INTRODUCTION
Wound healing is a physiological response in which various elements are combined and work together. The proliferative phase of the wound healing process is significant, since it is the stage in which granulation tissue grows from the wound bed to fill the defect and different types of cells interact with biochemical factors, including growth factors and enzymes, to assist tissue regeneration. Proper wound management is essential for wound healing. In the past, the concept of wound management was limited to the role of absorbing exudates, cleaning the affected area, and sealing the wound. More recently, many therapies that facilitate spontaneous healing at the cellular and molecular levels have been introduced [
1].
A biomaterial is defined as a natural or synthetic non-drug substance that replaces or augments a certain function, while maintaining contact with tissue and fluids [
2]. Silver-based foam products (Mepilex Ag; Mölnlycke, Gothenburg, Sweden), sutures for wound closure (Surgical Gut Suture; Ethicon, Somerville, NJ, USA), and porcine dermis biomaterials (EZ Derm; Mölnlycke) are representative examples of biomaterials. The characteristics required for biomaterials used in wound management include nontoxicity, a minimal foreign body reaction, natural degradation, and function at a molecular level [
3].
Human acellular dermal matrix (ADM) is a biomaterial that has been shown to be useful in tissue regeneration and wound healing and is actively used in clinical practice (Alloderm; LifeCell Corp., Branchburg, NJ, USA).
Previously-identified mechanisms through which ADM affects wound healing include scaffolding for granulation tissue formation [
4], inclusion of receptors for fibroblast attachment [
5], angiogenesis stimulation [
6], function as a chemoattractant of vascular endothelial cells [
7], and inclusion and protection of growth factors [
8]. Although ADM is commonly used in the form of a thin sheet, it has recently been used in a micronized form because of its ease of handling and ability to be used in various types of wounds. In clinical cases where a micronized ADM was applied to chronic pressure sores and sinus tract wounds, it resulted in an improvement in the size and depth of the wounds [
9-
11].
CG Paste (CG Bio, Seongnam, Korea), used in this study, is a paste-type micronized ADM that is currently used safely in clinical practice. It is a type of biomaterial and bio-absorbable wound dressing that is applied to open wound areas, including external wounds and chronic ulcers. There are disadvantages when micronized ADM is applied using the conventional method as a dressing (Cymetra, LifeCell Corp; GRAFTJACKET Xpress, KCI USA, Inc., Austin, TX, USA; CG Paste, CG Bio). For example, it easily detaches, can become a source of infection, and does not have an adequate healing effect. In this regard, we speculated that injection of CG Paste into the wound bed would make it less likely to detach and be a source of infection and could facilitate wound healing by creating a dynamic environment within the wound.
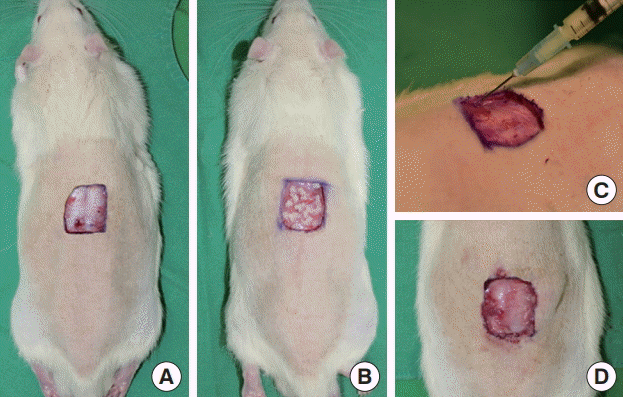
In this experiment, we first performed a biocompatibility test in white rats to rule out problems that could occur during off-label use of this product. The model was designed so that CG Paste would be injected into the subcutaneous layer of the skin surrounding a full-thickness skin defect. Ultimately, the present study aimed to investigate the effect of the subcutaneous injection of ADM on wound healing in full-thickness skin defects in white rats.
DISCUSSION
The comprehensive concept of a wound includes lacerations, punctures, amputations, abrasions, and surgical wounds, which are often encountered in reconstructive surgery. When a wound is left open and expected to heal without surgical treatment, it is called wound healing by second intention or secondary union. A dressing is a means of helping wound healing by secondary intention. An ideal wound dressing keeps the wound clean, with adequate wetting, protects the affected area from pressure and physical impact, reduces edema, and is inexpensive. In addition, careful consideration should be given to the role of the dressing material suitable for the specific characteristics of the affected area (e.g., exudate absorbency, adhesion, bacterial inhibition, and debridement) and physical properties of the dressing (e.g., ointment, film, foam, and gel) [
13].
