferable to puckering, wrinkling, tethering, and especially excess skin.”