INTRODUCTION
Ectropion is a common problem seen by plastic surgeons in the clinic, and its adequate prevention and management are crucial. Ectropion is a medical condition in which the eyelid rolls away from the globe [
1]. Patients with ectropion typically complain of irritable dry eyes and symptoms such as epiphora, keratopathy, lagophthalmos, and pain [
2].
Ectropion is traditionally classified into three broad categories according to its pathophysiology: paralytic, cicatricial, and involutional [
3]. Paralytic ectropion is caused by a flaccid orbicularis oculi, resulting in loosening of the muscular sling that supports the lid against gravity. Gravity continuously pulls the lower lid downward, and it eventually rotates away. In cicatricial ectropion, a scar contracture or deformity formed by trauma on the anterior lamella acts as the main retracting force on the lower lid. Involutional (atrophic) ectropion, also known as senile ectropion, occurs when the aging process results in atrophy of muscular and tendon structures, and the lid becomes abnormally lax and falls away from the orbit.
However, we suggest that in addition to clinically evident ectropion, potential ectropion should also be managed in order to prevent it from manifesting. Some patients may have sufficient lid laxity to develop ectropion in the future, even if they do not present with overt features of ectropion. Furthermore, patients preparing to undergo procedures that can cause secondary ectropion should receive prophylactic treatment. Therefore, we developed a more practical and comprehensive categorization of ectropion.
Various surgical procedures are used to treat lower lid ectropion [
2,
4-
6]. By evaluating the types of ectropion preoperatively, the most appropriate technique for each patient should be selected and performed; however, there is no established surgical algorithm. Several previous studies have proposed approaches for lower lid ectropion, but they were generally based on the three types of ectropion in the conventional classification, and included procedures that are too extensive and aggressive [
7-
9].
For the comprehensive management of ectropion, we propose a simple algorithm based on a new classification of types of ectropion according to its signs and causes. This will help surgeons to classify and manage each type of ectropion with appropriate procedures.
DISCUSSION
The eye has an important impact on a person’s facial aesthetic features and impression. Patients with lower lid ectropion have scleral show due to lower lid eversion. An eye with scleral show can appear sad, tired, and somewhat impassive, which can be a frustrating experience for patients. It also causes lagophthalmos of the lower lid, leading to symptoms such as eye dryness, epiphora, irritation, pain, and keratopathy. Patients suffering from these symptoms should be appropriately treated.
This study proposes an algorithm that can help surgeons to manage ectropion in an easier and more logical way, in order to obtain effective results. To treat ectropion effectively, the most crucial task is to appropriately assess the cause and to classify the case as the correct type. The first step in the evaluation is to take a history from the patient and to examine the lower lid. Conventionally, ectropion is classified as paralytic, cicatricial, and involutional ectropion. However, based on our experiences, we also thought that it would be useful to consider the possibility of preventing potential or latent ectropion.
Some patients do not have evident ectropion features, but have sufficient lid laxity to develop future ectropion. Furthermore, patients who are about to undergo procedures such as lower blepharoplasty that can cause secondary ectropion should receive concomitant prophylactic treatment. Therefore, we classified cases of ectropion using a more practical and comprehensive categorization of current or present ectropion and potential or latent ectropion.
In general, the patients with latent ectropion tended to be elderly, and the majority of them had reduced lid tone, which can potentially cause senile ectropion. Moreover, they visited the clinic requesting lower blepharoplasty for rejuvenation, which in turn is the main cause of secondary cicatricial ectropion. Therefore, as a means of prevention, rejuvenation, and correction of mild senile ectropion, we propose performing routine combined orbicularis oculi muscle canthopexy with lower blepharoplasty. As the preseptal oculi muscle is suspended to the inferior part of the lateral orbital rim periosteum, the oculi muscle bunches up in the pretarsal area. This results in pretarsal fullness, and we were also able to achieve additional rejuvenation effects other than the basic effects of canthopexy, such as changing the canthal tilt more positively or tightening the lidcheek segment. This procedure was also reported to be effective in previous studies, one of which reported that the rate of postlower blepharoplasty lid malposition decreased from 10% to 1% after adopting the procedure [
10].
If there is no evidence of current ectropion, lid laxity should be assessed in order to determine the likelihood that the patient will develop ectropion. An anterior distraction of the lower lid exceeding 6 mm it is considered to be a severe degree of laxity, and the structure must be hung up more rigidly and durably in order to prevent recurrence. Anderson and Gordy first described the lateral tarsal strip canthopexy, and many surgeons have modified the procedure [
11,
12]. It has several advantages over other techniques. First, both lid laxity and excessive horizontal length can be corrected simultaneously. Second, it has the cosmetic advantage of maintaining the anatomical canthal angle. Lastly, rapid rehabilitation is possible, making it suitable for elderly patients who cannot visit the clinic frequently [
13].
Therefore, in patients with no evident ectropion, but only lid laxity, the lateral tarsal strip was used as the target of suspension. As a structure, it is fibrous enough to bear the force of suspension for a long period. Additionally, in patients with severe laxity, the horizontal length of the lower lid margin can be reduced through wedge resection.
