INTRODUCTION
Breast animation deformity (BAD), dynamic breast deformity, breast distortion, muscle flex deformity, and jumping breast are synonyms for a condition in which the shape of the breast changes or is distorted above an implant during contraction of the pectoralis major muscle (PMM) [
1]. The degree of BAD is variable; however, BAD often affects patients’ quality of life and the cosmetic outcomes of surgery [
2-
4]. The incidence of BAD has been reported to be as high as 77% following breast augmentation with subpectoral implant placement [
5]. Many recent papers have described BAD following implant-based immediate breast reconstruction and reported no incidence or a very low incidence of BAD; however, most such papers have neither described how the condition was assessed nor stated how they classified the different degrees of BAD [
6].
In 2008, Spear et al. [
5] developed a 4-point BAD grading scale for women undergoing breast augmentation. To our knowledge, the study by Spear et al. is the only study to have tested an assessment tool for BAD in a clinical setting; furthermore, the grading scale was developed for women who underwent breast augmentation, not for the assessment of reconstructed breasts. Overall, Spear’s grading scale is based on a visual assessment of two different aspects: whether the implant is placed in a subpectoral or prepectoral location, and the degree of distortion of the breasts. However, when assessing patients’ breasts after immediate breast reconstruction, we found that the main features of BAD were distortion of the skin and movement of the breasts. Based on these observations, we developed a tool specifically for the assessment of BAD following immediate breast reconstruction.
The popularity of implant-based breast reconstruction has increased over the last decade [
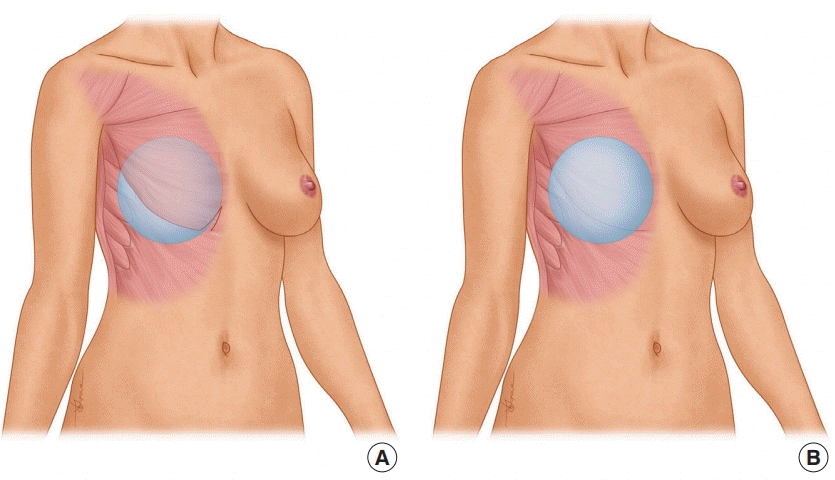
7]. Immediate breast reconstruction can be performed at the time of mastectomy by using various pocket planes, including prepectoral, partial muscle coverage, and total muscle coverage [
8]. The use of acellular dermal matrix (ADM) and lipofilling have facilitated a shift towards prepectoral implant placement [
9]. Prepectoral direct-to-implant breast reconstruction may reduce the incidence of BAD. However, its potential disadvantages include an increased incidence of capsular contracture, secondary ptosis, bottoming out, and visible wrinkling [
10,
11]. The aims of this paper were to assess and quantify the incidence of BAD in women undergoing direct-to-implant breast reconstruction with either prepectoral or dual-plane subpectoral implant placement, to develop a grading scale for the simple clinical assessment of BAD following direct-to-implant breast reconstruction, and to test the reproducibility of the grading system in a clinical setting by assessing its inter- and intra-rater agreement.
DISCUSSION
The degree of BAD following direct-to-implant breast reconstruction was significantly lower in patients with prepectorally placed implants than in those with subpectorally placed implants (
Table 3). Furthermore, all (100%) of the patients who underwent subpectoral direct-to-implant breast reconstruction were assessed to have some degree of BAD, which is higher than the value of 80% reported by Spear et al. [
5] in their series of women who underwent augmentation. The incidence of BAD in women who underwent reconstruction using the prepectoral technique was very low, which conforms to the results of our recent systematic review, where the incidence of BAD was found to be close to 0% following prepectoral implant placement in the included studies [
6].
