INTRODUCTION
Nasal tip surgery is pivotal in rhinoplasty, and a large part of this process consists of interventions on the lower lateral cartilage (LLC). The LLC, also known as the major alar cartilage, is a pair of V-shaped cartilages supporting the medial and lateral walls of the nostril and forming the dome of the nasal tip.
The trimming of the cephalic part of the LLC alters the anatomy of the alar part of the nose. Cephalic trimming of the LLC may cause long-term sequelae and many potential complications, which are divided into functional and aesthetic issues: functional issues include collapse of the valve, while aesthetic issues include alar retraction, nasal tip asymmetry, a pinched tip, and the loss of aesthetic projection [
1].
Deformities of the LLC may lead to functional and aesthetic handicaps; therefore, its width and length are critical for the outcomes of nasal tip surgery. Typically, the mean horizontal length of the lateral crus is 12 mm, and the vertical width is half of its length—about 6 mm [
2]. To have better aesthetics of the nasal tip and preserve the supporting function of the LLC, a thickness of the LLC of at least 0.7 mm was suggested [
3]. Furthermore, connections of the LLC with the upper lateral cartilage (ULC) through ligaments and attachments to the adjacent soft tissue, such as the skin, are crucial. The cephalic part of the lateral crus of the LLC plays a significant role in nasal tip deformation, such as bulbous nasal tip formation, boxy or pinched nasal tip deformity, and drooping nasal tip [
4].
There are many manoeuvres to increase nasal tip projection and reshape a wide tip. These manoeuvres include sutures, grafts, and flaps. Currently, cephalic trimming is frequently preferred by surgeons. The main limiting factor of cephalic trimming is the formation of dead spaces, which in the long term may cause uncontrolled scarring during recovery and an unnatural nasal tip definition. Cartilage grafts are effective in many cases, such as those involving weak or concave lower lateral crus, but they also pose risks, such as resorption, malposition, or distortion of the LLC or palpation of cartilage by patients [
5,
6].
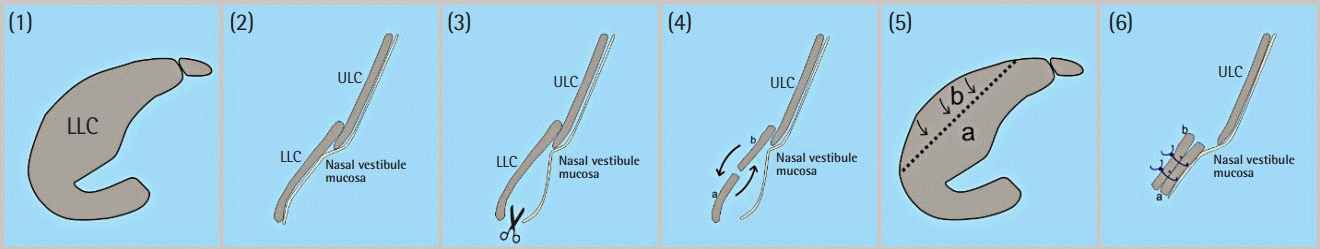
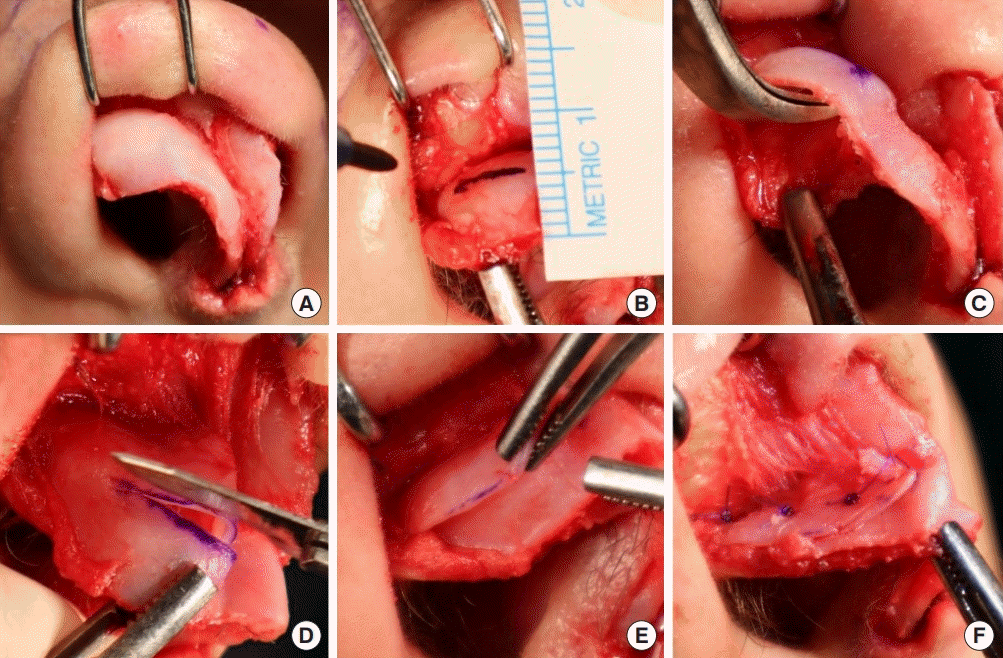
In nasal tip surgery, the cephalic lateral crural advancement (CLCA) flap narrows the tip and strengthens both the internal and external nasal valves. It also increases tip rotation, supports the lateral nasal wall, and allows medialization of the tip-defining points. Among the procedures on the LLC, the CLCA flap, which is a manoeuvre protecting the three-dimensional structure of the nose can result in more aesthetically favorable and natural-looking nose outcomes without performing excisions and using cartilage grafts.
