DISCUSSION
In this series of patients with medium to large elbow defects, the goals of stable internal fixation and durable skin coverage were achieved by collaboration between the orthopaedic and plastic surgeons. Successful coverage allowed early aggressive joint mobilisation.
Orthopaedic fixation was used to treat bony and soft tissue injury, and soft tissue coverage was performed when the wound was deemed clean and free of infection. Elbow fractures were reduced and internally fixated with preservation of articular congruity using devices such as the 3.5 mm reconstruction plate, 3.5 mm low contact dynamic compression plates as well as anatomical locking plates e.g., proximal ulnar locking compression plates. Successful operative treatment depends on restoring joint congruency (especially the ulnohumeral joint) and elbow stability, so that early joint motion is possible [
5]. Dead space at the fracture site can be a problem if the implants do not conform exactly to the bone surface or if there is a bone gap. A well vascularised muscle can fill the dead space and reduce the risk of infection.
Many local and pedicled flaps have been described for elbow reconstruction. Local flaps are indicated for small defects with healthy adjacent skin. Common designs include rotation flaps, transposition flaps, and perforator based island flaps. However, they cannot be used if there is extensive degloving injury. Pedicled flaps such as the radial foream, ulnar forearm, antecubital fasciocutaneous, and posterior interosseous flaps have been used, however, the disadvantages are extensive scarring and the need for skin grafting over the forearm. Muscles such as flexor carpi ulnaris, brachioradialis, and anconeus can be elevated to provide coverage of small areas but at the sacrifice of some limb function [
6]. The pedicled latissimus dorsi flap is a traditional workhorse flap for coverage of large elbow defects, especially proximal to the olecranon. When used for defects beyond the olecranon it has a propensity for distal tip necrosis, wound breakdown or failure [
2]. Free flaps are indicated for large defects distal to the olecranon [
7].
Although free tissue transfer has become increasingly popular, it has not been emphasised sufficiently for elbow coverage. The English literature contains relatively few reports on its use. Hallock used five local fascial flaps and three free flaps for elbow coverage in his series of upper extremity trauma [
6]. He advocated using local flaps for mild injuries but maintained that free flaps were necessary in larger or composite defects. Choudry et al. [
2] reported using free tissue transfers in only 19% of cases in their series of 96 patients requiring soft tissue coverage of the elbow. Of the 19 free flaps, only five (26%) were ALT flaps, with the latissimus dorsi being the flap of choice (42%). This may stem from the perception that the vascular supply of the ALT flap is unreliable, although recent studies have defined its vascular anatomy and proven the flap's reliability [
8,
9]. Other than the ALT flap, perforator flaps including the thoracodorsal artery perforator [
10-
12] and superficial circumflex iliac artery perforator [
13] flaps offer reliable skin cover.
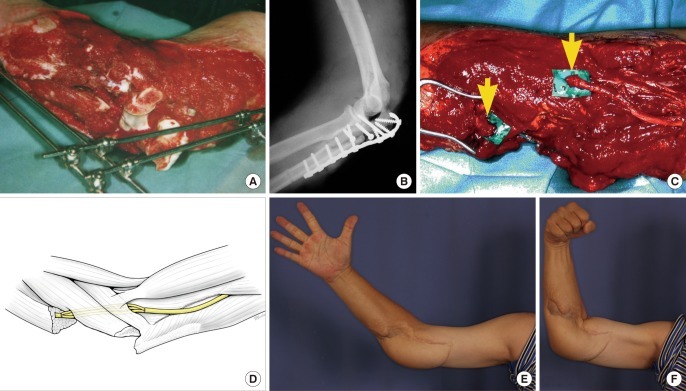
The ALT flap is ideal for elbow coverage. It can provide large amounts of skin (up to 35 cm long and 25 cm wide can be harvested on a single dominant perforator [
14]) as well as vastus lateralis muscle, which can be used to obliterate dead space and combat infection. Furthermore, vascularised muscle helps to vascularise the sural nerve grafts [
15,
16] and optimise outcome as seen in case 1. The motor nerve to the vastus lateralis could potentially be used as a vascularised nerve graft [
17]. Even if the motor nerve is harvested, or the vastus lateralis muscle is included in the flap, donor site morbidity is acceptable and studies have shown that all patients eventually return to their preoperative level of function [
18,
19].
Fascia lata grafts are easily harvested at the time of flap elevation and can be used to reconstruct the triceps tendon (case 4) or elbow ligaments. Primary closure of the donor site is possible if the skin paddle is ≤7 to 9 cm wide [
14], but the donor site is skin grafted if a larger skin paddle is needed. The skin paddle should cover the vascular anastomoses and be sufficiently large to accommodate the hardware and allow the elbow to move freely. Since the donor site is located a distance from the elbow, harvest of the flap can proceed concurrently with the other elbow procedures. A thin flap can be obtained by elevating in a suprafascial plane [
20] or by trimming of the subcutaneous fat to the subdermal level [
21,
22]. The skin paddle of the ALT flap allows fast skin-to-skin healing at the interface between the flap and the wound edge and its subcutaneous tissue allows gliding between the joint and skin.
Loss of movement after injury to the elbow is common. Sojbjerg [
1] defined a stiff elbow as one with flexion of less than 120° and a loss of extension of greater than 30°, Morrey et al. [
23] found that most tasks of daily living can be performed with 100° of elbow motion (from 30° to 130°). All of our patients displayed ≥100° of elbow flexion except for patient 1, who had elbow flexion of 45° (range, 45° to 90°). Although his elbow was stiff, he had excellent ulnar nerve recovery and declined further surgery.
The causes of posttraumatic elbow stiffness are varied and can be classified as intrinsic or extrinsic. Heterotopic ossification, as occurred in patient 1, is the most common cause of extrinsic elbow contracture and it is characterised by progressive ossification of periarticular soft tissues [
24]. Operative release of the stiff elbow depends on the aetiology but usually involves release of the posterior band of the medial collateral ligament, debridement of any bony blocks to motion and/or anterior and posterior capsulectomy [
25]. Total elbow arthroplasty may be considered in selected cases [
25]. The ALT skin paddle affords skin-to-skin healing and facilitates secondary surgery of the elbow.
In conclusion, the advantages of the ALT flap for elbow coverage are 1) abundant skin and subcutaneous tissue; 2) vascularised vastus lateralis muscle that can be used to obliterate dead space, provide a vascular bed for nerve grafts and combat infection; and, 3) access to fascia lata grafts for triceps tendon repair.