INTRODUCTION
Anterior neck burns represent a particular reconstructive challenge as this body area is under continuous tension due to its wide range of motion [
1]. The quality and quantity of skin required for satisfactory reconstruction of this area remains a difficult goal [
2], and contractures can limit neck extension, cause persistent pain, headaches and depression, leading to a poor quality of life [
3]. Various reconstructive techniques have been described including split-thickness skin grafts (STSGs), local flaps, local flaps combined with STSGs, expanded local flaps, thin pedicled flaps, free flaps, and expanded free flaps [
4], but patient outcomes are highly variable. In this study, we developed a butterfly design of the anterolateral thigh (ALT) flap to specifically address the post-resection skin defect. We describe the surgical technique involved to achieve restoration of neck extension in burn reconstruction.
IDEA
Butterfly design of ALT flap
Preoperatively, Doppler ultrasound [
5] and computed tomography angiography were performed for evaluation of suitable perforators arising from the lateral circumflex femoral system. Intraoperatively, the patient is positioned supine with the neck in hyperextension. Two teams work simultaneously–one excises the anterior neck scar with respect for the aesthetic unit of the neck and prepares the recipient vessels (external jugular vein, facial and superior thyroid arteries) while the other team designs and harvests the ALT flap.
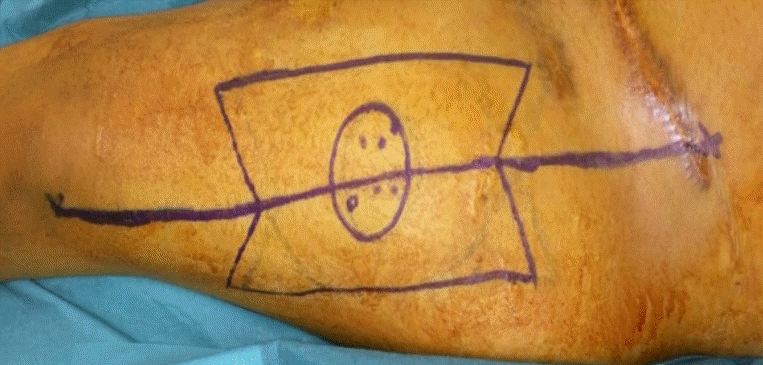
The ALT is designed in a butterfly shape corresponding to the post-resection defect with previously identified perforators located in the middle of the flap (
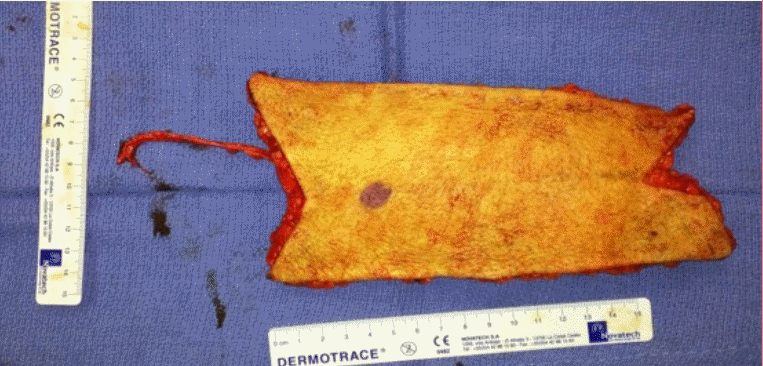
Fig. 1). The flap is then harvested sub-fascial and anastomosed end-to-end to the superior thyroid artery and external jugular vein. Because of the butterfly shape design of the ALT flap (
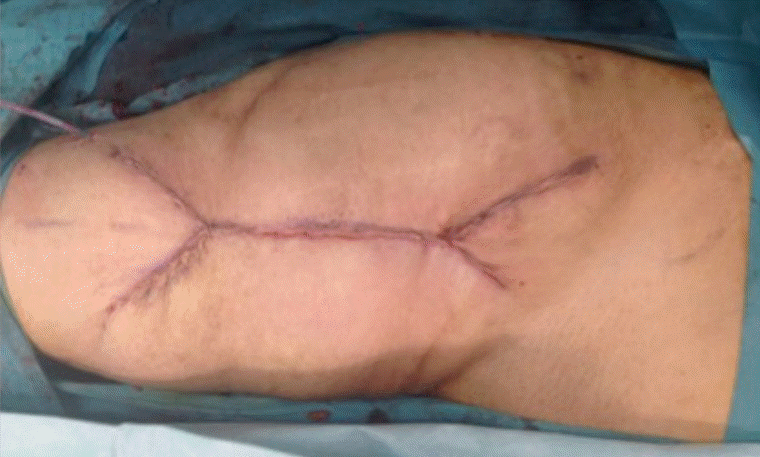
Fig. 2), the donor site can be closed in V-Y fashion at both proximal and distal ends (
Fig. 3).
