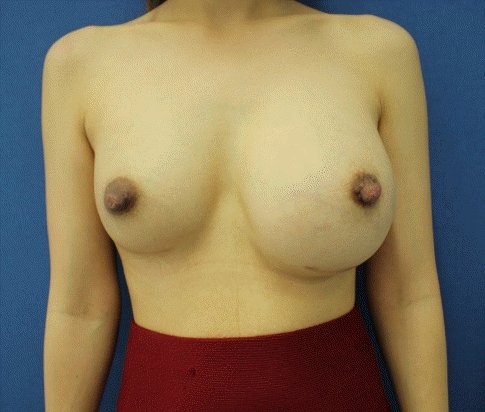
A healthy 32-year-old woman underwent breast augmentation 3 years ago with an anatomical textured silicone implant (Silimed, Rio de Janeiro, Brazil) placed in the subpectoral plane. She reported swelling in the left breast for 2 weeks. The area of swelling had been growing, without tenderness or fever. She stated that she had not experienced any trauma or accidents in the area of the breast. No adverse events had occurred during the perioperative and recovery periods. Upon examination, asymmetry of the breast was noted, without erythema or ecchymosis (
Fig. 1). The axillary lymph node could not be palpated. Hazy, pale-yellow periprosthetic fluid (150 mL) was drained from the swollen breast and sent for bacterial culture, cytology, and immunohistochemistry. The bacterial culture revealed no growth. Fluid cytology yielded some large atypical mononuclear cells, few histiocytes, and few small lymphoid cells on a proteinaceous background. The large atypical cells had a moderate amount of cytoplasm, intracytoplasmic vacuoles, irregular nuclear shape, lacy hyperchromatic nuclei, and small nucleoli (
Fig. 2). Immunohistochemically, the cells were positive for CD30, CD4, CD5, CD43, CD56, TCR-beta F1 (weak), and TIA1, and negative for CD2, CD3, CD7, CD8, CD20, CD68, and ALK (
Fig. 3). The diagnosis was BIA-ALCL. A multidisciplinary approach involving collaboration with a radiologist and oncologist was set up. Magnetic resonance imaging showed no evidence of lymphadenopathy or any suspicious mass at the capsule or inside the breast parenchyma. The surgical approach used an existing inframammary scar. The patient underwent bilateral removal of the implant, ipsilateral total capsulectomy, and removal of yellowish fibrinous material around the implant (
Fig. 4). The posterior capsule was injected with saline containing adrenaline in the rib area to facilitate removal. The entire capsule was care fully evaluated. The inner surface of the formalin-fixed capsulectomy specimen showed two shallow, irregularly-shaped ulcers measuring 1.7 × 1.5 × 0.2 cm and 1.5 × 0.5 × 0.2 cm, respectively, that were coated with a thin friable yellow material (
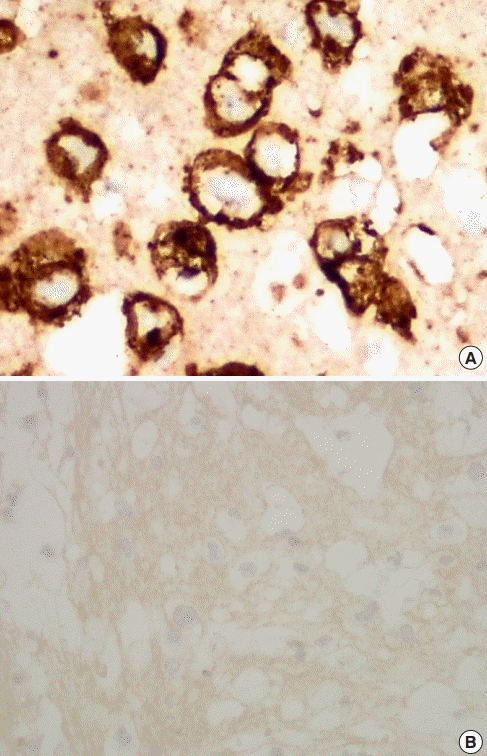
Fig. 5). The excised breast capsule was evaluated by hematoxylin and eosin staining. A histological section taken from the ulcer revealed a few large atypical cells with hyperchromatic nuclei embedded in the amorphous eosinophilic proteinaceous material, along with a few histiocytes and small lymphoid cells in the fibrous wall below (
Fig. 6A). CD30-positive tumor cells were located within the amorphous material coating the inner surface of the capsule, and no capsular invasion was observed (
Fig. 6B). The patient was categorized as having stage 1A disease [
6]. After complete surgical resection, she continued regular follow-up with her oncologist and plastic surgeon, and has shown no evidence of disease for 2 years.