DISCUSSION
Physiological and mechanical factors contribute to an ideal wound dressing. Optimal healing can be achieved by maintaining a moist wound environment to avoid desiccation, prevent infection, and reduce inflammation. A moist wound environment encourages the migration of enzymes, cytokines, growth factors, and white blood cells to the site of healing [
10]. Mechanical factors include ease of handling, the presence of an avenue to allow drainage of effluent, being non-adherent to the wound bed in order to minimize trauma during removal, and the ability to conform adequately to the wound surface. An ideal wound dressing should also be able to retain its position at the wound site, and should be able to withstand sterilization processes [
11]. There has yet to be a single wound dressing that is able to provide all the factors necessary for an ideal wound-healing environment.
Mepitel has most of the characteristics of an ideal wound dressing and served as the control for our experiment. It is a polyamide silicon wound dressing with extensive applications. It has been used in traumatic wounds, chronic wounds, burns, and fixation of skin grafts [
12]. It has been shown to increase the rate of granulation and re-epithelialization. The adequate drainage of exudates from the wound bed is achieved with pores (1.2 mm, 14 per cm
2) that span the dressing. It has the added advantage of being non-adherent to wounds, minimizing wound trauma and pain during dressing changes [
13].
The application of Mepitel over concave surfaces such as the groin and axilla is difficult [
14]. The high cost of Mepitel is also another disadvantage [
14]. In our experience, Mepitel has tended to adhere strongly to gloves and surgical instruments, making it difficult to handle. Mepitel could be improved by decreasing its thickness, making it lightweight, and increasing its flexibility. This would make it more suitable for facial wounds and wounds over skin creases. Modifying its adhesive properties to prevent adherence to gloves and instruments would also be an advantage. The development of a dressing without these pitfalls while retaining the superior characteristics of Mepitel would be ideal.
PCL has been utilized as an ultra-thin film for dressing cutaneous wounds and as a delivery vehicle for gentamicin sulphate [
2]. It possesses the advantages of being stable in ambient conditions, inexpensive, and readily available [
3]. PCL has been shown to possess excellent mechanical strength and has the ability to prevent contamination by microorganisms due to its thin geometry [
7]. The inflammatory response, which leads to scarring, is minimized because of decreased foreign material implantation.
HyA plays a major role in facilitating wound healing. The foetal skin contains a large amount of HyA, facilitating wound healing without scar formation [
15]. HyA provides a hydrophilic extra-cellular environment, which facilitates the migration of mesenchymal, epithelial, and inflammatory cells to the site of healing [
16]. The autolytic debridement of the wounds is enhanced by enzymes secreted from white blood cells [
17]. This prepares the wound for the repair phase. The present growth factors stimulate re-epithelialization and fibrous tissue deposition. The inflammatory response of wound healing is also shortened with HyA [
4], allowing rapid advancement into the remodelling phase. This translates into a faster rate of healing with reduced scarring. HyA also stimulates the production of TNF-alpha and increases cellular mitosis, promoting tissue growth and angiogenesis [
18].