In patients with evident ectropion, the displacement of the lid should be evaluated to determine the most appropriate next step. Malposition can be easily examined by comparing the location of the punctum with either the lower and upper eyelids or both lower eyelids. In cases of medial lid malposition, the caruncle is excessively exposed.
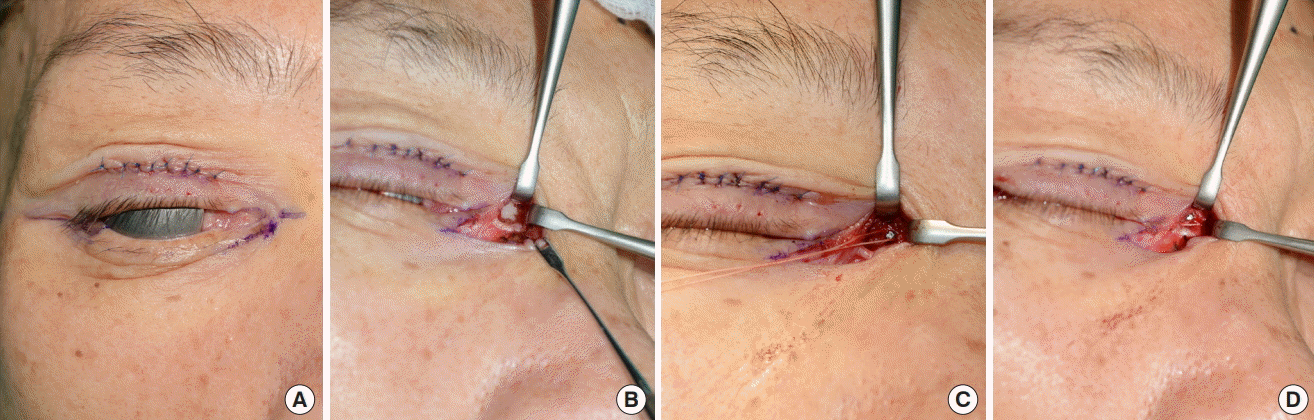
Present ectropion with lid malposition should be treated according to its pathophysiology. Generally, in cases with lid malposition, lamellar contracture is likely to be the main cause. Most such cases can be fully resolved without any additional grafts or flaps by releasing the contracture layer by layer. The structures comprising the lamella can be completely freed from the surrounding retracting tissues. However, if the anterior lamellar contracture is significant enough to result in a shortage of tissue, a full-thickness skin graft or local flap surgery should be considered to resolve the deficiency of the anterior lamella. For severe posterior lamellar contracture, a composite graft such as a palate mucosal graft should also be considered.
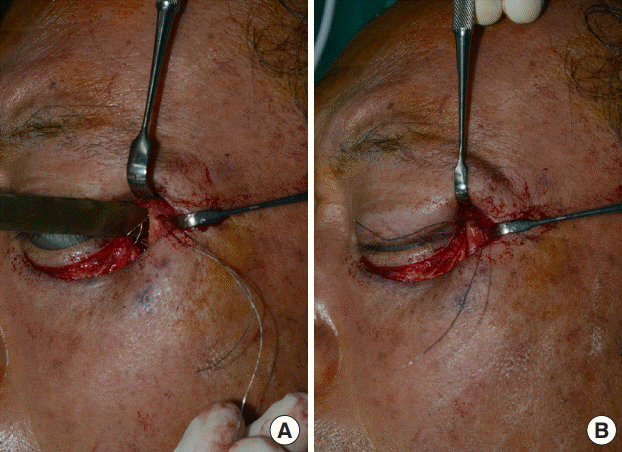
Despite the additional procedure to correct the lower lid deficiency, as time goes on, contracture can progress, resulting in recurrence of ectropion. Moreover, as the retracting forces are combined with gravity, more powerful tightening procedures should be used than for other types of ectropion. Thus, the structure used for suspension and the material used as the anchor should be more rigid and stronger. This can be achieved by drilling into the lateral orbital rim or using bone anchorage equipment [
6]. We passed a 1-0 steel wire through the drilled hole. The advantage of using the drilling method is that it can yield an even more superior-posterior vector to the lateral tarsal margin than the original lateral tarsal strip canthopexy method. Moreover, the lower lid becomes more inverted close to the orbit, preventing irritating ectropion symptoms. Although the most ideal anchoring spot is Whitnall tubercle itself, it is difficult to approach through a minimally extended subciliary incision. Drilling the lateral orbital wall makes it possible to pass the steel wire through the hole from the inner to outer aspect of the lateral rim, thereby anchoring the lateral tarsal end more medially, similar to the original position of Whitnall tubercle.
