INTRODUCTION
Among the various traumatic injuries treated at emergency departments, fingertip injuries are the most common and require prompt and adequate intervention for favorable outcomes [
1]. We defined the fingertip as the portion of the digit distal to the insertion of the flexor and extensor tendons on the distal phalanx [
2]. For amputated fingertip injuries, microsurgical replantation of the amputated fingertip to the stump is needed to achieve satisfactory recovery with regard to the length and function of the injured finger [
3]. However, microanastomosis of the fingertip amputation distal to the germinal matrix of the nail is difficult and requires an experienced microsurgeon. In cases of crush injury in particular, the injured vessels of the fingertip are not suitable for microanastomosis [
4,
5]. Without early microanastomosis, the expected outcome is not favorable. Therefore, a composite graft with the distal stump can be a treatment option. Composite grafting of the fingertip is affected by plasma imbibition and vascular inosculation through the cut edges, and its success rate is associated with delicate surgical procedures and postoperative care [
6]. To improve the survival outcomes of composite grafts, many adjuvant methods can be used [
7-
11].
Hyperbaric oxygen (HBO
2) therapy is well known for its many positive effects on wound healing [
12]. Previous animal studies have shown that the application of HBO
2 to composite grafts in rats and rabbits increased graft survival [
13,
14]. Systemic HBO
2 treatment increases oxygen diffusion, improves the condition of ischemia-reperfusion injuries, and stimulates angiogenesis [
12]. For compromised flaps and grafts, HBO
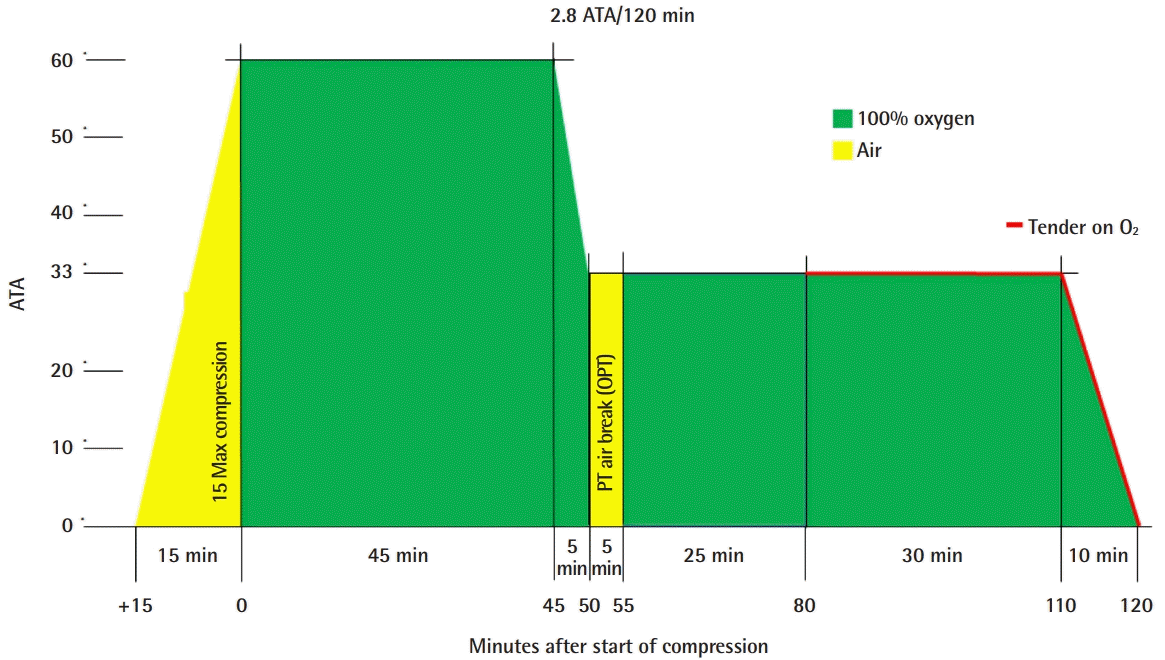
2 is typically applied at 2.0–2.5 atmospheres absolute (ATA) for 90- to 120-minute periods twice daily [
15]. For split-thickness skin grafts, the application of HBO
2 before and after surgery can improve the survival rate [
16]. Many trials have been designed to verify the effect of hyperbaric therapy on composite grafts in animal studies. However, few clinical comparison studies have been conducted to analyze the effect of systemic HBO
2 on composite grafts in humans. This study was conducted to evaluate the effect of systemic HBO
2 on composite graft survival in cases of amputated fingertip injury.
DISCUSSION
In this study, we evaluated the clinical effect of HBO2 therapy on composite graft survival in cases of fingertip injury. Fifty-five fingertip injuries treated with composite grafting were included in the analysis. These composite graft cases included 28 cases of graft success (50.9%) and 27 cases of failure (49.1%). Age, sex, hypertension, diabetes mellitus, smoking history, the mechanism of the injury, and the geometry of the injury were reviewed as baseline characteristics. The conventional and HBO2 groups showed no statistically significant differences in these baseline characteristics.