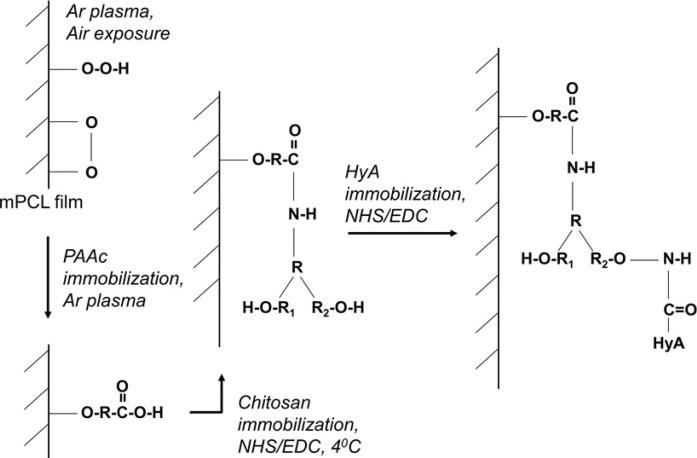
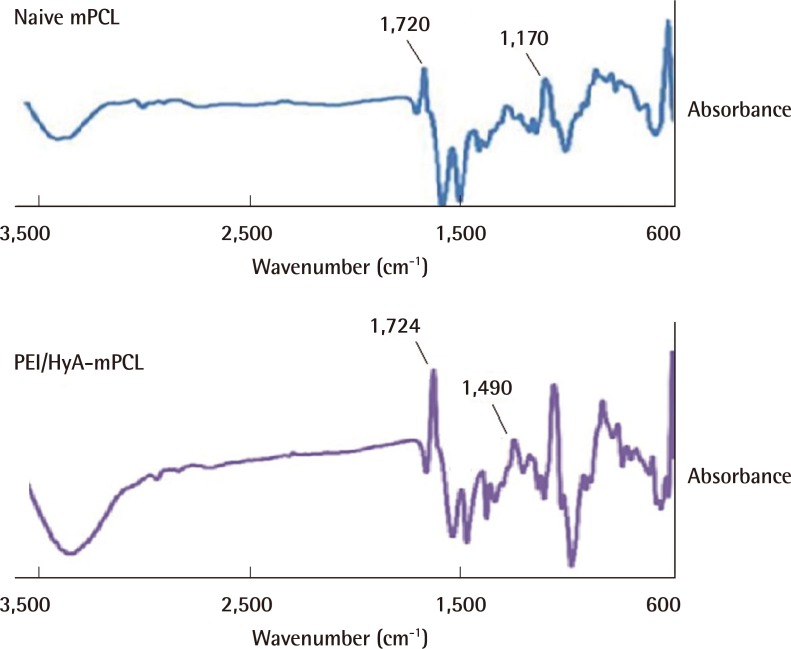
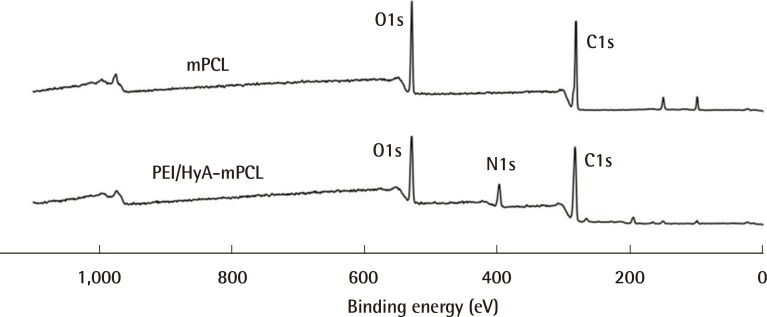
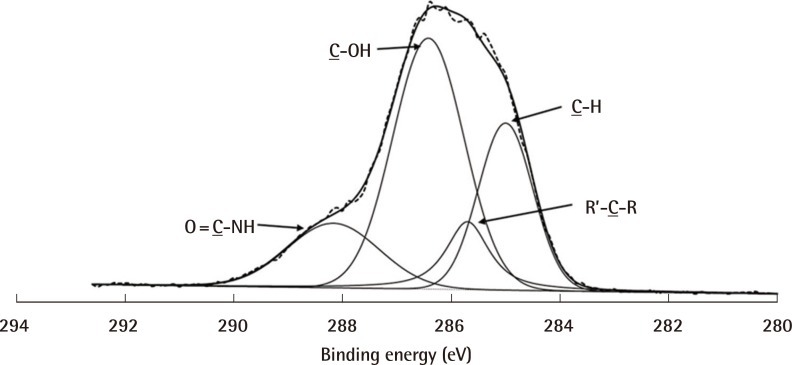
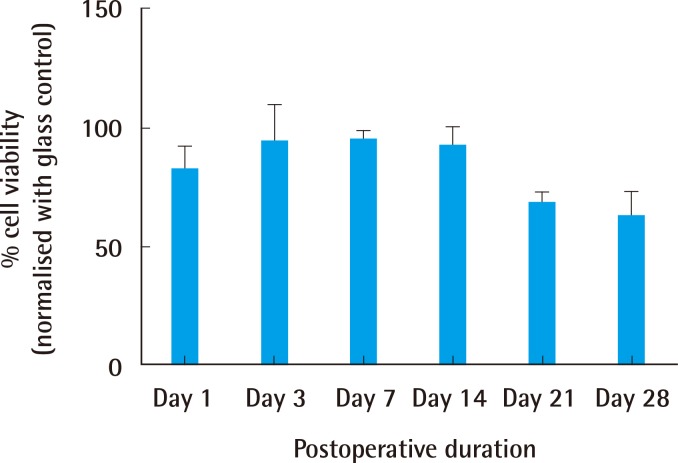
HyA has the ability to create an ideal environment to facilitate wound healing. A major drawback is its poor mechanical strength. This can be overcome by chemical modification and cross-linking. We have successfully surface grafted HyA onto PCL using our novel surface modification technique. This has equipped HyA with enough strength to serve as a wound dressing. PCL was chosen as the carrier primarily for its excellent mechanical strength and biocompatibility. Plasma-induced surface bioconjugation enables the manipulation of the surface chemistry of membranes. This allowed PCL to be used as a scaffold for the engraftment of HyA. HyA was proven