As the quality of rehabilitation has improved (e.g., through the increased use of wheelchairs), ischial sores have become one of the top 3 most common types of sores in terms of location, with an annually increasing number of patients [1]. Even after musculocutaneous or perforator flaps are performed to treat pressure sores, complications such as ulcer recurrence and wound dehiscence still remain common [2].
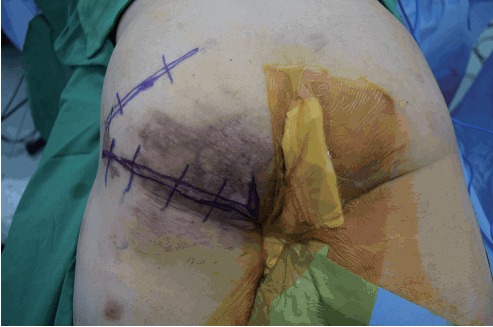
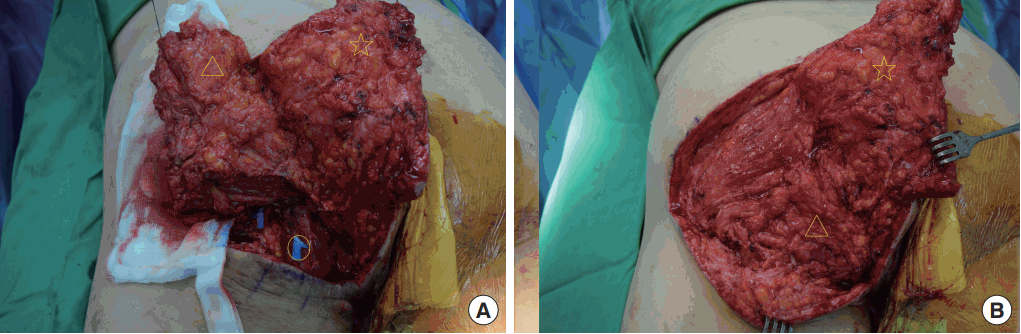
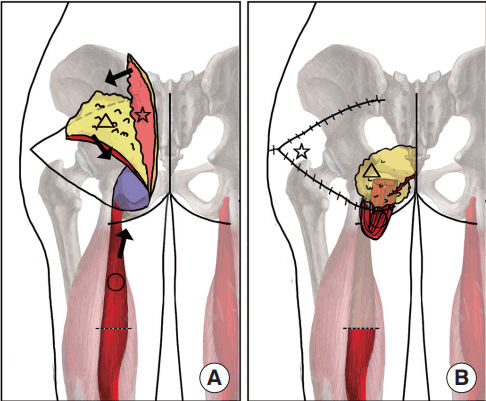
A 48-year-old man underwent surgery to treat a lumbar spinal cord tumor in 2003. In 2005, due to his bedridden state, he experienced a left ischial sore. In the same year, he was treated with bursectomy, a rotation flap, and a local flap. After a rehabilitation period that allowed him to ambulate and sit, the ischial sore recurred in 2017. After treating him with negative-pressure wound therapy, we performed a bursectomy, packed the dead space with a semitendinosus muscle flap that had no effect on the patient’s ambulatory ability, and covered the skin area with a local flap. However, after surgery, we observed abrasions and seroma in the ischial region (Fig. 1). To fix this problem, we performed a complete bursectomy, repositioned the semitendinosus muscle flap to apply more padding to the ischial tuberosity, packed the remaining dead space with an inferior gluteal artery pedicled adipofascial flap that did not involve muscle [3] to maintain the patient’s ambulatory ability, and covered the skin using a V-Y advancement flap (Figs. 2, 3).
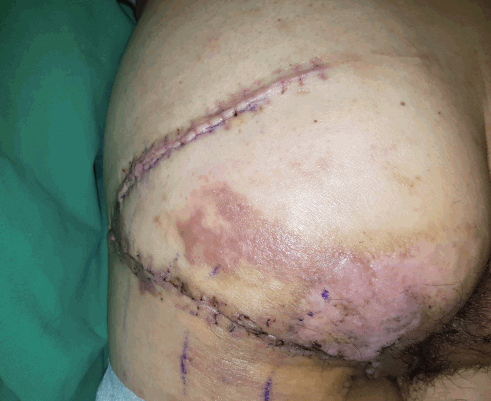
Considering the patient’s ambulatory ability and the shortage of tissue due to the recurrence of the sore, we believe the usage of the 3-flap technique presented above was an appropriate treatment (Fig. 4). Thus, we must consider each patient’s condition and the availability and efficacy of various tissue types to increase the diversity of flap reconstruction.