Many studies have stated that the incidence of BAD was low when prepectoral implant placement was used for direct-to-implant breast reconstruction. However, it has rarely been reported how the degree of BAD was assessed [
6]. In this study, we have clearly defined and classified BAD using our classification system and described how the degree of BAD was assessed.
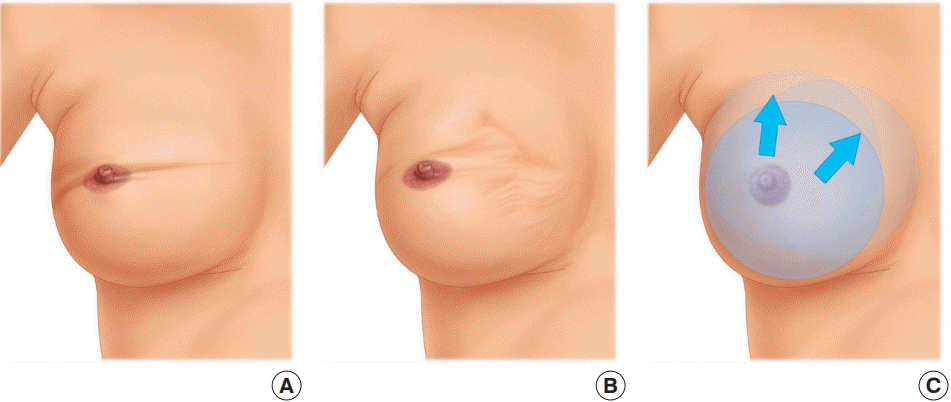
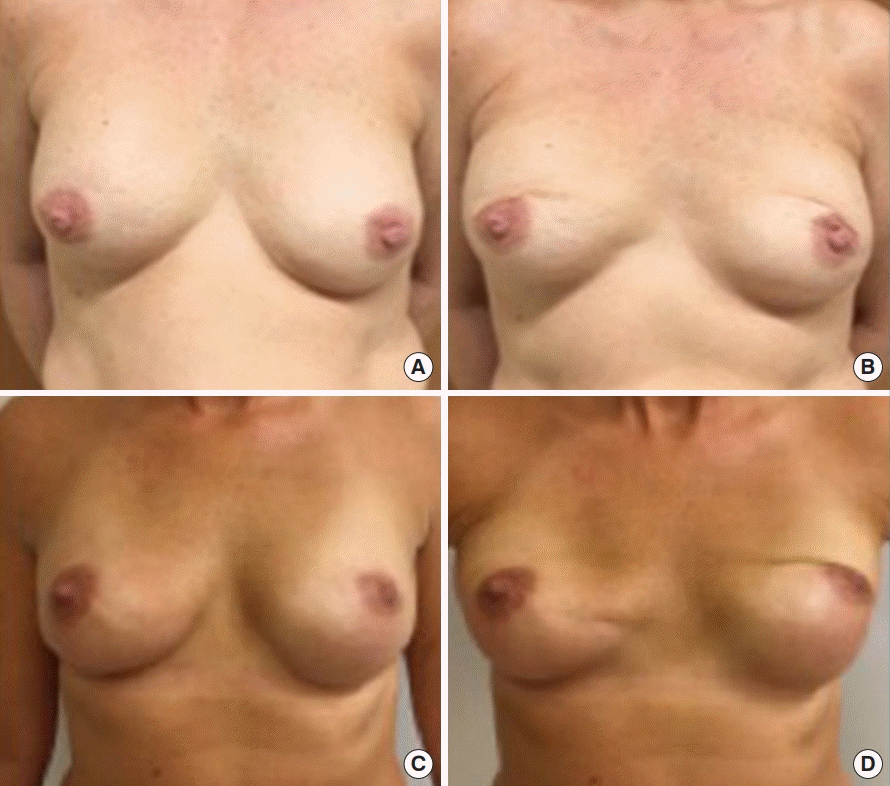
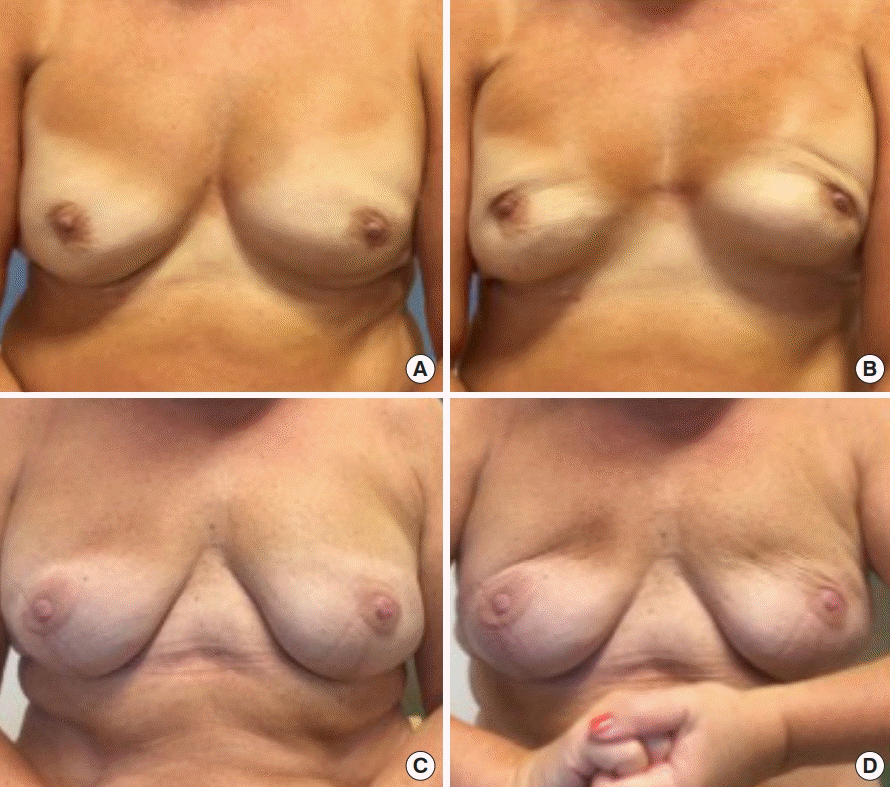
We used video recordings for our assessment of BAD. A major advantage of video footage is that dynamic recordings of the breast capture any deformity as it occurs during contraction of the PMM. We find videos to be superior to still photos for evaluating the degree of BAD. Video recordings also facilitate a reproducible evaluation by one or several observers to validate the assessment technique. When observing the videos of patients with direct-to-implant breast reconstructions, we found three areas of the breast that were affected by activation of the PMM: the TBM/NAC, the breast skin surrounding the TBM/NAC, and the movement of the entire breast. The clinical assessment was simple, using three grades, as described in detail above: no visible distortion/movement, visible distortion/movement, and severe distortion/movement. We sought to develop an accurate grading scale for BAD for women who have undergone reconstruction, which includes the main factors involved in BAD: distortion of the skin and movement of the reconstructed breast. We found that the degree of BAD was easy to assess using the three parameters of TBM/NAC distortion, breast skin distortion, and breast movement, scoring each from 0 to 2 based on the severity.
We used kappa statistics to test the intra- and inter-rater agreement in the assessments of BAD [
16]. The kappa values in the evaluation of our grading system were high, revealing high consistency in the results (intra-rater agreement, κ=0.6–0.7; inter-rater agreement, κ=0.7–0.8). The results revealed a high level of agreement in the assessment of BAD using our simple clinical NSE grading scale, suggesting that it can be used to assess the degree of BAD in a reproducible manner.
In comparison to Spear’s grading scale, in which the assessment is based on implant visibility, aesthetics, and distortion, we found that the assessment could be simplified by only considering the degree of BAD/distortion, which seems to be the most important factor leading to an unpleasing aesthetic result, accentuated implant visibility, and functional impairment following direct-to-implant breast reconstruction.