Although traditional wound management was limited to absorbing exudates and wiping out the affected areas, it has recently evolved to include the use of hyperbaric oxygen therapy, negative-pressure wound therapy (NPWT), stem cells, platelet-rich plasma, and biomaterials.
CG Paste is a biomaterial applied to wounds, and its clinical efficacy has recently been studied by several researchers in animal experiments and clinical trials. It is manufactured by combining a micronized ADM, which is produced by lyophilizing and pulverizing the ADM processed from human tissue, and a gelatin material derived from porcine skin, which is a biocompatible, water-soluble, natural polymer.
The main component of the micronized ADM has no immunogenicity, so there is no foreign body reaction when it is injected into the body, and it is known to induce migration of fibroblasts by providing an extracellular matrix, enabling it to survive as autogenous tissue [
14,
15]. ADM is known to help heal wounds through mechanisms such as acting as a scaffold for granulation tissue formation, providing receptors for fibroblast attachment, stimulating angiogenesis, functioning as a chemoattractant of vascular endothelial cells, and including and protecting growth factors.
Gelatin is a protein-based synthetic biomaterial. It is a denatured protein that is biodegradable, biocompatible, and non-antigenic. Gelatin is frequently utilized as a scaffold in tissue engineering and for a variety of purposes including compression sponges (e.g., Gelfoam, Pfizer; Surgifoam, Ethicon) for hemostasis [
16].
In contrast, when CG Paste is applied to the affected part of the body, as in its conventional use, there are disadvantages. For example, CG Paste can detach from the affected area and be smeared on the dressing foam material or drained together with the exudates in the case of NPWT. In addition, chronic open wounds, which are not responsive to dressing treatment, are less likely to have a widespread distribution of blood flow or growth factors in the wound bed [
17]. Therefore, it was thought that no matter how good a dressing material may be, topical application alone might have limitations in terms of stimulating the expression of growth factors and cytokines necessary for effective wound healing.
Therefore, we hypothesized that if CG Paste is injected into the subcutaneous layer of the wound bed, it would have a regenerative effect by allowing surrounding cells, including fibroblasts, to come into contact with the ADM, stimulating the expression of various growth factors and positively affecting collagen synthesis and microvessel neovascularization. Thus, since in matrix cell scaffold structures, various growth factors and cytokines play an important role in tissue regeneration, injecting CG Paste into the wound was expected to be more effective than topical application for forming an extracellular matrix.
A biocompatibility test was first performed to determine whether CG Paste caused a foreign body reaction when injected into the body of a white rat. Histological examination showed mild chronic inflammation rather than a foreign body reaction. This finding suggests that CG Paste can be used not only through the conventional method, but also by injection.
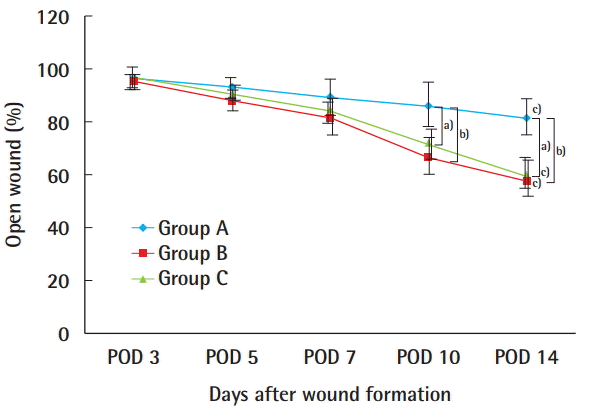
According to the results of the experiment, group C (the CG Paste injection group) showed a similar wound healing rate to that of group B (the CG Paste scrub dressing group), while group C was superior to group A (gauze dressing group) in terms of gross observations of the wound, suggesting that CG Paste can be used clinically by injection. As shown by BOTOX (Allergan, Irvine, CA, USA), the clinical use of a medical product may be modified in addition to its originally intended indications or usage.