Cases
Case 1
An 11-year-old boy from Saudi Arabia presented with severe anterior cervical contracture (based on range of neck extension according to Makboul’s classification system [
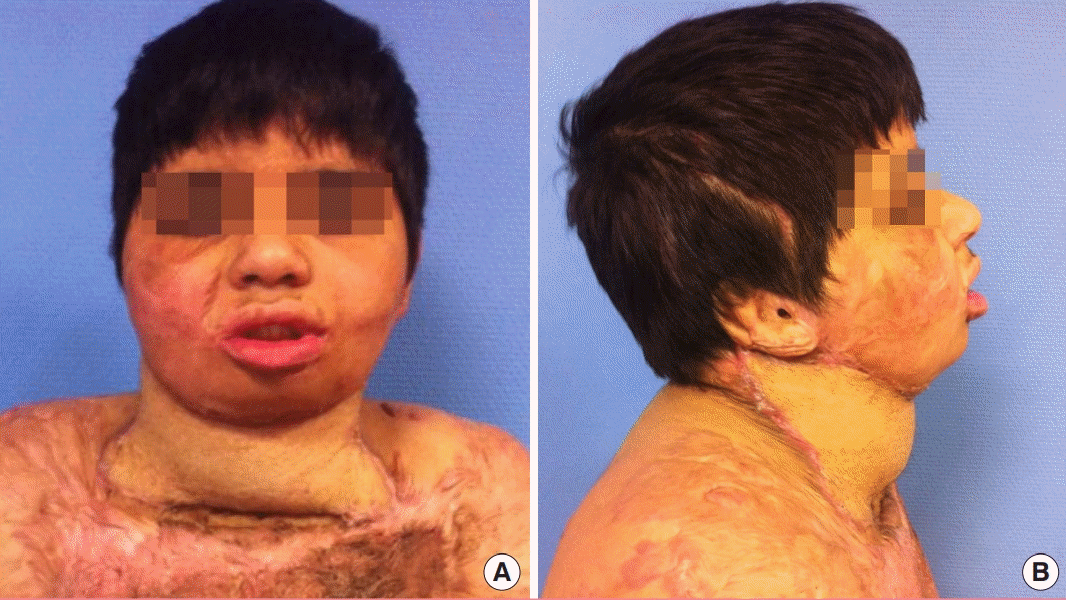
6]: mild, 95°–110°; moderate, 85°–95°; severe, < 85°). His parents gave their consent. He had previously sustained thermal burns involving 40% of total body surface area (TBSA) due to an oven explosion when he was 6 years old, and was treated initially with excision and STSG at another facility. Intraoperatively, the excision defect was 19 × 10 cm and resurfaced with a butterfly design ALT flap. At 4 years’ follow-up, neck extension had improved from 83° preoperatively to 120° without recurrence of scar contracture. Liposuction of the ALT flap was performed at 1-year post-operative to further improve neck contour (
Fig. 4).
Case 2
A 23-year-old woman from Saudi Arabia presented with moderate anterior cervical contracture similar to case 1. The patient gave her consent. TBSA was 45% with mainly upper body involvement and she was also initially treated with excision and STSG at 8 years old. The burn scar was excised and resurfaced with a 15 × 8 cm butterfly design ALT flap. At 4 years’ follow-up, neck extension was 120° from 90° preoperatively without any evidence of contracture recurrence. Similarly, she underwent a secondary contouring procedure with liposuction at 1-year postoperative to improve her aesthetic outcome (
Fig. 5).
DISCUSSION
Following burn injury, neck contractures may develop due to various reasons. Most commonly, this results from damage to deeper tissues leading to significant functional and aesthetic deficits of the lower face and neck including the upper chest [
7] or progressive contraction and hypertrophic scarring due to failure of skin grafting [
8]. When more than two-thirds of the anterior neck is involved, loco-regional options become severely limited; STSGs are also far from ideal due to their inherent poor cosmetic result, in addition to the need for prolonged immobilization and pressure dressings [
9]. Furthermore, Asian patients tend towards a greater inflammatory response to wounding and therefore, are at greater risk for developing burn contractures [
10].
Free tissue transfers provide full-thickness skin for superior resurfacing and have previously been demonstrated to be reliable and safe for reconstruction of head and neck burns, with a technical success rate of 94% [
8]. However, this is not without its drawbacks such as the need for a prolonged, complex procedure and the near obligatory requirement for future debulking procedures (up to 64% incidence) [
8]. With improved anatomical knowledge, thinner, wider and larger flaps such as the free fascio-cutaneous ALT flap can now be utilized to address the challenges of reconstructing anterior neck burn contractures. Various modifications to further optimize the use of the ALT for this purpose include pre-expansion to thin out the flap further [
11] and prefabrication at distant sites to obtain a thinner flap [
8]. These procedures are all staged however, and are not without risks of infection and pedicle thrombosis respectively.
In proposing our butterfly design for the ALT flap, we hope to provide a simple modification to further improve on the aforementioned advancements. By matching the dimensions of the skin defect better following scar excision, this would enable wound closure to have less tension as compared to the traditional, elliptical design of the ALT flap during insetting. In turn, this may help maintain flap mobility and that of the reconstructed neck at the cervico-mental angle, thereby further reducing the risk of developing scar contractures. Additionally, the butterfly design of the ALT flap renders the donor site at the thigh amenable to closure in V-Y fashion, which would arguably reduce the risks of further donor site morbidity such as dehiscence and/or need for additional skin grafting.
In both cases, platysmaplasty was not necessary as the muscle was not involved nor scarred. There were no local complications such as flap losses or donor site dehiscence. Length of hospital stay was 7 and 5 days respectively without the need for extra rehabilitation. Neck extension improved by 37° and 30° to normal ( > 110°) at 4 years’ follow-up with no evidence of contracture recurrence. While further debulking was required in both patients, this is a trade-off that can be performed on an outpatient basis and the risks of which would certainly be better tolerated compared to the need for multiple staged procedures. Ultimately, we believe that this butterfly design of the ALT flap is valuable for both primary and secondary reconstruction of anterior neck burns and affords all the advantages of free tissue transfers without the inherent risks of multiple staged procedures.