to be present on the surface of our bio-conjugated PCL membrane using the PEI method of grafting. The membrane was shown by our in-vitro study to be cytocompatible (with cell viability of more than 70%) when evaluated with human dermal fibroblast cells.
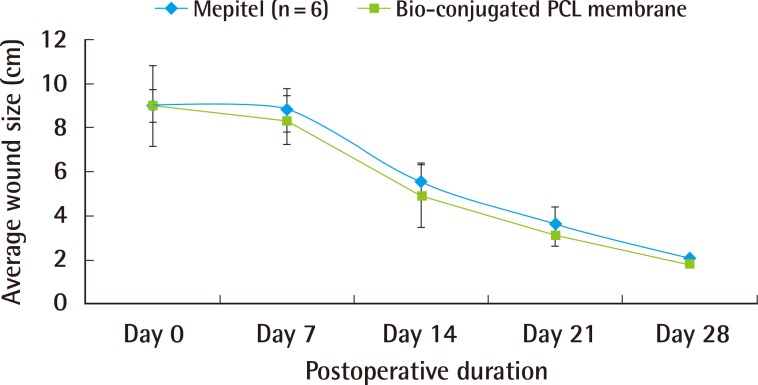
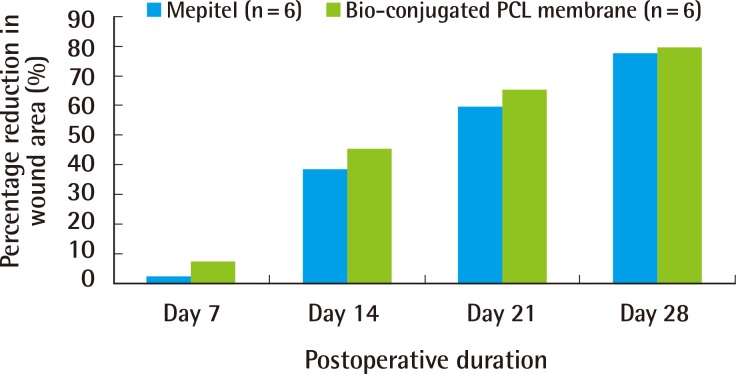
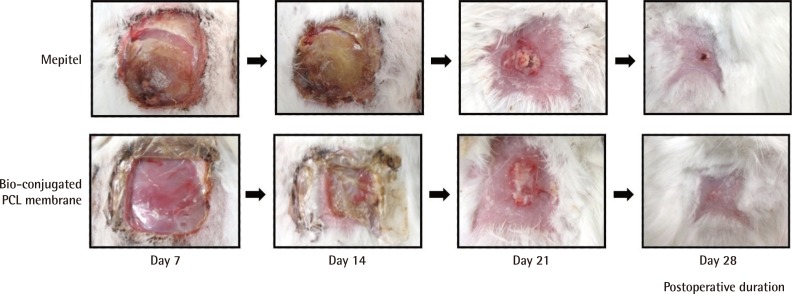
Our study showed that a bio-conjugated PCL membrane was capable of bringing on the healing of a full-thickness wound, comparable to Mepitel. The bio-conjugated PCL membrane was biocompatible and did not elicit any local or systemic inflammatory reaction. Scarring was minimal by the end of the study. Bio-conjugated PCL also has the advantage of being non-adherent to the wound, similar to Mepitel. This would minimize trauma to the wound site and pain during dressing change.