HBO
2 treatment involves the administration of a high concentration of oxygen in a high-pressure environment, with the patient breathing 100% oxygen at a pressure of 1.4 atmospheres or higher [
19]. HBO
2 can be applied at pressures of 2.0–3.0 ATA for periods of 1 to 4 hours. The arterial PO
2 becomes elevated to 1,000–1,500 mmHg due to dissolved oxygen in the plasma. At the tissue and cellular levels, hyperoxygenation promotes angiogenesis and improves post-ischemic tissue survival. Increasing the applied pressure increases the PO
2 of the tissue, which is beneficial for wound healing [
20].
Most oxygen transported through the blood is carried in the form of oxyhemoglobin; specifically, 20 mL of oxygen is attached to hemoglobin per 100 mL of blood at standard atmospheric pressure. In contrast, only 0.3 mL of oxygen is dissolved in the plasma per 100 mL of blood. If the atmospheric pressure is raised to 3.0 atmospheres, the partial pressure of arterial oxygen reaches 2,200 mmHg. The dissolved plasma oxygen level increases from 0.3 mL to 5.4 mL, which is about 18 times the level at standard atmospheric pressure. This elevated partial pressure of oxygen can provide enough oxygen to maintain basal metabolic function without normal hemoglobin, which is the principle of HBO
2 treatment [
12].
In addition to hyperoxygenation, as a secondary mechanism, HBO
2 promotes tissue regeneration and neovascularization in skin grafts and flaps [
16]. The effect of HBO
2 on skin grafts and flaps is thought to improve wound oxygen tension, fibroblast function (collagen synthesis), and vascularization [
15]. Large amounts of animal data and multiple serials of clinical case reports have been published regarding the effectiveness of HBO
2 in skin grafts, composite grafts, and flap ischemia. Even though many studies have discussed the efficacy of HBO
2 in grafts and flaps, comparative clinical studies of HBO
2 are rare, as it is challenging to collect identical cases to compare. Evaluating the effect of HBO
2 alone is also difficult due to the challenges associated with obtaining patient consent to observe the flap or graft without additional adjunct therapy.
Before conducting the data analysis, we hypothesized that HBO
2 would be effective in the treatment of fingertip injury. We also expected that HBO
2 treatment would be more beneficial for crush injuries than for guillotine injuries. Generally, the survival of a composite graft after a crush injury is more difficult to attain [
21]. Thus, we compared the success rate according to HBO
2 treatment status for guillotine and crush injuries. For both the conventional and HBO
2 groups, guillotine injuries were associated with a significantly higher proportion of successful outcomes than crush injuries (
Table 3). The results also showed that HBO
2 treatment increased the graft survival rate in patients with guillotine-type fingertip injuries. However, in the crush injury group, HBO
2 therapy did not significantly affect graft outcomes. Considering the mechanism by which HBO
2 increases graft survival by promoting angiogenesis caused by hyperoxygenation, we hypothesized that the crushed amputation was unsuitable for angiogenesis or neovascularization. Therefore, crush fingertip injuries treated with composite grafts do not appear to be an appropriate indication for HBO
2 treatment.
Another outcome that we considered was healing time. The HBO2 group showed a median healing time of 3 weeks, while the median healing period for the conventional group was 4 weeks. This difference in healing time was statistically significant, with a statistical power (1–β) of 85.5%. The shorter healing time in the HBO2 group could be related to faster restoration of the function of the injured finger and a reduction in the number of clinic visits.
This study had a few limitations. First, it was retrospective in nature. The outcomes were reviewed only through images and the descriptions in the electrical medical records. Some data were missing, and not all information on necessary parameters could be obtained. Second, the statistical analysis was limited. This study included only patients from a short period, and information was collected from a single center representing only one region. To overcome the limitation of the small sample size, we collected the data consecutively. Lastly, during the study period, we only had one multiplace chamber, so we could not differentiate the HBO2 treatment protocol by indication; rather, we had to apply a single treatment protocol for every patient. Differences in the applied pressure and the number of HBO2 treatments per day may affect the wound survival outcome. Future studies may be used to develop an optimal treatment protocol.
HBO2 treatment effectively facilitates composite graft survival in guillotine-type fingertip injuries. HBO2 can also decrease the time required for the composite graft to heal. HBO2 therapy appears to increase survival rate and improve healing time in fingertip injuries treated with composite grafting, and it is considered to be adequate to perform in cases of guillotine injury, where the cutting surface is relatively clean. However, the effect may not be significant in cases of crush injury, so we expect that additional adjuvant therapy or another reconstruction plan will be required. Additionally, future randomized controlled trials with adequate sample sizes may be needed.