DISCUSSION
This study aimed to investigate the effects of dissecting the LLC from the vestibular skin and mucosa and using a CLCA flap without performing cephalic trimming of nasal tip rotation. Using this manoeuvre, we also reconstructed bulbous nasal tips and supported both the internal and external nasal valves while preserving the scroll area.
Nasal tip surgery is a challenging and complicated part of rhinoplasty. The major component of nasal tip surgery formation of an aesthetic LLC. In LLC surgery, each cephalic trimming manoeuvre can—in the long term—pose possible risks for pinched nasal tip deformity, loss of tip rotation, collapse of the internal and external nasal valves, unnatural and aesthetically unfavorable results in the supra-alar area, and weakness and deformities in the alar rim. Thus, to narrow the nasal tip, we should not perform radical excision because manoeuvres involving cephalic trimming excisions could lead to the formation of dead spaces around the surgical field. In the long term, these dead spaces may cause re-draping of the skin, which may lead to unnatural nasal tip definition (e.g., undesired shadows in the supra-alar crease) and sometimes a decrease in tip rotation. Surgical techniques that would recover the three-dimensional anatomy of the nasal alar and tip regions would advance protective nasal tip surgery as well. With our CLCA flap technique, one can support the alar rim and prevent drooping of the nasal tip and the formation of dead spaces.
Nasal tip size, shape, and position are determined by the length, width, and strength of the lateral crus. It has been reported that a nose with concave lateral crus and convex domal segment of the middle crus provides a more aesthetic domal junction and domal outline [
9]. In nasal tip surgery, the position and shape of the lateral crus play a major role in terms of functionality and aesthetics. The lateral crus plays an important role in the appearance of the borders of the alar rim. Functionally, the LLC is an important component of the external nasal valve, which forms the first section of the nasal airway and supports the internal nasal valve. Preservation of the ligament complex in the scroll area of the lateral crus that connects the LLC to the ULC is a vitally imperative consideration in nasal tip surgery. Our CLCA flap technique was able to increase the strength of the LLC by keeping the scroll ligament complex intact.
Toriumi and Checcone [
4] emphasized the necessity of understanding the harmony between the external nasal contour and the components under the tip. Their statement underscores the significance of preserving the contours of the lower lateral crura. If they are not adequately preserved, it is likely there would be a pinched nasal tip, and in some extreme cephalic trimming cases, intervention may lead to alar collapse. Therefore, for many patients, a preventative alar batten graft medial to the supra-alar line is advised to avert the collapse of the lateral nasal wall after cephalic trimming. Our CLCA flap technique does not employ any cephalic trimming, so we did not require a cartilage graft to support the lateral nasal wall.
Gruber et al. [
10] emphasized the importance of preserving the lateral crura and cephalic part of the LLC in surgery sparing with LLC and its cephalic portion. In modern rhinoplasty, the role of cephalic trimming of the LLC is questionable in terms of its long-term outcomes [
11]. Cephalic trimming damages the scroll area, and in the long term, it may cause unsuccessful recovery of the scroll area, formation of scars, loss of support on the cartilage and ligament junction, and adverse results over the nasal tip area [
12].