The kappa statistic is well-known as a tool to evaluate the reliability of diagnostic tests [
17,
18]. Its use in plastic surgery is, however, surprisingly scarce. In 2014, Ibrahim et al. [
19] used Fleiss’ kappa to evaluate aesthetic outcomes following two-stage breast reconstruction with or without ADM, and found kappa values ranging from fair to moderate.
Several methods have been proposed to assess BAD [
3,
7,
10,
20,
21]. Most recently, Fracol et al. [
21] suggested using Kim’s quantitative grading scale to standardize the grading of BAD by nipple displacement in centimeters and the percentage of skin area affected by rippling [
21]. Within the last 2 years, Cheffe et al. [
20] developed an objectively measurable scale to address the severity of BAD in women undergoing dual-plane augmentation. Landmarks on the breast were marked and analyzed on still photos with and without contraction of the PMM. In addition, Kummel et al. [
10] proposed a more detailed 3-point grading system to describe and distinguish grades of BAD in women undergoing augmentation and suggested how to prevent BAD by performing a two-stage procedure. Furthermore, Vidya and colleagues suggested how to manage BAD in relation to its grading for women undergoing subpectoral reconstruction [
7].
In a systematic literature review, we found that the majority of the proposed grading scales for BAD had not been tested for reproducibility [
6]. If a grading system is to be accessible for general use, it must be tested for reproducibility. The high intra- and inter-rater agreement obtained for our grading system confirms its reproducibility. The NSE grading scale is an easy-to-use, clinically relevant, consistent, and reproducible grading scale for assessing BAD in women who have undergone reconstruction; therefore, it constitutes a potential contribution to BAD grading in future clinical studies.
The duration of drain placement was significantly longer in the subpectoral group than in the prepectoral group. A retrospective analysis conducted in 2018 found comparable results between subpectoral and prepectoral reconstructions and no differences in seroma formation [
22]. The same conclusion was drawn in a recent large meta-analysis, where the authors found no significant differences in seroma formation between prepectoral and subpectoral reconstructions [
23]. In this study, we used one piece of ADM for both prepectoral and subpectoral reconstruction procedures. Therefore, the difference in seroma formation was not due to the number of pieces of ADM used. Instead, we believe that the difference may have been caused by the more severe surgical trauma that occurred when performing the subpectoral technique.
One of the limitations of this retrospective study is the difference in the duration of follow-up between the subpectoral and the prepectoral reconstruction groups. The follow-up in the prepectoral group was short, and the results should be interpreted with this in mind. We cannot rule out the possibility that the degree of BAD may increase over time in the prepectoral group. Future studies, preferably prospective randomized trials, with longer follow-up will be needed to elucidate this potential issue.
The number of papers on BAD describing its low incidence following prepectoral direct-to-implant breast reconstructions is increasing. However, although the incidence and degree of BAD seems to be minimized by using the prepectoral technique, there are also possible disadvantages of using this pocket plane. Specifically, there is a risk of wrinkling, capsular contraction, bottoming out, and visible implant edges. Long-term follow-up of women who undergo prepectoral reconstruction may reveal a substantial incidence of ptosis. Furthermore, this study only examined the degree of BAD following direct-to-implant breast reconstruction, and no patients reconstructed using a two-stage technique were investigated. The results should be interpreted in this context, and we cannot know whether the results are applicable for patients reconstructed using a two-stage technique.
Most importantly, we must keep in mind patients’ perceptions of BAD. Studies evaluating and comparing cosmetic and functional outcomes, as well as patient-related outcome measures, following prepectoral and subpectoral direct-to-implant breast reconstruction are needed. Surgeons may desire a shift towards the prepectoral technique, but is this wish also shared by patients?
The degree of BAD following direct-to-implant breast reconstruction was significantly lower in patients with prepectorally placed implants than in those with subpectorally placed implants. We found some degree of BAD in all cases of subpectoral direct-to-implant breast reconstruction. BAD can be assessed in a reproducible manner using the NSE grading scale. In conclusion, we have developed a supplementary grading scale that we believe is easy-to-use, clinically relevant, consistent, and reproducible for the assessment of BAD.