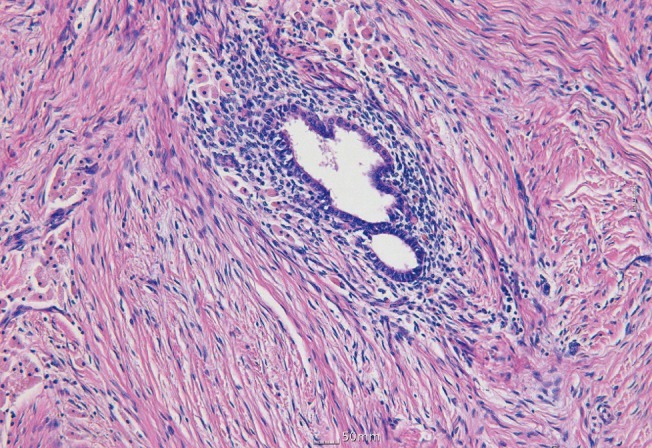
In endometriosis, functioning endometrial gland and stromal tissue is present outside the uterine cavity, and this causes various clinical symptoms because it proliferates under the influence of female hormones [
1-
3]. The ovary is the most commonly affected site, and the pelvic cavity is the usual location, but the intestine, appendix, gall bladder, pancreas, kidney, ureter, urinary bladder, vagina, perineum, and peritoneum can also be involved [
5]. Surgical scar endometriosis involves the incision sites on the abdominal wall, laparoscopic port, perineum, and Bartholin cyst; among them, the incidence of Cesarean scar endometriosis is 0.03% to 0.4% [
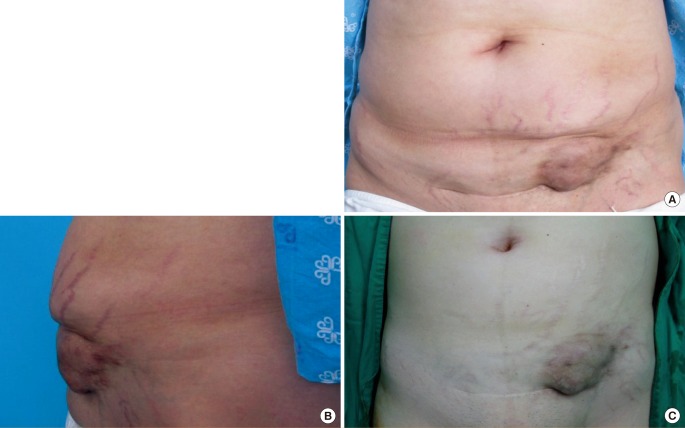
6]. Patients with endometriosis often complain of menstrual pain, dyspareunia, chronic pelvic pain, and infertility. In surgical scar endometriosis, tenderness of the operation site, or a non-tender nodule and periodic pain and bleeding corresponding to the menstrual cycle could be present, as in this case. Differential diagnoses for a mass on a surgical scar are hernia, primary or metastatic tumor, lymphoma, sarcoma, lipoma, abscess, sebaceous cyst, and suture granuloma [
2,
3]. History taking and physical examination are always the most important procedures for the diagnosis. A nodule on a surgical scar in a reproductive female patient with a prior history of pelvic or intra-abdominal surgery suggests the possibility of surgical scar endometriosis, especially for a lesion with periodic pain on menstruation. The average onset time for surgical scar endometriosis is 30 months after surgery (frequently reported in the literature to be postoperative 1 to 2 years) [
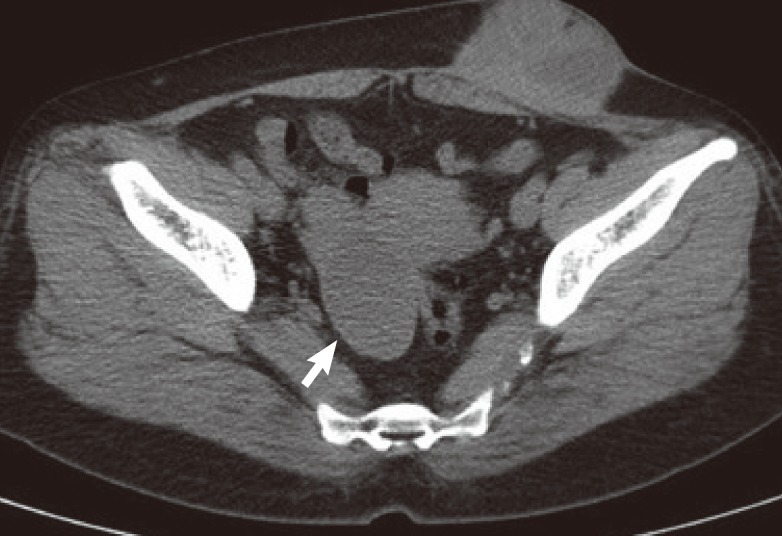
7], but it should not be a strict rule because even in this case, ten years had passed before the development of the tumor. Other diagnostic tools including computed tomography, magnetic resonance imaging, fine needle aspiration biopsy, and serum CA-125 could be helpful [
3,
5]. Medication such as a combined oral contraceptive, progesterones, danazol, gonadotropin-releasing hormone agonists, aromatase inhibitors, and androgens can be used for decidualization, atrophy of endometrial tissue, and relieving pain, but recurrence after cessation of medication makes surgical resection the treatment of choice [
8-
11]. The authors had performed conservative excision on 8×7.5×6 cm Cesarean scar endometriosis, saving the musculoaponeurotic layer; the defect was reconstructed using mini-abdominoplasty.
The present case highlights four points. First, this is a rare case report of extensive endometriosis. Second, scar endometriosis can be misdiagnosed as a malignant tumor, so plastic surgeons should keep in mind the possibility of cutaneous endometriosis in an abdominal mass of a reproductive female with a previous history of pelvic or intra-abdominal surgery. Third, though wide en bloc excision with a surrounding safety margin is the standard surgical method to prevent local recurrence of endometriosis as like a malignancy, the authors decided to perform conservative excision of the possible remnant tumor instead of wide excision in consideration of the benign nature of the disease and the low probability of recurrence with regard to the patient's age nearing menopause along with the simultaneous bilateral salpingooophorectomy. In our patient, the mass abutted and even penetrated the rectus abdominis, external oblique, and pyramidalis muscles and their fascia due to adhesion at the surgical site and frequent menstrual bleeding. If conventional wide excision were performed at the sacrifice of the musculoaponeurotic strut, an incisional hernia could have occurred in the lower abdominal wall, which lacked the posterior sheath of the rectus abdominis. Finally, we performed mini-abdominoplasty to avoid functional and cosmetic problems. The large defect after ablation of the tumor made the primary closure difficult and could cause various wound complications such as dehiscence, hematoma, seroma, and hypertrophic scar; asymmetry of the abdominal wall or dog-ear deformities could also occur. In mini-abdominoplasty, the dissection is limited to below the umbilicus, and a smaller amount of excessive skin and subcutaneous tissue is resected via a shorter incision [
12]. Through limited dissection, many complications associated with full-abdominoplasty such as hematoma, seroma, necrosis of skin flap, and umbilicus and malposition of the umbilicus can be reduced. The application of mini-abdominoplasty made the patient satisfied with eradication of both the tumor and lower abdominal obesity without any of the problems associated with primary closure or full-abdominoplasty.