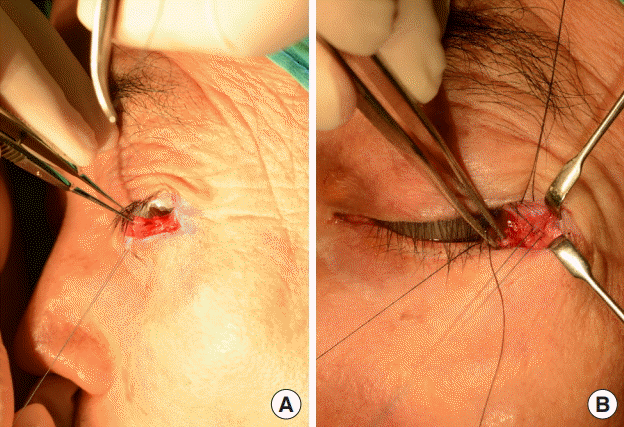
In patients with medial lid malposition, medial canthopexy should be performed. We suggest that the anchoring spot should be just superior to the medial canthal tendon insertion site. This is for the same reason as in lateral canthopexy; it allows the tarsoligamentous structures to be pulled up more medially and superiorly. For medial canthopexy, we used the Mitek anchoring system to make the procedure simpler and more effective. Considering the anatomy around the medial canthal tendon, drilling a hole for canthopexy is risky. Various procedures have been developed for medial canthopexy, of which transnasal canthopexy is particularly widely known. However, it requires an extensive incision for the approach and is technically difficult [
14]. We used a minimal incision for the approach; thus, we found that the Mitek Micro bone anchor system was an adequate alternative for anchoring fixation. The Mitek system is composed of a titanium alloy for anchoring onto the bone and two strands of Ethibond sutures with needles on the end. Several studies have reported that the Mitek suture anchor was advantageous for the correction of medial lid ectropion [
14-
17].
In addition to canthopexy procedures, other optional procedures can be performed. If a patient had been diagnosed with complete or unrecoverable incomplete palsy through electromyography, but had a responsive temporalis muscle, a facial reanimation procedure using temporalis transfer was performed along with canthopexy. Furthermore, if the patient had upper lid lagophthalmos or brow ptosis, gold plate insertion or a suprabrow lift using the frontalis suspension sling was performed together as combined surgery.
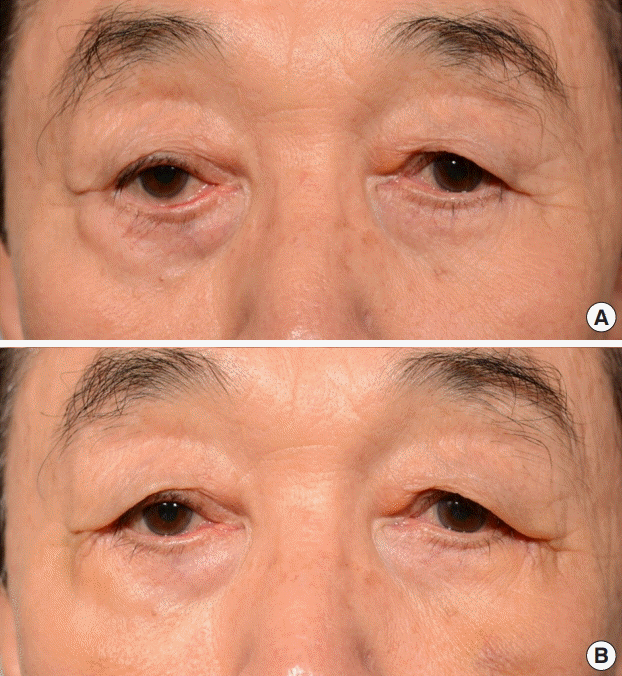
Patients were mostly satisfied with their aesthetic appearance after surgery. Prior to surgery, they were unhappy with their appearance, but after surgery, most of the patients had a score above 3 (satisfactory). Epiphora was the least improved symptom. It is presumed that even if the punctum is moved closer to the globe through the canthopexy procedure, in paralytic patients, it cannot be completely resolved because of a flaccid oculi muscle that cannot function as a lacrimal pump.
Almost all patients who visited our clinic desired the surgical procedure to be performed simply and quickly with local anesthesia. If there is no need for additional surgery, such as a facial reanimation procedure, it was possible to do so in an outpatient setting.
Although some studies have proposed algorithmic approaches for lower lid ectropion, most of them involved too extensive and aggressive procedures. Pepper et al. [
7] proposed an algorithm for paralytic ectropion management that included suborbicularis oculi fat pad lift, which involves extensive subperiosteal dissection of the infraorbital area. In the study of Fagien [
8], for some procedures in the algorithm, an additional upper transcutaneous blepharoplasty incision was necessary. In the algorithm proposed in the present study, no additional extensive dissection or incision was necessary for the canthopexy, and the procedures were effective, simple, and easy to perform.
For the adequate treatment and prevention of ectropion, it is important to decide what canthopexy procedures to perform. Medial and lateral canthopexy should be accurately adjusted. Through the suggested simple surgical algorithm in our study, both medically acceptable results and patient satisfaction were achieved without significant postoperative complications. Therefore, for management of patients with ectropion, the algorithm of this paper would be useful.