Sheen [
13] first described the cephalic malposition of the LLC as bulbosity, boxy nasal tip deformation, and parenthesis-shaped tip deformity from the frontal view. In general, cephalic malposition results in supratip swelling and a bulbous nasal tip. Furthermore, it may frequently cause loss of alar support, resulting in external nasal valve collapse, which may lead to alar retraction. Cephalic malposition of LLCs may result in alignment of the nasal tip with the medial canthus rather than the lateral canthus. The anatomical angle of the LLC to the midline must be 45°, but cephalic malposition decreases the angle to 30°. Cephalic trimming is not a physiological manoeuvre for repositioning the LLC in primer rhinoplasty. It has been reported that repositioning of bulbous and cephalic malposition of the lateral crus can be achieved by cephalic trimming, dissecting from the vestibular skin, and adding a strut graft below the lateral crura [
14]. Our CLCA flap technique allows lateral crural rotation in patients with cephalic malposition. This technique achieves better nasal tip definition without performing additional excisions and cartilage grafts.
The lateral crural spanning suture technique has been suggested to repair the convexity of the lateral crura [
15]. In patients with weak cartilage, dome sutures may progress to pinched nasal tip deformity because of the disturbance of the normal lateral crural convexity. The tightness of dome sutures and rigid crura promotes pinched nasal tip formation.
The CLCA flap is a manoeuvre to be used in patients with lateral crural convexity. The lateral crural mattress suture technique has also been defined for the correction of lateral crural concavity. Studies have suggested that cephalic trimming and dissection of the LLC from the vestibular skin can be applied to bulbous and cephalic malpositioning of the lateral crura [
16].
Dome sutures decrease the concavity deformation of lateral cartilage in most of the concave LLC cases, but these sutures lead to the displacement of the caudal border of the lateral crus. The cephalic part of the lateral crus can be pulled inferiorly, but sometimes using just a few sutures may be inadequate. Furthermore, it may be compulsory to apply a lower lateral crural strut graft. Both in the short and long terms, these manoeuvres mostly end up as pinched nasal tip deformity.
The CLCA flap technique enables crural rotation and avoids such problems in extreme concavity or convexity and cephalic misposition of the lower lateral crura, without demanding additional sutures or cartilage grafts. If there is wide lower lateral crus on the vertical plane, the CLCA flap can be adopted. Even if wide lower lateral crura seem oriented normally in the anatomical position, some supratip fullness would still be present on the lateral view. Although cephalic trimming lessens supratip fullness and the width of the LLC in the vertical plane initially, it may lead to poor nasal tip definition in the long term.
There should not be excessive intrusion on the LLC in thin-skinned patients because LLCs may lose their strength, thereby making the lateral nasal walls weak. This could lead to the emergence of deformations of the alar rim. Studies have reported that disproportionate resection of the lateral crura to achieve better nasal tip definition, especially in thick-skinned patients, causes multiple complications. Some of these complications include tip asymmetry, external nasal valve failure, alar failure, drooping nasal tip, and tip definition loss [
17]. Weak lower lateral crura cause both adverse functional and aesthetic outcomes. Studies have suggested that weak lateral crus of the alar cartilage may evolve into alar rim concavity and even alar rim (external nasal valve) collapse [
18]. When applied to thin and weak lateral crura, the CLCA flap supports the lower lateral crus by advancing the cephalic flap over the LLC.
Thanks to recent cadaveric studies, the relationship between the lower lateral crura and the surrounding tissues has been better understood. A study of turn-in folding of the cephalic portion of the lateral crus with weak and ineffective alar parts emphasized the importance of not trimming the cephalic part of the LLC [
19]. After that, the cephalic turn-in-the-flap technique was defined [
20]. These two techniques were later modified [
21]. A study described the superior-based transposition flap as not involving cephalic excision, and fixing the flap harvested from the cephalic part of the LLC over the rest of the LLC [
22]. The difference of our CLCA flap technique from the superior-based transposition flap is that in addition to the cephalic part of the LLC, the lateral crus is also separated from the vestibular skin. The advantage of the CLCA flap technique is that it allows rotation of the lateral crus in the cephalic direction together with the cephalic flap. Therefore, the CLCA flap contributes to cephalic rotation of the nasal tip. This manoeuvre also allows the lateral crus flap and cephalic flap to be clamped on each other effortlessly.
