INTRODUCTION
Pectus excavatum (PE) or funnel chest is a congenital chest wall deformity with an incidence of 1 in 400 live births and a maleto-female ratio of 4:1 [
1,
2]. In female patients, the deformity commonly leads to a distortion of the female breast, resulting in so-called breast strabism with a diminished intermamillary distance [
3]. Females with PE tend to complain about the disturbing aesthetic appearance of their breasts and not about the sternal depression, which may be partly concealed by their breast tissues. Funnel chest resulting in a severe breast deformity may stigmatize a young woman, causing embarrassment, social anxiety, and other psychological disorders [
4]. Surgical correction of the deformity has been shown to improve patients’ quality of life and to have positive influence on self-perception [
5,
6].
Trying to correct the deformity by augmenting the breast with silicone implants may aggravate the strabism of the breasts by making the sternal inclination more prominent, which leads to unsatisfactory aesthetic results [
3]. Instead, as we have demonstrated in previous publications, remodeling the anterior thoracic wall with retrosternal metal bar implantation by a minimally invasive repair procedure (MIRPE) [
7] or by a modified approach with a semi-open technique (minor open videoendoscopically assisted repair of pectus excavatum; MOVARPE) [
8] corrects the underlying deformity and leads to a marked improvement in the appearance of the breasts [
3].
Aesthetic correction remains a major indication for PE repair and is the most difficult parameter to measure postoperatively. The patient’s satisfaction with a procedure and the surgeon’s evaluation of the postoperative results can differ [
9,
10]. The aim of this study was to investigate the association between female patients’ personal outcome evaluations and the assessments made by medical professionals. Standardized photographs of patients’ preoperative and postoperative aesthetic appearance were analyzed by patients and by medical professionals. Differences in the evaluation based on evaluators’ sex or degree of medical education were determined. Furthermore, we assessed whether the surgical intervention had an impact on the psychosocial well-being of the female participants. To our knowledge, no publications have yet investigated quality of life, satisfaction, body image, and aesthetic results before and after bar removal with an exclusive focus on female PE patients.
DISCUSSION
In the present study, we focused on the aesthetic appearance, quality of life, and body image of female adult and adolescent patients before and after PE repair. Most previous studies concentrated on this deformity in males [
11,
12,
14] or even excluded female subjects from their studies [
15]. We focused on a female cohort, since the secondary breast deformity in females aggravates their symptoms and has a pronounced effect on body image. Since PE has been shown to cause only minor functional deficits [
16], insurance coverage is not always provided and the surgical correction of PE is sometimes still dismissed as a merely aesthetic procedure. However, many studies have clearly shown that the PE deformity has a significant influence on psychosocial development and that the benefits of surgical correction are not limited to aesthetic improvements [
11,
12,
14,
17].
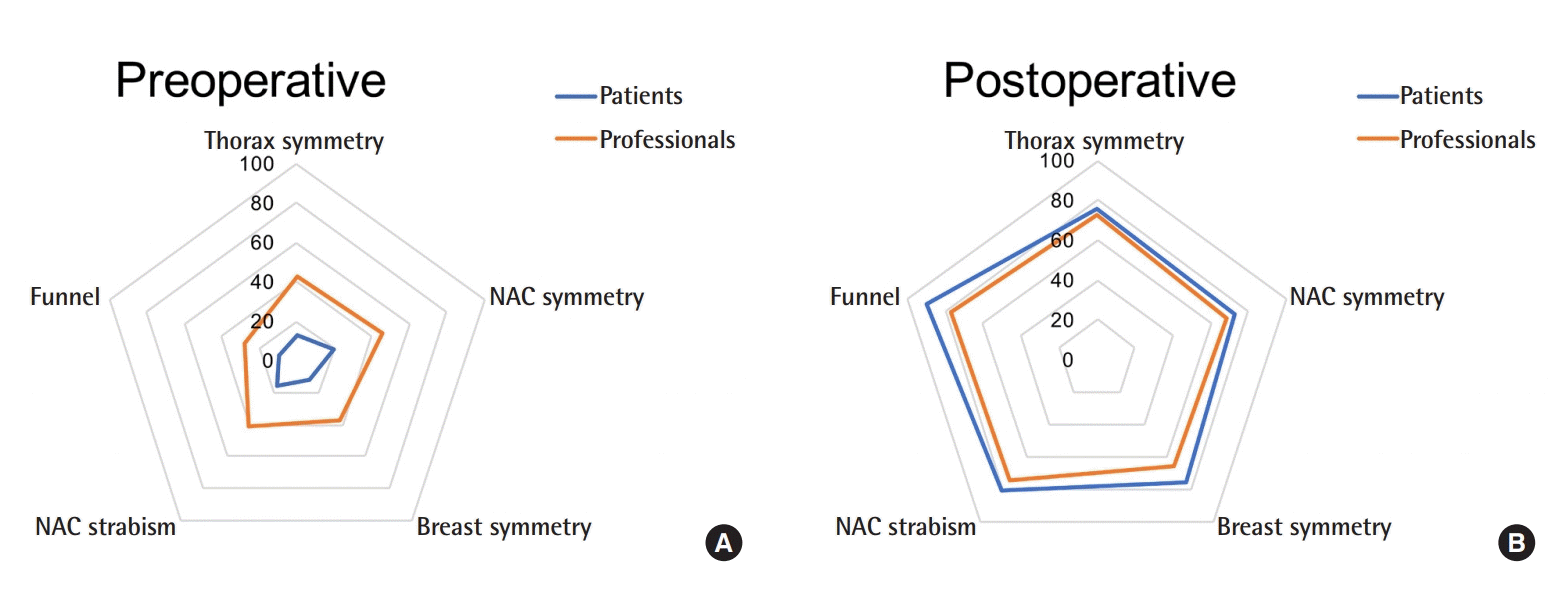
Our study demonstrated that female patients rated their preoperative deformities far worse than medical evaluators. Postoperatively, patients rated their appearance equal or slightly better than the medical evaluators. This indicates that the PE deformity strongly impacted patients’ self-perception and that surgical correction successfully led to a self-evaluation that was in accordance with the other evaluators. We found only minor differences in the evaluations of male or female professionals and little impact of their degree of medical education.