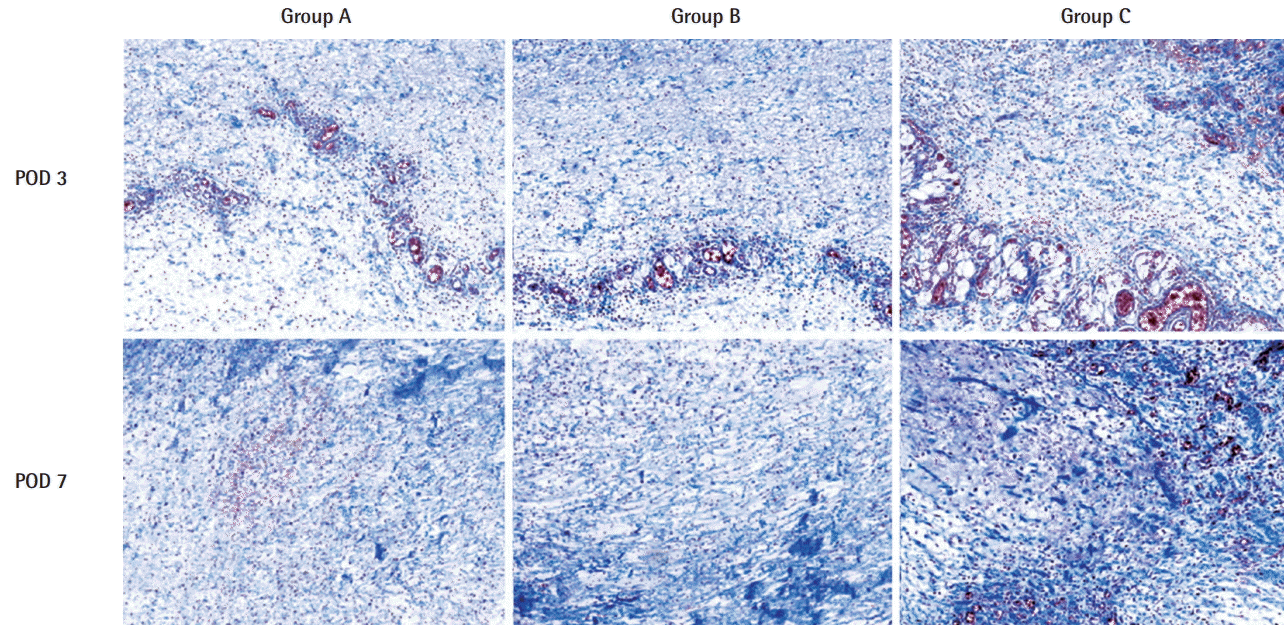
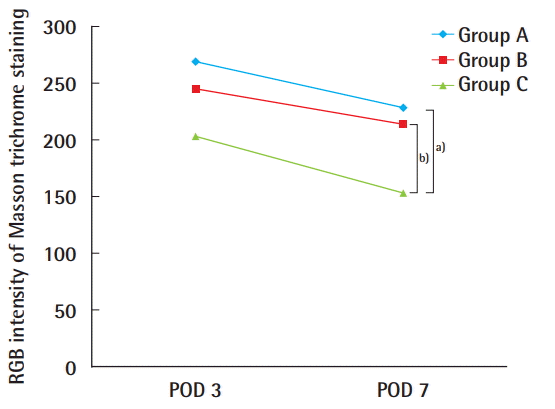
The histological examination using Masson trichrome staining revealed that more collagen fibers were formed in group C (CG Paste injection group) than in the other groups. Collagen was first applied as a biomaterial in 1881, and the familiar catgut suture (Surgical Gut Suture, Ethicon) is also an example of a collagen-rich biomaterial [
18]. Collagen fibers constitute most of the extracellular matrix in the body by forming a collagen fibril-based network, and simultaneously affect the migration and stimulation of various surrounding cells by forming well-organized, three-dimensional scaffolds [
19].
The presence of more collagen fibers in the experimental group suggests two clinical possibilities. First, the quality of wound healing may have improved through increased structural integrity of the extracellular matrix. According to this possibility, as the number of collagen fibers increases, the repaired tissue will be stronger and better able to withstand tensile forces, and the regenerated dermal layer will be strengthened through increased cross-linking between the fibers. Second, collagen fibers may dynamically increase the remodeling phase of wound healing by affecting the migration of surrounding cells, including fibroblasts. It is also worth noting that there are economic advantages of increasing the dynamicity of the remodeling phase (e.g., growth factor-based dressings and cell-based therapies, including stem cells) over existing therapies.
