RESULTS
The average age of the 10 patients was 42.4 years (range, 2–61 years) with eight men and two women. All injured fingers were crushed and had Allen classification type 3 amputations with significant exposure of the distal phalanx, as well as defects in both the nail bed and pulp area [
6]. Of the 10 fingers treated, there were two thumbs, four index fingers, and four middle fingers. Eight patients received the subcutaneous flap as an initial operation due to the absence of the amputated segment, and two patients underwent this flap surgery as a secondary operation due to necrosis after replantation (
Table 1). Fractures of the distal phalanx were present in two cases.
All flaps survived and all composite grafts were successful. Two cases of tuft fractures healed well. We examined the shape of the pulp area and nail growth, and the average follow-up was 11.2 months (range, 4–27 months). The recipient and donor sites healed without any significant complications. Although the donor site usually had a subungual hematoma in the immediate postoperative period, none had significant morbidity during long-term follow-up. The nails of all patients did not have any serious deformity such as nail ridge, split nail, pterygium, or hooked nail, except for one patient (patient no. 5) who had loss of almost the entire nail bed and distal phalanx after replantation failure. The outcomes of nail growth were excellent in five patients (50%), very good in four patients (40%), and fair in one patient (10%), in accordance with Zook’s criteria (
Table 2) [
7].
Case 1
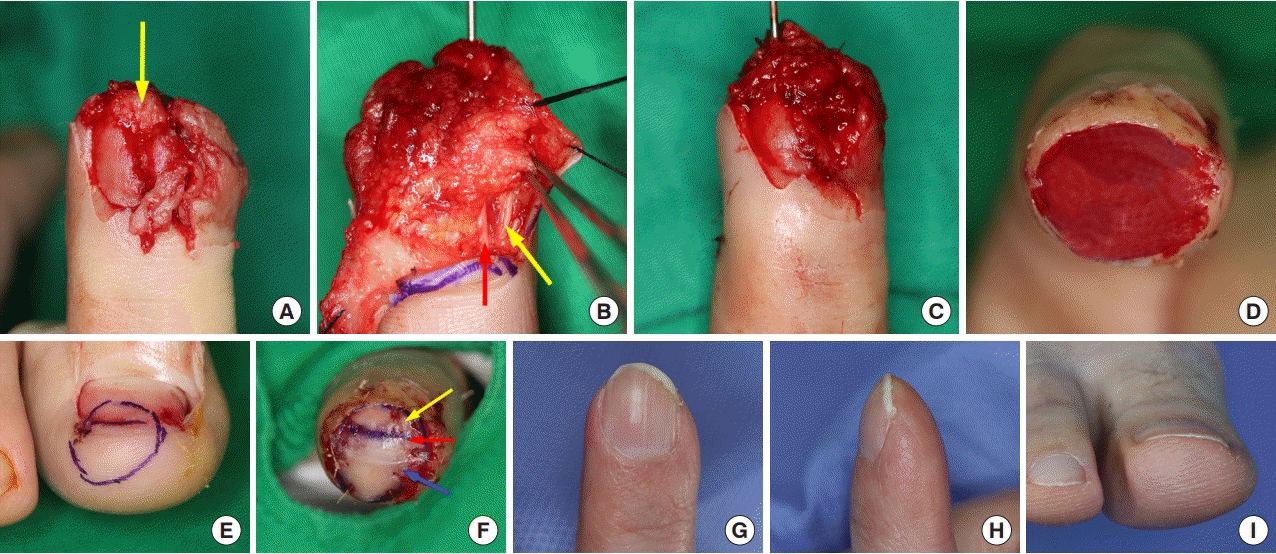
A 50-year-old woman presented with amputation of her left index finger by a press machine. The amputated segment was small and severely crushed, and we decided to operate with a subcutaneous flap for the exposed distal phalanx. She underwent composite graft surgery 3 weeks later. At a 27-month follow-up, a minor variation of the shortened nail was observed, and the nail was graded as “very good” (
Fig. 2).
Case 2
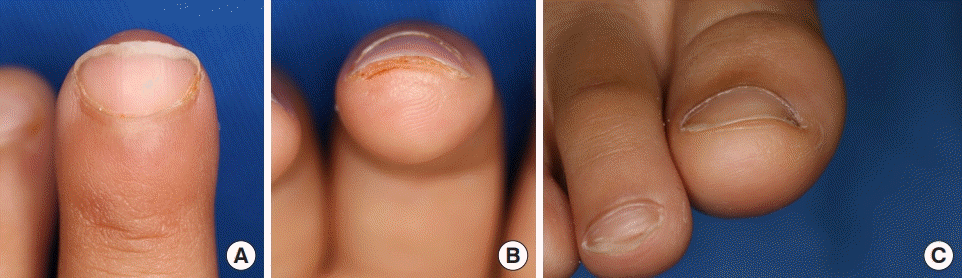
A 5-year-old boy was involved in a horse bite accident, leading to necrosis of the right middle fingertip. After debridement, a soft-tissue defect of the fingertip was observed with an exposed distal phalanx. A subcutaneous flap was applied, and a subsequent composite graft was performed 3 weeks after flap surgery. At a 12-month follow-up, the new nail was graded as “excellent” (
Fig. 3A).
DISCUSSION
Fingertip injuries are among the most common hand injuries regardless of age, as the fingertip is a prominent and frequently used part of the hand [
1,
2]. However, no consensus yet exists regarding the ideal reconstruction of fingertip injuries with nail bed defects, and its reconstructive methods are limited.
