Many plastic surgeons work for years trying to prevent the aging process of their patients and improve the age-related appearance of the face by using various injectable agents including synthetic and autologous agents and to search for an ideal soft tissue filler. A review of fillers in 2007 described an ideal filler material as biocompatible, non-antigenic, non-toxic, easy to use, long-lasting (yet not permanent), inexpensive, and reversible. Its safety profile should be high, and a predictable result should be achievable [
7]. Facial autologous fat transfer has become one of the most popular methods for facial rejuvenation because fat possesses many qualities of an ideal filler, including its lack of immunogenicity, relatively low cost, abundant donor-tissue availability, and ease of harvesting [
8]. However, the notable problems that have limited its widespread acceptance are the unpredictable absorption rates causing contour irregularities, which require multiple repetitions of the procedure, potential dissipation of the transplanted fat, and the risk of lumps and bulges along thin skin areas such as the periorbital area [
8,
9]. Some studies report 20% to 50% postgrafting resorption commonly observed with autologous fat grafting [
9]. Several substances such as growth factors, beta blockers, insulin, and hyperbaric oxygen, and even the combined use of adipose-derived stem cells and platelet-rich plasma synergistically supplement fat grafts, increasing revascularization and fat graft survival, improving cosmetic facial contouring, and decreasing complications [
10]. Recently, Levi et al. [
11] demonstrated that lymphedema-associated adipose-derived stem cells have a much higher adipogenic gene expression and enhanced ability to undergo adipogenic differentiation compared to control adipose-derived stem cells. Alghoul et al. [
12] demonstrated in an experimental model that the mixing of HA with the fat graft can potentially improve early fat graft survival and thus, enhance vascularity and prolong fat volume maintenance. This demonstrates the ability of LF to last for a long period of time, and patients, even after many months of the procedure, are satisfied with the results. HA is an important component of the extracellular matrix, which is synthesized in the interstitial tissue, transported in the lymph, and catabolized mainly in lymph nodes and the liver. HA acts by binding water molecules, resulting in increased skin hydration and turgor. Its hydrophilic properties help with volume maintenance and tissue viscoelasticity. HA, since 1996 when it was launched in the European market, was utilized as a filler agent for improving wrinkles and scars, or increasing the tissue volume, and has since become the "gold standard" for fillers [
13].
Recently, in a clinical investigation, Liu et al. [
2,
3,
4] found that the hyaluronan content in the interstitial fluid of the lymphedematous limb is significantly higher than that of a normal limb. These data further validate the use of an LF graft
in vitro by using an experimental model [
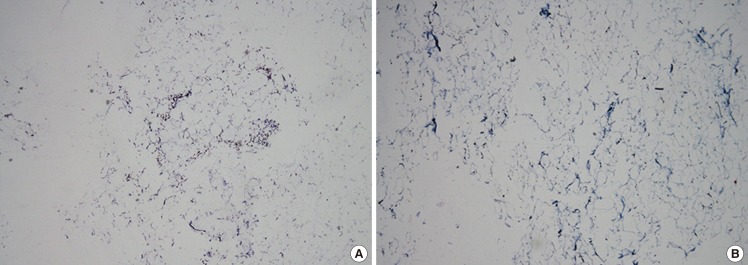
14]. We performed a histological analysis of the harvested LF (as shown in
Fig. 3B), which in accordance to the literature and in comparison to the normal fat harvested from the abdomen (
Fig. 3A), demonstrates the presence of a large quantity of collagen, elastin, and adipocytes. The LF tissue contains high levels of HA and is rich in precious anti-aging molecules. Furthermore, recent experimental studies have shown that lymphatic fluid stasis results in a subcutaneous fat deposition and that this effect is associated with increased adipocyte number, lipid accumulation, and fibrosis [
15]. Therefore, lymphedematous patients have available a large amount of fat to harvest and are rich in HA and stem cells with a high adipogenic potential that can be used for different clinical purposes.
This study demonstrated a clinical application of LF as an ideal autologous injectable filler easily available in patients with lymphedema. This method could be rightly offered to lymphedema patients simultaneously with other surgical or non-surgical interventions in order to boost their quality of life. Furthermore, we recommend the further study and investigation of this tissue having important properties and qualities for future clinical applications and research.