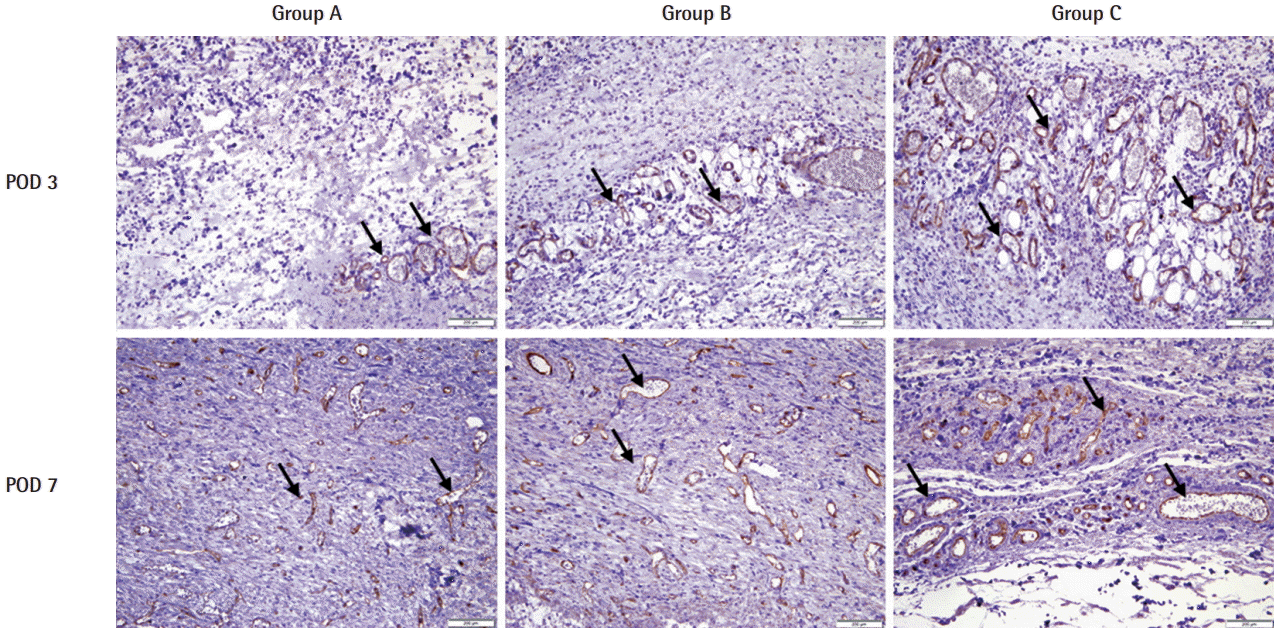
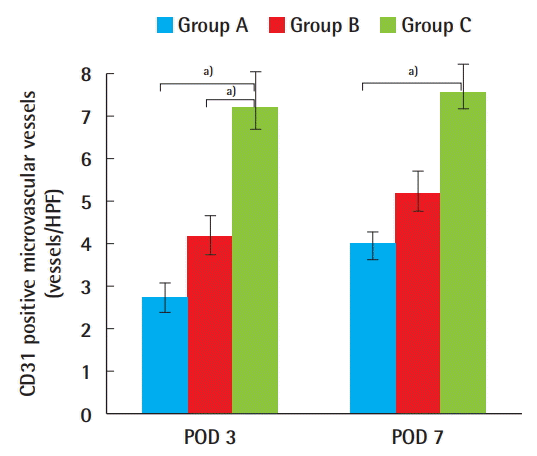
The MVD observed in the entire dermal layer of the wound margins was higher in group C (the CG Paste injection group) than in the other groups, which suggests the possibility of neovascularization. We think that a great deal of angiogenesis would have had to occur for the collagen fibers to be viable, and further investigations should be carried out to show the specific cells, growth factors, and pathways through which CG Paste injection induces angiogenesis.
In this study, we demonstrated that when CG Paste was injected into the subcutaneous layer of the wound margin, it enhanced wound healing, in contrast to the conventional method of applying CG Paste topically on the wound. This was confirmed by the fact that CG Paste injection was comparable to the conventional method with respect to the rate of wound recovery and by the results of the histological examination, which showed an increase in the amount of collagen fibers and MVD.