Mepitel has its disadvantages, as stated above. We engineered the bio-conjugated PCL membrane to overcome the limitations of Mepitel. Bio-conjugated PCL exhibited a greater ease of handling compared to Mepitel. It did not stick onto gloves or surgical instruments, and did not crumple during dressing application and change. Being an ultra-thin membrane (thickness of 10-30 µm), it conformed better to the contours of the wounds. This would likely lead to greater ease of handling during application to a concave wound surface. It also has the advantage of being lightweight, providing greater patient comfort. A lightweight dressing should also reduce traction on the surrounding skin and reduce friction during wound healing. Being fully bioresorbable makes the bio-conjugated PCL membrane an ideal dressing for chronic wounds. It is degraded via hydrolysis over a period of 1 to 2 years, depending on the amount implanted [
19]. It can be left at the wound site without removal or dressing change, minimizing trauma to the wound. Only the secondary absorbent dressing needs to be changed regularly.
Compared to Mepitel, the bio-conjugated PCL membrane also has the added advantage of retaining exudate at the wound site. Wounds treated with bio-conjugated PCL membrane showed a greater extent of exudate collection beneath the dressings, filling the surface area of the wound. Exudate from an acute wound creates a moist wound environment necessary for the diffusion of enzymes, cytokines, growth factors and the migration of cells necessary for wound healing. It also contains nutrients for cell metabolism and facilitates autolytic debridement [
20].
However, excessive exudate might impede wound healing. The surrounding skin can be macerated. Physical and psychosocial morbidity could also arise. Dressings may also have to be changed more often, placing additional stress on health care resources [
21]. Exudate from chronic or infected wounds would also impede wound healing. Exudate from these wounds contains proteolytic enzymes that cause the breakdown of growth factors and the surrounding skin, and also increases inflammation [
20].
We have observed from this experiment that exudate from wounds dressed with bio-conjugated PCL drained from the margins into the secondary layer of gauze. The extent of exudate retention could be reduced by creating pores in the membrane. Wounds with excessive discharge will have to be dressed adequately with a secondary absorbent layer such as gauze. Desiccated exudate that had collected was removed by rubbing the area with moist cotton balls.
One of the major drawbacks of Mepitel is its cost. PCL has a relatively lower cost of production compared to other aliphatic polyesters and is widely available [
22]. HyA is also readily available by means of microbial biosynthesis [
23]. The cost of fabricating bio-conjugated PCL membranes as described above is low, and the fabrication process is relatively simple. This allows us to offer the market an effective yet economical dressing.
Wound infection causes significant morbidity and mortality, and is also a financial burden for hospitals. Up to 38% of hospital acquired infections are caused by wound infections [
24]. A sterile dressing is necessary to prevent wound contamination and subsequent infection. Terminal sterilization and aseptic processing are possible methods for sterilizing bio-conjugated PCL membrane. Gamma irradiation and low temperature hydrogen peroxide gas are feasible methods for terminal sterilization. Steam sterilization is not recommended, as it will affect the structural integrity of PCL [
25].
Future advances in bio-conjugated PCL membranes would include the incorporation of anti-inflammatory and anti-bacterial agents for infected wounds. Being light-weight and ultra-thin, it is ideal for facial wounds and wounds over skin creases, providing maximal comfort for the patient. Having the ability to retain moisture, it can be used for wounds with low production of exudates or desiccated wounds. HyA has been shown to reduce adhesion formation in the peritoneal cavity. In addition to being a wound dressing, bio-conjugated PCL membrane has the potential to be used as an anti-adhesion membrane following abdominal surgery.
Bio-conjugated polycaprolactone membranes are comparable to Mepitel as a safe and efficacious wound dressing. They have the factors necessary to create an optimal environment for wound healing. Compared to Mepitel, they have the added advantage of being bioresorbable, ultra-thin, and light-weight, and also have better handling qualities.