The scroll ligament complex that acts as a gliding joint between the LLC and the ULC has been verified in recent cadaveric studies. This complex is mainly formed by ligaments and cartilages, but it also contains a deep layer of the superficial musculoaponeurotic system and perichondrium [
23]. This arrangement supports both the internal and external nasal valves by securing the unity of the ULC and LLC. Our CLCA flap technique protects the scroll ligament complex, allowing a gliding action between the LLC and the ULC. It enables three-dimensional control by preserving the scroll ligament complex in the nasal tip.
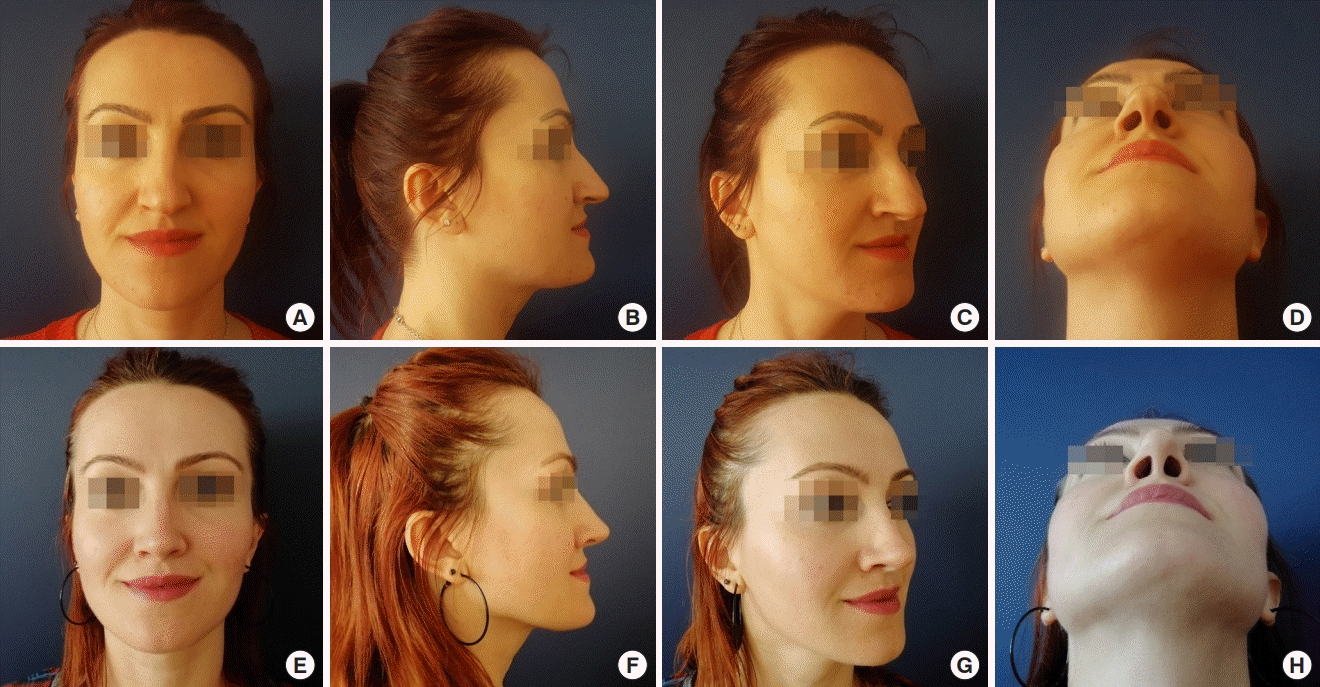
The CLCA flap, also known as the preservation of the nasal tip manoeuvre, has proved to be an important technique in rhinoplasty. It is an effective and controlled manoeuvre to position the lateral crura. This study presented several advantages of the CLCA flap. In summary: (1) the LLC can be strengthened; (2) it is possible to eliminate extreme concavity or convexity of the LLC without using a cartilage graft and extra sutures; (3) nasal tip rotation improves; (4) the CLCA flap provides aesthetic wing contours; (5) the scroll area is preserved; (6) the internal and external nasal valves are supported; or (7) nasal tip definition improves.
In conclusion, the CLCA flap technique preserves the connection between cartilages, representing the functional anatomy and supporting the internal and external valves without cartilage excision. We believe that this technique is a valuable modern preservation rhinoplasty technique. By applying the CLCA flap technique in nasal tip surgery for suitable candidates, we hope to achieve more natural, aesthetic, and functional results. The main limitation of this study is that operations were performed by one surgeon only, with a limited number of patients, and a longer follow-up period would be required. Further studies with a higher number of cases and longer follow-up periods would provide a better understanding of the efficiency of the CLCA flap technique.