Fingertip injuries are managed according to the Allen classification as follows [
6]: (1) Type 1 has only a pulp defect without nail bed and bone exposure. If the amputated segment is present, a composite graft is the treatment of choice. If not, secondary healing is usually an adequate option; (2) Type 2 has both nail bed and pulp defects, but without bone exposure. If the amputated segment is present, the treatment depends on the shape of the defect. For the transverse type, acceptable options include various local and regional flaps, such as the thenar flap, Moberg flap, volar V-Y advancement flap, bilateral V-Y advancement flap, and cross-finger flap [
8-
11]. However, if the shape is oblique, a free flap is recommended; (3) Type 3 has an exposed distal phalanx as well as both nail bed and volar pulp defects. In these cases, replantation or flap surgery is required.
Although conventional fingertip reconstructions such as the volar V-Y advancement flap and the Moberg flap are often applied in cases of transverse amputation over Allen classification type 3 injuries, the Moberg flap is difficult to apply for fingers other than the thumb [
8,
9]. Additionally, although the bilateral V-Y advancement flap is suitable for central fingertip defects owing to its limited bilateral advancement, postoperative pain is one of the worst complications related to fingertip scars [
10]. These conventional flaps may not be ideal reconstructive methods for nail bed defects.
After the development of acellular dermal matrix (ADM), nail bed reconstruction with ADM and a split-thickness skin graft (STSG) were recently introduced [
11]. Although this method has certain advantages, including minimal functional deficits and donor site morbidity, it may not be suitable for complex crush trauma patients. It also cannot be applied to large defects or volar pulp defects with bone exposure.
Several methods of reconstruction exist for nail bed and volar pulp defects with an exposed distal phalanx. A nail bed graft is possible for the nail bed over the bone. If the nail bed defect is small, a nail bed graft over the bone can be done. However, if the defect is larger, graft survival tends to be low due to the presence of less viable vascularity over the exposed bone [
12,
13]. A nail bed graft cannot be used to reconstruct a volar pulp defect; therefore, it is only an option for the dorsal side of the exposed distal phalanx.
Microvascular toenail transfer involves the transfer of a composite of nail and a finite portion of pulp from the toe. It can be applied from partial to full defects of the fingertip. However, its indications for nail reconstruction are relatively rare, and it requires advanced microsurgical techniques [
14].
Lee et al. [
15] introduced a thin thenar fascial flap for coverage of exposed bone with subsequent nail bed grafts. The fascial flap provides a healthy wound bed for nail bed grafting. However, this method may induce joint stiffness due to immobilization before flap division.
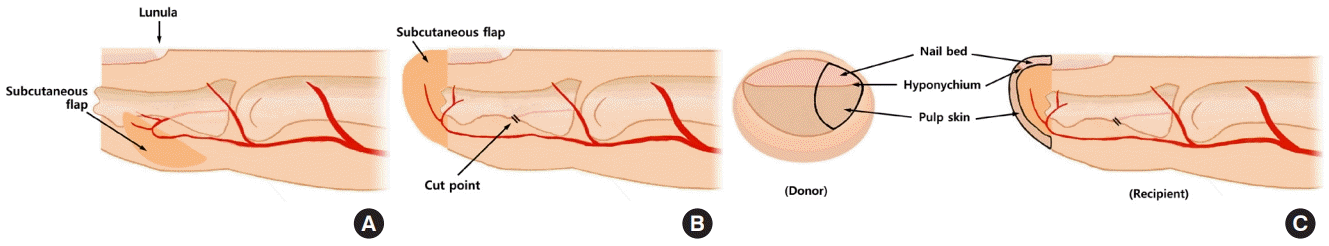
Thus, we propose a subcutaneous flap to cover the exposed distal phalanx and a composite graft composed of nail bed, hyponychium, and volar skin. The composite graft was taken from the fibular hyponychial side of the great toe to decrease irritation around the donor site when patients wore their shoes. The donor site healed by secondary intention in the first four cases. However, the patient complained of pain during dressing of the donor site; therefore, we used an additional STSG from the fibular side of the big toe. The thin STSG was used as the donor for the composite graft in the last six cases. This was done to achieve faster healing of the donor site of the composite graft and to reduce pain.
The present study has limitations in that it included a relatively small number of cases. It is expected that the subcutaneous tissue of the donor site will be reduced after transposing adjacent volar tissue to the defect site. Four patients complained of insufficient volume of the volar pad compared to normal fingertips. However, no patients reported experiencing pain in the reconstructed finger that caused discomfort in daily life. We suggest that this is because the incision of the subcutaneous flap was on the lateral side (i.e., the non-pinching side of the finger), unlike the volar V-Y advancement flap.
The subcutaneous flap from the adjacent tissue covered the exposed bone sufficiently and became a good recipient bed for the nail bed graft. The reconstructed hyponychial fold is natural because the composite graft was harvested from the nail bed, hyponychium, and pulp skin of the big toe as one piece (
Table 2). If the graft is done with an STSG only, excluding the nail bed graft, the possibility of hook nail deformity may be high. While the nail bed was harvested at a depth equal to that of the defect, the volar pulp skin was harvested with a sufficient thickness to contain some subcutaneous tissue. This reconstruction does not require long-term immobilization and minimizes major complications, such as shortened nail, hook nail deformity (
Figs. 2G,
3A), and a bulky volar pulp. These techniques require a relatively short learning curve as they are not microsurgical procedures.
The subcutaneous flap was obtained from tissue adjacent to the injured tissue without extensive sacrifice. The donor scar was minimal and was not distinguishable from a traumatic scar (
Figs. 2H,
3B). The composite graft required a small and thin volume of tissue from the great toe. No donor site morbidity and minimal scarring was observed in the great toe (
Figs. 2I,
3C).
A subcutaneous flap and composite graft fitting the defect shape could constitute a new reconstructive paradigm for fingertip injuries with nail bed defects and distal phalanx exposure.