Many reports about psychological health in PE patients have examined largely pediatric or adolescent patient series and have mainly included males [
4,
11,
12,
17,
18]. The present study focused on both adolescent and adult female patients, ranging from 14 to 41 years of age. Studies have shown significant improvements in psychological and psychosocial well-being after PE repair in children [
5,
12] and young adults [
11], but the results of these studies were not based exclusively on females. Our psychological questionnaire confirmed the improvements in quality of life and psychological well-being after surgery, specifically in female patients. As stated previously, this is of particular importance because the PE deformity leads to an overall more severe aesthetic distortion in female patients than in male patients, as a result of the resultant breast deformity. Furthermore, previous investigations have usually evaluated patients before removal of the pectus bar [
5,
11,
12]. Several investigators have pointed out that data on quality of life after bar removal were not available, although these data are needed to justify performing the Nuss or MOVARPE procedure for aesthetic reasons. So far, only three reports have included postoperative evaluations, and all of these demonstrated high patient satisfaction with the results of the Nuss procedure after removal of the pectus bar [
18-
20]. To our knowledge, our study is the first to evaluate female PE patients’ quality of life and satisfaction after bar explantation.
Many studies on aesthetic outcomes after breast surgery have confirmed that patients and medical professionals have different perceptions of the results [
10,
21]. Previously, we conducted a study comparing the aesthetic evaluations of patients, medical professionals, and laypersons after implant-based breast reconstruction [
9]. In oncologic patients, we showed that patients rated their postoperative results significantly more positively than the other evaluators. Similar findings have also been reported in other studies on breast cancer patients, indicating that the differences in evaluations among patients, physicians, and laypeople are not based only on aesthetic criteria; instead, they are multifactorial [
10]. These results in oncologic patients are in contrast to the results of the current study on PE repair, where only the preoperative evaluations showed different ratings between patients and the other evaluators. The postoperative evaluations yielded similar aesthetic ratings in all groups. In our view, this may confirm that PE repair corrects not only an aesthetic deformity, but also has a positive influence on patients’ self-perception.
Interestingly, a study by Kim et al. [
19], evaluating satisfaction after pectus bar removal in 39 children through a questionnaire, came to a different conclusion. The operative results were evaluated by the patients and their parents, as well as by two surgeons and two nurses. The surgical team’s scores for overall satisfaction were higher than the patients’ and/or parents’ scores, and the same pattern was found for the scores for recommendation of the surgery to others. The authors suggested that preoperative expectations different among patients, parents, and the surgical team, and that a sufficient clarification should therefore be provided prior to surgery. We agree that patients and their parents should be thoroughly informed before surgery in order to ensure that they have realistic expectations regarding outcomes.
Patient satisfaction has become an important tool as a measure of the quality and outcomes of medical care [
22]. A review of patients’ evaluations of medical services that included results from over 50 studies showed that the average percentage of satisfied patients was about 78% [
23]. The most common assumption is that satisfaction is defined as an “evaluation based on the fulfillment of expectations” [
24]. Various studies have tested this theory and have come to the conclusion that there is evidence to suggest that patients’ expectations are involved in evaluations, but not in a simplistic way [
22,
25]. Expectations are modified throughout the process of care and influence evaluations. A discrepancy model has been proposed, suggesting that dissatisfaction is only expressed when an extreme negative event occurs, and that the expression of dissatisfaction is likely an indicator that something went wrong [
24]. Therefore the high satisfaction rates in most studies are a questionable measure of medical quality, and the satisfaction questionnaires used in studies are still based on an insufficient knowledge of how and what patients evaluate [
24].
In accordance with these points, objective measures were analyzed in our study, and differences were still present between medical evaluators and patients. This suggests that factors beyond objective criteria influenced the evaluations.
Since self-perception is a major contributor to therapeutic decision-making, a systematic evaluation of body image should be included in the assessment of patients with thoracic wall deformities. A multidisciplinary approach, including a psychological evaluation, is mandatory for the treatment of PE deformities, and psychological screening should routinely be carried out in all patients with thoracic wall deformities. The careful selection of patients following multidisciplinary preoperative management is important for preventing disappointing results.
The limitations of this study are its retrospective data acquisition nature and the small number of patients included, which limited our ability to draw generalizable conclusions. Nonetheless, this study presents the largest experience to date, with the longest follow-up of female patients who underwent PE repair with retrosternal pectus bar implantation. Further work is needed to verify that the information the current study obtained from a small number of patients is representative of a larger population.
In summary, our results show that female patients with a PE deformity and secondary breast deformity can greatly benefit from surgical correction, with high levels of satisfaction and improvements in their quality of life. We therefore conclude that corrective surgery of PE has a positive effect on patients’ physical and psychological well-being. Psychological improvement through aesthetic correction of the deformity is an indication for surgery.